The 15 Us Cities With The Highest Rates Of New Hiv Diagnoses
A lot has changed since we last reported on the top 25 U.S. cities with the highest rates of HIV infection in 2013.
At the beginning of 2015, it was reported that 952,604 people in United States were living with HIV. According to the 2015 HIV Surveillance report from the Centers for Disease Control and Prevention, those living with the highest rates of HIV were African-Americans, who made up 44.3 percent of all cases, followed by Latinx Americans who represent 16.4 percent of those living with HIV, Asian-Americans at 5.5 percent, then Whites at 5.3 percent.
The highest age rate was for people between 25 and 29 . People between 20 and 24 were at 31.2 percent, and those over 65 made up 18 percent .
Men accounted for 81 percent of all HIV cases in 2015 722,244 males compared to 230,360 women. For men, 70 percent of transmissions were attributed to male-to-male sexual contact, 11 percent to injection drug use, 10 percent to heterosexual contact, and 7 percent to male-to-male sex and injection drug use. For women, 74 percent of cases were attributed to heterosexual sexual contact, 23 percent to injection drug use, and 2 percent to perinatal transmission.
Thanks to data collected by the CDC from city and state health records, we have learned the majority of the cities that have the highest HIV rates are in southerns states. In fact, the South attributed 13 out of the top 15 cities on our list. The state of Florida has the highest HIV rates across the country.
Hiv Infection And Aids 2016
The incidence of HIV/AIDS in Minnesota remains moderately low. In 2015, state-specific HIV infection diagnosis rates ranged from 1.9 per 100,000 population in New Hampshire to 29.2 per 100,000 in Louisiana. Minnesota had the 17th lowest HIV infection rate . In 2015, state-specific AIDS diagnosis rates ranged from 1.2 per 100,000 persons in Wyoming to 13.5 per 100,000 population in Louisiana. Minnesota had the 14th lowest AIDS rate at 3.0 AIDS cases reported per 100,000 population).
As of December 31, 2016, a cumulative total of 11,309 cases of HIV infection were reported among Minnesota residents. Of the 11,309 cases, 3,824 are known to have died. By the end of 2016, an estimated 8,554 persons with HIV/AIDS were assumed to be living in Minnesota.
The annual number of AIDS cases reported in Minnesota increased steadily from 1982 through the early 1990s, reaching a peak of 361 cases in 1992. Beginning in 1996, the annual number of new AIDS diagnoses and deaths declined sharply, primarily due to better antiretroviral therapies. In 2016, 131 new AIDS cases and 67 deaths among persons living with HIV infection were reported.
The number of HIV diagnoses has remained fairly constant over the past decade from 2006 through 2016, at approximately 269 cases per year. There was a peak of 280 newly diagnosed HIV cases in 2009, and 229 new HIV cases were reported in 2016.
- For up to date information see> > HIV
Impact On Communities Of Color
- Racial and ethnic minorities have been disproportionately affected by HIV/AIDS since the beginning of the epidemic, and represent the majority of new HIV diagnoses, people living with HIV disease, and deaths among people with HIV.36,37
- Black and Latino people account for a disproportionate share of new HIV diagnoses, relative to their size in the U.S. population .38,39 Black people also account for more people living with HIV than any other racial group â an estimated 479,300 of the 1.2 million people living with HIV in the U.S. are black.40
- Black people also have the highest rate of new HIV diagnoses, followed by Latino people â in 2019, the rate of new HIV diagnoses per 100,000 for Black people was about 8 times that of white people Latino people had a rate 4 times that of white people.41
- Black people accounted for close to half of deaths among people with an HIV diagnosis in 2019.42,43
- Survival after an AIDS diagnosis is lower for Black people than for most other racial/ethnic groups, and Black people have had the highest age-adjusted death rate due to HIV disease throughout most of the epidemic.44 HIV ranks higher as a cause of death for Black and Latino people, compared with White people.45 Further, HIV was the 6th leading cause of death for Black people ages 25-34 in 2019.46
You May Like: Can Chiropractors Help Ear Infections
Impact Across The Country
- Although HIV has been reported in all 50 states, the District of Columbia, and U.S. dependencies, the impact of the epidemic is not uniformly distributed.
- Ten states accounted for about two-thirds of HIV diagnoses among adults and adolescents in 2019 .30 Regionally, the South accounted for more than half of HIV diagnoses in 2019.31
- Rates of HIV diagnoses per 100,000 provide a different measure of the epidemicâs impact, since they reflect the concentration of diagnoses after accounting for differences in population size across states. The District of Columbia has the highest rate in the nation, compared to states, nearly 3 times the national rate and Georgia was the state with highest rate , twice that of the national rate.32,33 Nine of the top 10 states by rate are in the South.34
- New HIV diagnoses are concentrated primarily in large U.S. metropolitan areas , with Miami, Orlando, and Atlanta topping the list of the areas most heavily burdened.35
| Table 1: Top Ten States/Areas by Number and Rate of New HIV Diagnoses , 2019 | |
| State | |
| U.S. Rate | 13.2 |
| CDC. HIV Surveillance Report, Diagnoses of HIV Infection in the United States and Dependent Areas, 2019 vol. 32. May 2021. |
South Carolina Ranked With 9th Highest Hiv Case Rate In Us
COLUMBIA, S.C. – To raise awareness about the HIV-AIDS epidemic, South Carolina residents gathered at the State House to mark the 41st anniversary of World AIDS Day and honor those who have lost their lives.
Around 20,000 South Carolina residents are living with a diagnosed HIV infection, according to the state Department of Health and Environmental Control, the state is ranked ninth-highest HIV case rate in the country.
Dr. Shakaria D. Johnson, a physician consultant at the department, says, 84% of South Carolinians living with HIV are aware of their status. 88% are linked to medical care, and 70% have achieved viral suppression through ongoing treatment.
South Carolina residents gathered on Dec. 1 to show their support for those diagnosed. People learned about the resources available and were able to get tested. Undiagnosed people risk unknowingly transmitting the disease.
The department of health and environmental control says nearly half of all South Carolinians that have recently been diagnosed with HIV-AIDS are in their twenties.
MORE | Lanes open after multiple vehicle crash causes traffic delays on I-20
World AIDS Day is commemorated internationally each year, to raise awareness about the AIDS epidemic and remember those who have died from the disease and have been diagnosed.
Estoria Wright, a Columbia local and poet, says she was thankful to be among those gathered here every year, celebrating life including her own.
Copyright 2022 WRDW/WAGT. All rights reserved.
You May Like: Medicated Ear Drops For Ear Infection
Hiv Statistics By State 2022
Human immunodeficiency virus, or HIV, is a virus that weakens a persons immune system by attacking cells that fight off infection, specifically a persons CD4 cells. HIV is spread through body fluids such as blood. If HIV goes untreated and advances, it can lead to acquired immunodeficiency syndrome or AIDS. Unlike most other viruses, when a person contracts HIV, they have it for life because the human body cannot fight off the virus entirely. HIV, however, can be controlled and its progression can be slowed significantly. There are three stages of HIV: acute HIV infection, clinical latency , and AIDS.
Hiv In The United States
Currently, in the United States, over 1.1 million Americans are living with HIV. After years of stagnation in the annual infection rate, which hovered at around 50,000 new infections per year, the rate has begun to steadily drop in recent years due to newer preventive strategies like PrEP and HIV treatment as prevention, the latter of which can reduce the risk of HIV transmission to zero.
According to data from the Centers for Disease Control and Prevention , 37,968 new HIV infections were reported in the 2019 surveillancea drop of nearly 8% since 2010.
Despite these gains, around 15,800 people with HIV died in the United States in 2019, and as many as 14% of those infected remain unaware of their status. Of those who have been diagnosed, only 63% are linked to medical care, and only 51% are unable to achieve an undetectable viral load needed to ensure a normal to near-normal life expectancy.
HIV stigma and a lack of access to medical care, particularly among the poor and communities of color, are among the driving factors for these failures.
Recommended Reading: 8 Hour Infection Control Course For Dental Assistants
Key Points: Hiv Diagnoses
In 2020, MSM were the population most affected by HIV in the U.S.:
- In 2020, MSM accounted for 71% of new HIV diagnoses in the United States.f
- In 2020, Black/African American MSM accounted for 26% of new HIV diagnoses and 39% of diagnoses among all MSM.
- In 2020, Hispanic/Latino MSM made up 21% of new HIV diagnoses and 31% of diagnosis among all MSM.
- From 2016 to 2019, HIV diagnoses decreased 7% among gay and bisexual men overall. But trends varied for different groups of gay and bisexual men.
Transgender people accounted for approximately 2% of the 30,635 new HIV diagnoses in 2020.
- Transgender womeng accounted for 2% of new diagnoses.
- Transgender menh accounted for less than 1% of new diagnoses.
People who acquired HIV through heterosexual contact made up 22% of HIV diagnoses in the U.S. in 2020.
- People assigned male sex at birth who acquired HIV through heterosexual contact accounted for 7% of new HIV diagnoses.
- People assigned female sex at birth who acquired HIV through heterosexual women accounted for 15%.
- From 2016 to 2019, HIV diagnoses from heterosexual contact decreased 13% overall.
People who inject drugs accounted for 7% of new HIV infections in the U.S. and 6 dependent areas in 2020.
- Men who inject drugs accounted for 4% of new HIV diagnoses.
- Women who inject drugs accounted for 3% of new HIV diagnoses.
Blacks/African Americans and Hispanics/Latinos continue to be disproportionately affected by HIV:
States With The Highest Rates Of Hiv
These numbers are based on the CDCs HIV Surveillance Report.
California has the highest number of people living with HIV of 128,153, a rate of 389.7 people with HIV per 100,000 residents. Of those living with HIV in California, the largest group is White with 48,155 people and the second-largest is Hispanic/Latino with 48,029.
New York has the second-highest number of people living with HIV of 126,495, a rate of 760.2 per 100,000. This rate is more than double that of Californias. The largest group living with HIV in New York is Black/African American with 47,164 people living with the virus.
Florida has 110,034 people living with HIV, the third-highest number in the United States. Floridas HIV rate is 612.3 per 100,000. The group with the highest number of people living with HIV is Black/African American with 49,943.
Texas has the fourth-highest number of people living with HIV in the United States of 88,099, translating to a rate of 382.9 per 100,000 people. The largest group living with the virus is Black/African American with 31,915 people, followed by Hispanic/Latino with 29,758.
Georgia has 52,528 people living with HIV, a rate of 608.8 per 100,000. This is the fifth-highest in the country. A majority of those infected with the virus are Black/African American, totaling 35,974.
Here are the 10 states with the highest rates of HIV:
Read Also: Can Flagyl Cure Yeast Infection
Boxed Warning: Risk Of Drug Resistance With Use Of Descovy For Prep In Undiagnosed Early Hiv1 Infection And Post
- DESCOVY FOR PrEP must be prescribed only to individuals confirmed to be HIV negative immediately prior to initiation and at least every 3 months during use. Drug-resistant HIV-1 variants have been identified with use of emtricitabine/tenofovir disoproxil fumarate for HIV-1 PrEP following undetected acute HIV-1 infection. Do not initiate if signs or symptoms of acute HIV-1 infection are present unless HIV-negative status is confirmed
- Severe acute exacerbations of hepatitis B have been reported in individuals infected with hepatitis B virus who discontinued products containing FTC and/or TDF and may occur with discontinuation of DESCOVY®. Closely monitor hepatic function with both clinical and laboratory follow-up for at least several months in individuals with HBV who discontinue DESCOVY. If appropriate, anti-hepatitis B therapy may be warranted
Cities With The Highest Hiv Rates
Around 1.1 million people are living with HIV in the United States of America . Nearly one in seven of these people are unaware they have HIV.
The size of the HIV epidemic is relatively small compared to the countrys population, but is heavily concentrated among several key affected populations. Around 70% of annual new HIV infections occur among gay and other men who have sex with men , among whom African American/Black men are most affected, followed by Latino/Hispanic men.
Heterosexual African American/Black women and transgender women of all ethnicities are also disproportionately affected.
Now, before we begin, across the world, here are the top 10 Countries with the Most HIV Cases :South Africa 7,800,000
While the USA may not be in the top 10 across the world, the United States is the greatest funder of the global response to HIV. But dont forget that the U.S. does have an ongoing HIV epidemic, with approximately 36,801 people receiving an HIV diagnosis in the United States and dependent areas.
HIV affects locations in the U.S. differently as well, so weve compiled the cities with the highest rates in the nation . Looking at these cities, youll find that many of them have a large Black population, significant issues with poverty, and are geographically located in the South.
You May Like: What Antibiotics Are Prescribed For Kidney Infection
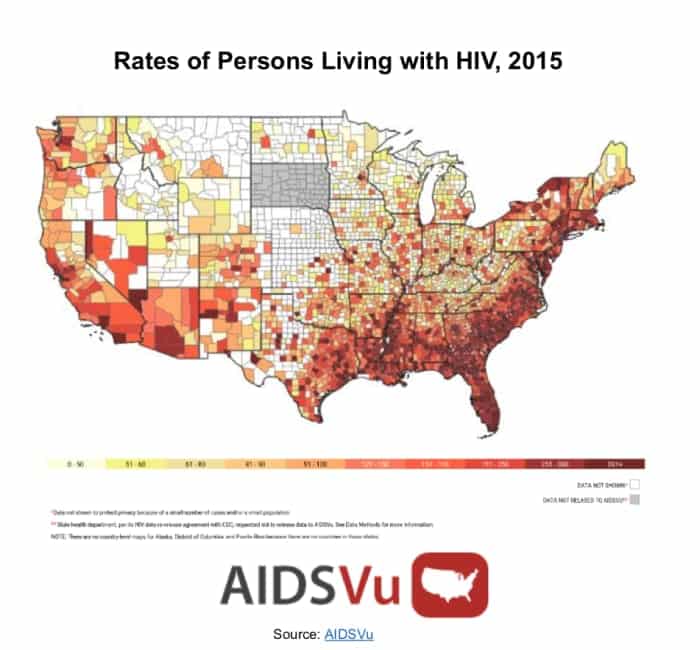
Are Some Regions Of The United States More Impacted By Hiv Than Others
Yes. HIV is largely an urban disease, with most cases occurring in metropolitan areas with 500,000 or more people. The South has the highest number of people living with HIV, but if population size is taken into account, the Northeast has the highest rate of people living with HIV.
*Rates per 100,000 people. Includes adults, adolescents, and children under the age of 13.
New Hiv Infection Rates
New HIV infection rates have dropped over the years. The world has seen a 52% reduction in new HIV infections since the epidemic peaked in 1997. In 1997, 3 million people reported new HIV infections, compared with only 2.1 million in 2010 and 1.5 million in 2020.
This is because people in resource-poor countries now have significantly improved access to HIV treatments. Preventing vertical transmission of HIV, which refers to when the infection passes from a birthing parent to their fetus, has also contributed to lowering transmission rates. Additionally, the medical community has added new HIV prevention tools and methods.
However, the unequal distribution of HIV treatment and prevention strategies still leaves many vulnerable populations behind. Important barriers to improving access to care include stigma, discrimination, social inequities, and exclusion.
Before the COVID-19 pandemic, many people with HIV or at risk of HIV still did not have access to prevention, care, and treatment. The pandemic caused a greater disturbance in the distribution of health services in many countries. Some countries report a 75% disruption of HIV services.
According to UNAIDS, the Joint United Nations Programme on HIV/AIDS, the benefits of providing HIV services outweigh the risk of dying from COVID-19.
HIV spreads through contact with bodily fluids from people who have the virus. Bodily fluids that carry HIV include:
It is not possible to contract HIV through:
- sharing foods or beverages
Also Check: What Antibiotics Are Used To Treat Skin Infections
Hiv Infections By State
In the United States, where you live plays a large part in how likely you are to get HIV. While it is clear that dense urban populations with high prevalence rates contribute to the risk, there are other unique factors that account for a growing disparity between U.S. states.
A prime example is the rate of infection in states that have either adopted or refused Medicaid expansion, intended to expand healthcare to economically disadvantaged people.
According to the CDC, the 13 states that refused Medicaid expansion account for 42% of all new infections. Florida, Texas, Georgia, and North Carolina represent the lion’s share of these infections.
Poverty remains a driving force for HIV infections, particularly in the South where the rates of poverty are highest. Moreover, nearly half of all Americans without health insurance live in the South.
With that being said, the Northeast has a higher prevalence rate overall, centered mainly in dense urban populations like New York City, Baltimore, and Washington, D.C.
These dynamics are reflected in the 10 U.S. states with the highest HIV prevalence rates, according to the CDC.
| State/Area |
|---|
| 65 and over | 900 |
Youth also accounts for the highest rate of undiagnosed infections. Today, nearly half of all HIV-positive youth between the ages of 13 and 24 are unaware of their status and, as a result, are more likely to infect others. The picture is little improved among adults 25 to 34, where one in three remains undiagnosed.