Cdc Classification System For Hiv Infection
| Learn how and when to remove this template message) |
The CDC Classification System for HIV Infection is the medical classification system used by the United StatesCenters for Disease Control and Prevention to classify HIVdisease and infection. The system is used to allow the government to handle epidemicstatistics and define who receives US government assistance.
Revised Classification System For Human Immunodeficiency Virus Infection In Children Less Than 13 Years Of Age
The following CDC staff members prepared this report:
M. Blake Caldwell, M.D., M.P.H.
Robert J. Simonds, M.D.Mary Lou Lindegren, M.D.
Division of HIV/AIDSNational Center for Infectious Diseases
CONSULTANTSExternal ConsultantsStephane Blanche, M.D. Savita Pahwa, M.D.Necker Hospital Cornell Medical SchoolParis, France New York Hospital
New York, NYMary Boland, R.N., M.S.N.Children’s Hospital of New Jersey Catherine Peckham, M.D.Newark, NJ Institute of Child Health
London, EnglandWilliam Borkowsky, M.D.New York University Medical Center Merlin Robb, M.D.New York, NY Walter Reed Army Medical Center
Washington, DCEdward Connor, M.D.Children’s Hospital of New Jersey Gwendolyn Scott, M.D.Newark, NJ University of Miami School of
MedicineLouis Cooper, M.D. Miami, FLSt. Luke’s HospitalNew York, NY William Shearer, M.D., Ph.D.
Baylor College of MedicineClemente Diaz, M.D. Houston, TXUniversity Medical CenterSan Juan, PR Richard Stiehm, M.D.
University of California at LosLeon Epstein, M.D. Angeles Medical CenterUniversity of Rochester School of Los Angeles, CA
MedicineRochester, NY Rand Stoneburner, M.D.
World Health OrganizationDavid Fleming, M.D. Geneva, SwitzerlandOregon Department of Human
Resources Rachel Strikof, M.P.H.Portland, OR New York State Health Department
Albany, NYCeline Hanson, M.D.Baylor College of Medicine Pauline Thomas, M.D.Houston, TX New York City Department of Health
Durham, NC
Centers for Disease Control National Institutes of Health
and Prevention
Beth Roy
The Who Clinical Staging System For Hiv/aids
Virtual Mentor.
For over twenty years, human immunodeficiency virus infection and acquired immunodeficiency syndrome have been significant public health concerns, and the epidemic continues to challenge humanity. The majority of the worlds new HIV infections occur in low- and middle-income countries, with two-thirds of the worlds HIV-infected population living in Africa . Many complex factors contribute to the disproportionate impact of HIV in resource-poor settings: poverty, disease stigma, cultural and social barriers to testing and treatment, insufficient health care infrastructure to support the large patient pool, lack of health literacy, limited provider training, inadequate medical equipment, scarce manpower to distribute health care throughout the region, and few qualified laboratory facilities .
- Provides guidance including when to start, switch, or stop prophylactic medications, antiretrovirals, and other interventions
- Assists clinicians in the assessment of a patients current clinical status
- Encourages clinical providers to offer diagnostic HIV testing to patients who exhibit clinical signs suggestive of HIV infection
- Classifies disease in a progressive sequence from least to most severe
- Is designed to be used with reference to current and previous clinical events, making it useful for surveillance purposes .
You May Like: How To Pull An Infected Tooth At Home
Category A: Mildly Symptomatic
Children with two or more of the conditions listed below but none of the conditions listed in Categories B and C.
- Salmonella , recurrent
- Toxoplasmosis of the brain with onset at greater than 1 month of age
- Wasting syndrome in the absence of a concurrent illness other than HIV infection that could explain the following findings: a) persistent weight loss more than 10% of baseline OR b) downward crossing of at least two of the following percentile lines on the weight-for-age chart in a child at least 1 year of age OR c) less than the 5th percentile on weight-for-height chart on two consecutive measurements at least 30 days apart PLUS a) chronic diarrhea OR b) documented fever
Current Trends Classification System For Human Immunodeficiency Viru Infection In Children Under 13 Years Of Age

INTRODUCTION
With the identification of the causative agent of the acquired immuno-deficiency syndrome , a broad spectrum of clinical manifestations hasbeen attributed to infection with the human immunodeficiency virus .With the exception of the CDC surveillance definition for AIDS , nostandard definitions for other manifestations of HIV infection have beendeveloped for children. Classification systems published to date have beendeveloped primarily to categorize clinical presentations in adult patientsand may not be entirely applicable to infants and children .
Physicians from institutions caring for relatively large numbers ofHIV-infected children report that only about half of their patients withsymptomatic illness related to the infection fulfill the criteria of theCDC surveillance definition for AIDS .
GOALS AND OBJECTIVES OF THE CLASSIFICATION SYSTEM
The system was designed primarily for public health purposes, includingepidemiologic studies, disease surveillance, prevention programs, andhealth-care planning and policy. The panel attempted to devise a simplescheme that could be subdivided as needed for different purposes.
DEFINITION OF HIV INFECTION IN CHILDREN
These definitions apply to children under 13 years of age. Persons 13years of age and older should be classified according to the adult classi-fication system .
CLASSIFICATION SYSTEM
Perinatally exposed infants and children whose infection status isindeterminate are classified into class P-0.
You May Like: Planned Parenthood Treat Yeast Infections
Revision Of The Hiv Center Medical Staging Scale*
HIV-related symptomatology represents both an indirect measure of immune functioning and a clinically significant indicator of disease progression. The most widely used classification system for HIV-related symptomatology is the Centers for Disease Control system. Although the CDC scale has widely recognized clinical utility, it provides only nominal-level measurement, which may be problematic for both clinicians and researchers. This article describes the revision and validation of the HIV Center Medical Staging Scale , an ordinal-level physical illness scale that provides a means of independently measuring the progression of HIV-disease symptomatology and immunological decline. Concurrent use of the rHCMSS, the CDC classification system, and T-lymphocyte and viral load data will provide a more comprehensive indication of HIV-disease progression for clinical and research purposes.
- Previous article in issue
Appendix C: Cdc Pediatric Hiv Cd4 Cell Count/percentage And Hiv
| Stagea | Aged 1 Year to < 6 Years | Aged 6 Years |
|---|---|---|
| < 200 | < 14 |
Key:MMWR
a Only among children aged < 6 years.b Suggested diagnostic criteria for these illnesses, which might be particularly important for HIV encephalopathy and HIV wasting syndrome, are described in the following references:Centers for Disease Control and Prevention. 1994 Revised classification system for human immunodeficiency virus infection in children less than 13 years of age. MMWR. 1994 43.Centers for Disease Control and Prevention. 1993 Revised classification system for HIV infection and expanded surveillance case definition for AIDS among adolescents and adults. MMWR. 1992 41.c Only among adults, adolescents, and children aged 6 years.Key: CMV = cytomegalovirus HSV = herpes simplex virus
Modified from:
Centers for Disease Control and Prevention. 1994 revised classification system for human immunodeficiency virus infection in children less than 13 years of age. MMWR. 1994 43.
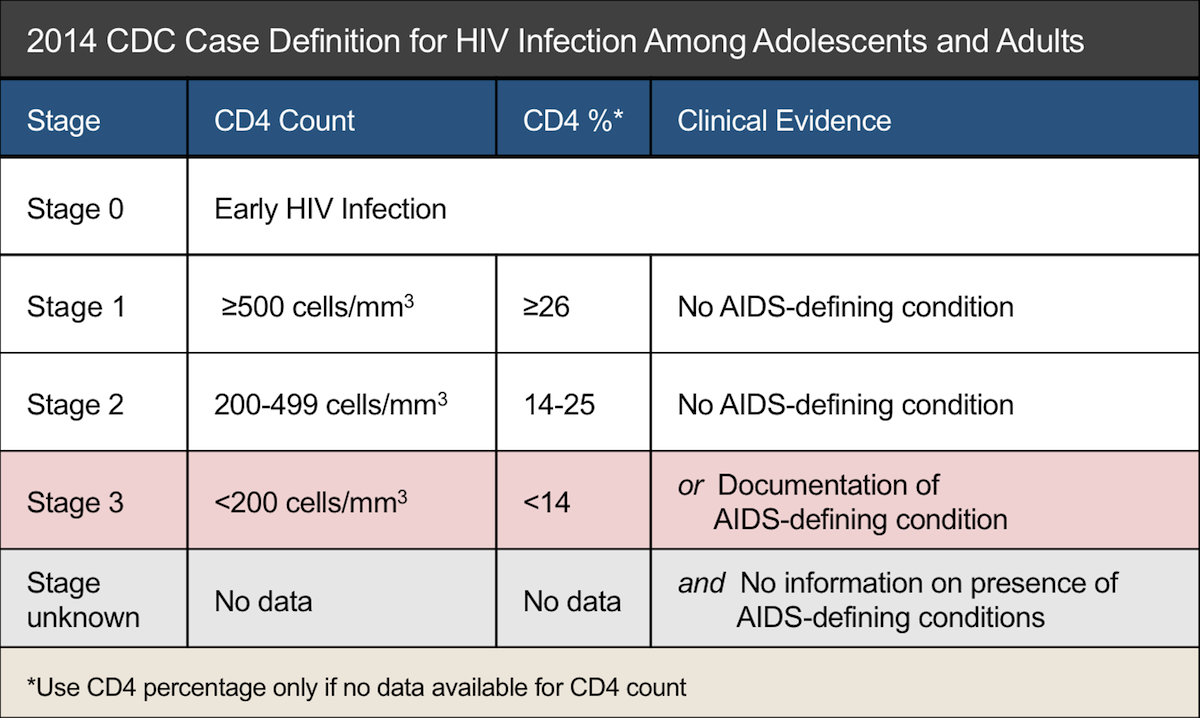
Centers for Disease Control and Prevention: Revised Surveillance Case Definition for HIV InfectionUnited States, 2014. MMWR. 2014 63:1-10.
| Stagea |
|---|
|
Modified from:
Centers for Disease Control and Prevention: Revised Surveillance Case Definition for HIV InfectionUnited States, 2014. MMWR. 2014 63:1-10.
You May Like: Will Tooth Infection Go Away On Its Own
Goals And Objectives Of The Classification System
The classification system presented in this report is primarily applicable to public health purposes, including disease reporting and surveillance, epidemiologic studies, prevention and control activities, and public health policy and planning.
Immediate applications of such a system include the classification of infected persons for reporting of cases to state and local public health agencies, and use in various disease coding and recording systems, such as the forthcoming 10th revision of the International Classification of Diseases.
Tests For Hiv And Aids
Blood tests are the most common way to diagnose the human immunodeficiency virus , the virus that causes acquired immunodeficiency syndrome . These tests look for antibodies to the virus that are present in the blood of infected individuals. People exposed to the virus should get tested immediately.
Early testing is crucial with HIV. If you test positive for the virus, you and your doctor can develop a treatment plan to help fight HIV and ward off complications. Early testing also can alert you to avoid high-risk behavior that could spread the virus to others.
Because it can take from six weeks to six months to develop antibodies to the virus, follow-up tests may be needed. Your doctor will ask about your symptoms, medical history and risk factors and perform a physical examination.
The primary tests for diagnosing HIV and AIDs include:
UCSF Health medical specialists have reviewed this information. It is for educational purposes only and is not intended to replace the advice of your doctor or other health care provider. We encourage you to discuss any questions or concerns you may have with your provider.
Recommended Reading: Natural Nasal Spray For Sinus Infection
Terms Definitions And Calculations
HIV diagnoses and stage 3 classificationsHIV infection is classified as stage 3 when the immune system of a person infected with HIV becomes severely compromised andor the person becomes ill with an opportunistic infection. In the absence of treatment, AIDS usually develops 8 to 10 years after initial HIV infection with early HIV diagnosis and treatment, this may be delayed by many years. With the release of the Revised Surveillance Case Definition for HIV Infection United States, 2014, CDC now uses a stage system to describe HIV infection .
Diagnoses of HIV infection and deaths of persons with diagnosed HIV infection are the number of persons diagnosed with HIV infection and the number of persons with a diagnosed HIV infection who have died in a given time period, respectively. Note that diagnoses of HIV infection are regardless of stage of disease at diagnosis persons who were diagnosed with HIV infection and classified as stage 3 at the same time and persons who were diagnosed with HIV infection that later received a stage classification. Also note that deaths of persons with a diagnosis of HIV infection may be due to any cause . Other systems, such as the National Vital Statistics Reports, provide data on HIV infection as a cause of death in the US population.
Uses of these data: Incidence estimates are useful for planning and for allocating of funds, as well as evaluating the impact of prevention programs.
Percentage
Revision Of Case Definition For Aids For Surveillance Purposes
For national reporting, a case of AIDS is defined as an illness characterized by one or more of the following ”indicator” diseases, depending on the status of laboratory evidence of HIV infection, as shown below.
- I.
-
Without Laboratory Evidence Regarding HIV Infection
If laboratory tests for HIV were not performed or gave inconclusive results and the patient had no other cause of immunodeficiency listed in Section I.A below, then any disease listed in Section I.B indicates AIDS if it was diagnosed by a definitive method .
- A.
-
Causes of immunodeficiency that disqualify diseases as indicators of AIDS in the absence of laboratory evidence for HIV infection
- 1.
-
high-dose or long-term systemic corticosteroid therapy or other immunosuppressive/ cytotoxic therapy 3 months before the onset of the indicator disease
- 2.
-
any of the following diseases diagnosed 3 months after diagnosis of the indicator disease: Hodgkin’s disease, non-Hodgkin’s lymphoma , lymphocytic leukemia, multiple myeloma, any other cancer of lymphoreticular or histiocytic tissue, or angioimmunoblastic lymphadenopathy
- 3.
-
a genetic immunodeficiency syndrome or an acquired immunodeficiency syndrome atypical of HIV infection, such as one involving hypogammaglobulinemia
- B.
You May Like: Is A Uti And Bladder Infection The Same
Category B: Moderately Symptomatic
Children who have symptomatic conditions other than those listed for CategoryA or C that are attributed to HIV infection. Examples of conditions in clinicalCategory B include but are not limited to:
- Anemia , neutropenia , or thrombocytopenia persisting for at least 30 days
- Cytomegalovirus infection, with onset before 1 month of age
- Diarrhea, recurrent or chronic
- Herpes simplex virus stomatitis, recurrent
- HSV bronchitis, pneumonitis, or esophagitis with onset before 1 month of age
- Herpes zoster involving at least two distinct episodes or more than one dermatome
- Persistent fever
- Toxoplasmosis, onset before 1 month of age
- Varicella, disseminated
Revised Classification System For Hiv Infection And Expandedsurveillance Case Definition For Aids Among Adolescents And Adults
The following CDC staff members prepared this report:
National Center for Infectious Diseases Division of HIV/AIDSKenneth G. Castro, M.D.John W. Ward, M.D.Laurence Slutsker, M.D., M.P.H.James W. Buehler, M.D.Harold W. Jaffe, M.D.Ruth L. Berkelman, M.D.
Office of the DirectorAssociate Director for HIV/AIDSJames W. Curran, M.D., M.P.H.
1993 Revised Classification System for HIV Infection and ExpandedSurveillance Case Definition for AIDS Among Adolescents and Adults
Summary
CDC has revised the classification system for HIV infection toemphasize the clinical importance of the CD4+ T-lymphocyte count inthe categorization of HIV-related clinical conditions. Thisclassification system replaces the system published by CDC in 1986 and is primarily intended for use in public health practice.Consistent with the 1993 revised classification system, CDC hasalso expanded the AIDS surveillance case definition to include allHIV-infected persons who have less than 200 CD4+ T-lymphocytes/uL,or a CD4+ T-lymphocyte percentage of total lymphocytes of less than14. This expansion includes the addition of three clinical conditions
-
pulmonary tuberculosis, recurrent pneumonia, and invasive cervical cancer — and retains the 23 clinical conditions in the AIDS surveillance case definition published in 1987 it is to be used by all states for AIDS case reporting effective January 1, 1993.
REVISED HIV CLASSIFICATION SYSTEM FOR ADOLESCENTS AND ADULTS
CD4+ T-Lymphocyte Categories
Clinical Categories
You May Like: Antibiotics For Spider Bite Infection
Different Stages Of Infection
Stages of HIV infection are described differently by the World Health Organisation and the US medical system. These stages are less important because of effective HIV treatment .
- WHO stages use symptoms only and do not test results.
- The US Center for Disease Control categories use both symptoms and test results.
In Adults And Adolescents
This classification system is how the United States agency, the Centers for Disease Control and Prevention classifies HIV disease and infection. This is to allow the government to handle epidemic statistics and define who receives US government assistance. In 1993, the CDC added pulmonary tuberculosis, recurrent pneumonia, and invasive cervical cancer to the list of clinical conditions in the AIDS surveillance case definition published in 1987 and expanded the AIDS surveillance case definition to include all HIV-infected persons with CD4+ T-lymphocyte counts of less than 200 cells/uL or a CD4+ percentage of less than 14. Considerable variation exists in the relative risk of death following different AIDS defining clinical conditions.
According to the US CDC definition, one has AIDS if he/she is infected with HIV and present with one of the following:
- A CD4+ T-cell count below 200 cells/l
- Tuberculosis
- Wasting syndrome due to HIV
People who are not infected with HIV may also develop these conditions this does not mean they have AIDS. However, when an individual presents laboratory evidence against HIV infection, a diagnosis of AIDS is ruled out unless the patient has:
- the individual has had Pneumocystis carinii pneumonia
- OR one of the above defining illnesses AND a CD4+ T-cell count below 200 cells/l .
Read Also: Yeast Infection Test Strips Walgreens
Cdc Classification System For Hiv
CDC HIV CLASSIFICATION FOR ADULTS AND ADOLESCENTS
Version/Release Date/File
You must to view and download files.
Clear Data. Clear Impact.
© 2022 Clinical Data Interchange Standards ConsortiumCDISC is a 501 global nonprofit charitable organization with administrative offices in Austin, Texas,with hundreds of employees, volunteers, and member organizations around the world.
Cdc Classification System For Hiv Infection In Children
In the new system, HIV-infected children are classified into mutually exclusive categories according to three parameters:
- a) infection status
- b) clinical status
- c) immunologic status
This classification system reflects the stage of the child’s disease, establishes mutually exclusive classification categories, and balances simplicity and medical accuracy in the classification process. This document also describes revised pediatric definitions for two acquired immunodeficiency syndrome-defining conditions.
When an infant is born to an HIV-infected mother, diagnosis of an HIV infection is complicated by the presence of maternal anti-HIV IgG antibody, which crosses the placenta to the fetus. Indeed, virtually all children born to HIV-infected mothers are HIV-antibody positive at birth, although only 15%-30% are actually infected.
Read Also: Otc Urinary Tract Infection Relief
Screening For Hiv Infection
The US Preventive Services Task Force strongly recommends that clinicians screen for HIV in all adolescents and adults at increased risk for HIV infection, and all pregnant women.
The American College of Obstetricians and Gynecologists recommends that all females aged 13-64 years be tested for HIV at least once during their lifetime. Retesting annually or more often is recommended for those at high risk because of injection drug use, sex with an injection drug user, sex for money or drugs, sex since their most recent HIV test with men who have sex with men, or sex since their most recent HIV test with more than 1 person.
Guidelines issued in 2015 on HIV testing during pregnancy by the American College of Obstetricians and Gynecologists are as follows:
The Centers for Disease Control and Prevention recommends HIV screening for patients in all health-care settings, after the patient is notified that testing will be performed unless the patient declines the CDC recommends that persons at high risk for HIV infection be screened for HIV at least annually.
Citing the benefits of early diagnosis and treatment and the failure of risk-based screening to identify a substantial proportion of HIV-infected patients early in the disease, the American College of Physicians recommends that clinicians adopt routine screening for HIV and encourage all patients to be tested.