Human Papilloma Virus Persistence After Cone Excision In Women With Cervical High Grade Squamous Intraepithelial Lesion: A Prospective Study
Florin Horhat
1Department of Obstetrics and Gynecology, University of Medicine and Pharmacy Victor Babe, Timioara, 300041 Timi, Romania
2Department of Anatomy, University of Medicine and Pharmacy Victor Babe, Timioara, 300041 Timi, Romania
3Department of Obstetrics and Gynecology, County Hospital Timioara, 300202 Timi, Romania
4Department of Informatics and Statistics, University of Medicine and Pharmacy Victor Babe, Timioara, 300041 Timi, Romania
5Department of Surgery, University of Medicine and Pharmacy Victor Babe, Timioara, 300041 Timi, Romania
6Department of Microbiology, University of Medicine and Pharmacy Victor Babe, Timioara, Piata Eftimie Murgu, No. 1, 300041 Timi, Romania
Abstract
1. Introduction
HPV 16 and 18 are the most common HR-HPV types worldwide and account for about 70% of all squamous cells carcinomas and for up to 85% of all adenocarcinomas. HPV 16 is the most carcinogenic HPV genotype and HPV 18 causes a greater proportion of glandular cancers compared to squamous cell carcinoma. After HPV 16 and 18, the six most prevalent types that account for an additional 20% are types 31, 33, 35, 45, 52, and 58 .
The objectives of our study were to estimate the rate of HPV infection persistence after LEEP in patients with high grade squamous intraepithelial lesions and to investigate if HPV persistence is type related.
2. Materials and Methods
Dna Sample Quality Assessment
The optical density of the extracted DNA samples was calculated from the absorbance ratio at 260 nm/280 nm measured in a Protein Nucleic Acid Analyzer. The OD 260/280 value of the DNA samples ranged from 1.62.0. In addition, the human -globin gene was detectable in the collected DNA samples, indicating the adequacy of the specimen for DNA amplification.
How Many Leeps Should I Have Before A Hysterectomy
A hysterectomy is a major surgery to remove your uterus that should never be the first-line treatment for treating abnormal cell growths. Your provider may recommend a hysterectomy if you have more advanced cervical dysplasia, and additional LEEPs or related procedures havent prevented abnormal cells from recurring. Talk to your provider about your options based on your unique circumstances.
Recommended Reading: What Is The Difference Between A Yeast Infection And Chlamydia
Risk Factors For The Presence Of Hpv Dna In The Surgical Plume
The risk factors for the existence of HPV DNA in surgical smoke are presented in Table 5. Among the 134 cervical cell samples that were positive for HPV DNA, the positive rates of HPV DNA in surgical smoke determined by the hybridization technique at different distances from the suction device to the surgical site were 9.1%, 15.3%, 45.1% and 53.9%, respectively. The Chi-square test revealed that positive rate of HPV DNA in surgical smoke was significantly higher in samples obtained at a greater distance between the suction device and surgical site . Therefore, the distance between the suction device and surgical site was positively associated with the presence of HPV DNA in surgical smoke. However, the operation time and pathological grade were not significantly correlated with the presence of HPV DNA in surgical smoke. As shown in Table S2, logistic regression analysis revealed that the location of the suction device from the surgical site influenced the presence of HPV DNA in surgical smoke .
|
Table 5 Correlation of HPV DNA in surgical smoke with the distance of the suction device from the surgical site, operation time and pathological grade |
Hpv Dna In Surgical Smoke
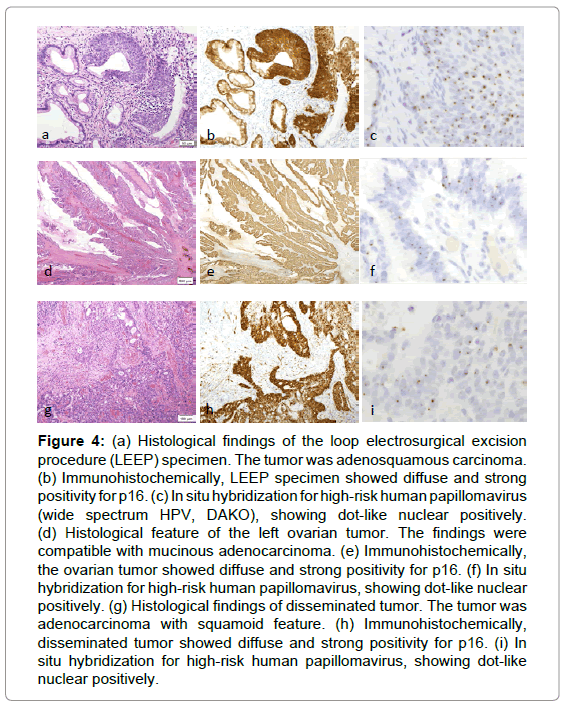
A total of 40 of the 134 surgical smoke samples were positive for HPV DNA by flow fluorescence in situ hybridization. The specific distribution of the HPV subtypes in cervical cells and LEEP plume is shown in Table 4. HPV16 was the most common type, followed by HPV58 , HPV52 , HPV33 , HPV31 and HPV18 . In addition, single HPV infections and dual HPV infections with HPV52 and 58 DNA were detected in smoke plume samples. As shown in Figure 1B, HPV 16 was detected in 27.5% of the smoke plume specimens and was the most common subtype found in the HPV DNA-positive LEEP plume specimens, followed by HPV 58 , 52 , 33 , 31 , 18 , 68 , 53 and 56 . Additionally, HPV DNA positivity in the exfoliated cervical cells was significantly associated with HPV DNA positivity in the surgical plume, as shown in Table S1.
|
Table 4 Detection of specific HPV genotypes by flow fluorescence in situ hybridization in exfoliated cervical cells, surgical plume and LEEP operators nasal swab samples |
Read Also: I Ve Had A Sinus Infection For 2 Months
Are There Other Treatments For Cervical Dysplasia Other Than Leep
Your provider can use several methods to remove abnormal tissue from your cervix. Some, like LEEP, allow for a pathologist to study a tissue sample for signs of cancer or precancerous cells. These methods include:
- Cryosurgery: The surface tissue is destroyed by freezing. Cryosurgery doesnt allow a pathologist to review the tissue to look for cancer.
- Cold knife conization: A cone-shaped wedge of tissue is removed from your cervix. This procedure carries similar risks to LEEP and allows for pathology to assess the tissue for cancer.
- Laser treatment or cone excision: Heat from a high-intensity beam of light destroys or cuts away abnormal tissue. This procedure doesnt leave a tissue sample for a pathologist to inspect for cancer cells.
The best treatment for you will depend on factors such as the amount and location of the abnormal tissue.
Hpv Dna In Operators Nasal Epithelial Cells
All nasal epithelial cells obtained from the doctors preoperative nasal swabs were negative for HPV DNA. Among the operators, 70.1% wore an ordinary mask, and the others wore a special N95 surgical mask. However, 2 of the 134 swabs obtained from the nasopharynx postoperatively were positive for HPV: one was positive for HPV 16, and the other was positive for HPV 58. These two HPV subtypes were detected in operators who wore the ordinary face mask when operating LEEP. Moreover, the distribution of HPV subtypes in the operators nasal swabs was consistent with the genotypes detected in the corresponding cervical cells and surgical smoke samples. The same results were obtained for nasal swabs by flow fluorescence in situ hybridization and PCR assay. In addition, the operators whose nasal swabs were positive for HPV underwent a nasal swab examination after an additional 3, 6, 12, 18 and 24 months one operator tested negative for HPV16 DNA at the 3-month examination, and the other operator tested negative for HPV58 at 6 months. Additionally, both nasal swabs were negative for HPV DNA at the subsequent examinations at 12 months and 24 months. Furthermore, these doctors with nasal swabs positive for HPV16 or 58 were confirmed to have no HPV-related diseases, such as verruca acuminate, every 3 months during the subsequent 35 and 43 months, respectively.
Read Also: Oral Yeast Infection Pill Otc
British Columbia Specific Information
Health Canada has approved 2 HPV vaccines:
To determine if you are eligible to receive the free vaccine, see HealthLinkBC File #101b Human Papillomavirus Vaccines, visit ImmunizeBC HPV , or speak with a public health nurse at your local public health unit. Those not eligible for the free HPV vaccine can purchase it at most pharmacies and travel clinics and at some sexual health clinics.
To learn more about HPV infection, see HealthLinkBC File #101a Human Papillomavirus Infection and Genital Warts. For more information on STIs, sexual health information, where to get tested and other sexual health services in your area, visit SmartSexResource.
What Happens Before Leep
Your healthcare provider will ensure you dont have any conditions that may prevent you from getting the procedure. For instance, you shouldnt have a LEEP if you have acute pelvic inflammatory disease or inflammation of your cervix . You may need to take a pregnancy test before getting a LEEP. Your provider can advise you on the right timing for a LEEP if youre pregnant.
If there arent any contraindications, your provider will schedule the procedure at a time when youre not menstruating, ideally one week after your period ends.
Follow your providers instructions about how to prepare. Your provider may advise you to:
- Avoid having intercourse or using vaginal creams or douches 24 hours before the procedure.
- Pack a pad that you can wear after the procedure to handle any vaginal discharge.
- Stop taking medications that affect how your blood clots, like anticoagulants or aspirin.
- Take a pain reliever like ibuprofen or acetaminophen 30 minutes before the procedure.
- Wear loose-fitting clothes that you can easily remove and replace with a hospital gown on the day of your procedure.
Recommended Reading: Iud And Yeast Infection Treatment
What Are The Risks For A Leep
Some possible complications may include:
- Changes or scarring in the cervix from removal of tissue
- Trouble getting pregnant
- Potential for preterm birth or having a low birth weight baby
If you are allergic to or sensitive to medications, iodine, or latex, tellyour healthcare provider.
If you are pregnant or think you could be, tell your healthcare provider.
There may be other risks depending on your condition. Be sure to discussany concerns with your healthcare provider before the procedure.
Certain factors or conditions may interfere with LEEP. These factorsinclude:
- Acute inflammation of the cervix
Why Youd Have One
Your doctor may have recommended a LEEP if your Pap smear or a tissue sample from your cervix showed some cells that didnât look normal. You may also get one if your doctor found something unusual during an examination of your . Doctors use LEEP to diagnose or treat abnormal things, including cells that look like they might become cancer.
Before you agree to get one, make sure your doctor explains:
- Why they want you to have one
- What the results could mean
- What the risks, benefits, and complications could be
Dont Miss: Bladder Infection From Swimming Pool
Recommended Reading: Yeast Infection Resistant To Diflucan
Loop Electrosurgical Excision Procedure
In the late twentieth century, Sheldon Weinstein, a surgeon who worked in gynecology in the United States, invented the Loop Electrosurgical Excision Procedure, or LEEP, a procedure for removing abnormal, pre-cancerous cells from a woman’s cervix in the US. LEEP, also known as the Large Loop Excision of the Transformation Zone, involves inserting a wire loop heated by an electrical current into a womans to remove the entire surface layer of cells in the cervix, the passage between the and the bottom of the uterus. The procedure removes cells with pre-cancerous changes before they progress into cervical cancer. Women who receive LEEP often spend less than an hour at their gynecologist’s office for the procedure and may experience side effects such as cramping and light bleeding. LEEP replaced several invasive and potentially dangerous cervical cancer treatments, providing a quick and inexpensive way to remove women’s pre-cancerous cervical cells before they progress to cervical cancer.
LEEP also carries risks of infection, bleeding, a chance of scarring the cervix by removing tissue, trouble getting pregnant, and low birth weight babies. Despite risks associated with the procedure, many physicians recommend LEEP for women who experience pre-cancerous cervical changes. However, many earlier stages of cervical cancer are not visible to the naked eye, and patients can die from only treating cancer in its later, more advanced stages.
How Does The Loop Electrosurgical Excision Procedure Work
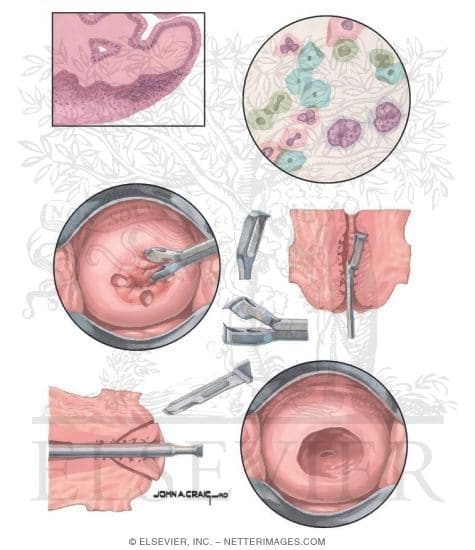
LEEP is used in treating moderate or mild precancerous changes in your uterus. This technique is sometimes used to treat cancers that have gone deeper into the tissue of your cervix or severe cases of dysplasia.
In some cases, your doctor will apply a local anesthetic medication in the area of the cervix, known as a cervical block. Medications for pain control can also be given intravenously or pre-operatively in pill form. This procedure is different from the ones where the abnormal tissue is destroyed, such as with freezing or laser techniques.
Recommended Reading: How Long After Yeast Infection
Why Would You Need To Have Leep
Your healthcare provider may recommend LEEP after a Pap smear or a colposcopy biopsy confirms that you have abnormal cells in your cervix. Colposcopy is a noninvasive procedure where a device similar to a microscope magnifies your cervix to make abnormal growth easier to see.
LEEP is used to diagnose and treat cervical dysplasia and conditions like genital warts and polyps.
What Is A Loop Electrosurgical Excision Procedure
Loop electrosurgical excision procedure uses a wire loop heated byelectric current to remove cells and tissue in a womans lower genitaltract. It is used as part of the diagnosis and treatment for abnormal orcancerous conditions.
With LEEP, an electric current passes through the fine wire loop to cutaway a thin layer of abnormal tissue. This tissue will be sent to the labfor testing. LEEP can also remove abnormal cells to allow healthy tissue togrow.
Don’t Miss: Can You Get Sick From A Tooth Infection
When Is Leep Used
Your doctor may recommend a LEEP if your Pap test or gynecological exam reveals abnormal cells. The procedure may also be used to confirm a cancer diagnosis or to treat precancerous conditions.
HPV can cause precancerous changes to the cervix. If you have HPV or your doctor suspects it, you may need a LEEP to remove precancerous tissue to prevent it from developing into cancer.
Genital warts caused by HPV and benign polyps can also be removed with LEEP.
After LEEP, you could experience some side effects, including:
- scarring on the cervix
Your doctor can help you weigh the risks and benefits of LEEP.
As with any procedure that cuts or removes tissue, theres a risk of infection. Signs of infection include fever, chills, and pain. Let your doctor know if you have any of these symptoms after your LEEP.
Memorial Sloan Kettering Cancer Center provides a pretty thorough rundown of what to expect with your LEEP.
Here are the highlights:
What Happens After The Procedure
You may rest for a few minutes after the procedure before going home. You may want to wear a sanitary pad for bleeding. It is normal to have some mild cramping, spotting, and dark or black-colored discharge for several days. The dark discharge is from the medication applied to your cervix to control bleeding.
You may also have other restrictions on your activity, including no strenuous activity or heavy lifting.
Take a pain reliever for cramping or soreness as directed by your physician. Aspirin or certain other pain medications may increase the chance of bleeding. Be sure to take only recommended medications.
Your physician will advise you on when to return for further treatment or care. Generally, women who have had LEEP will need more frequent Pap tests.
Notify your physician if you have any of the following:
- Bleeding with clots
- Fever and/or chills
Dont Miss: Is Psoriasis A Viral Infection
Don’t Miss: Oil Of Oregano Pills For Yeast Infection
Are There Any Risks Associated With Leep
As with any surgical procedure, complications may occur. Some possible complications may include, but are not limited to, the following:
- Changes or scarring in the cervix from removal of tissue
- Difficulty getting pregnant
- Potential for preterm birth or having a low birth weight baby
Patients who are allergic to or sensitive to medications, iodine, or latex should notify their physician.
There may be other risks depending upon your specific medical condition. Be sure to discuss any concerns with your physician prior to the procedure.
Are There Complications Or Risks With Leep
There are no reported or common risks with LEEP. Any complications or side effects would involve increased bleeding, narrowing of the cervix opening, or infection. LEEP is associated with preterm labor in a subsequent pregnancy, and your doctor may want to schedule a followup in this situation.
LEEP carries a small risk of making your cervix incompetent during pregnancy. This incompetence means your cervix does not stay closed tightly enough during pregnancy. If this issue should occur, there are procedures to help keep the cervix closed, so it is able to support a pregnancy.
LEEP has been presented as very safe, but there are some risks acknowledged. Some risks include a heightened risk of premature labor, low birth weights, second-trimester miscarriage, and in few, rare cases there have been reports of the cervix narrowing, which caused the menstruation cycle to be obstructed causing severe pain.
Other complaints have come through from a group of women complaining that the LEEP procedure has affected their sexual drive. The official word from most doctors in the United States, and worldwide, is there are no proven sexual side effects from the LEEP procedure. While there has not been a lot of research into the side effects of sexual drive impact, one paper in Thailand found that LEEP is associated with a small but significant decrease in overall sexual satisfaction.
Recommended Reading: Chronic Uti Symptoms But No Infection
Loop Electrical Excision Procedure
With a loop electrosurgical excision procedure, or LEEP, your doctor uses a wire loop heated by an electrical current to remove large genital warts or abnormal cervical tissue. It can be performed in the doctors office with sedation and local anesthesia or in the hospital with general anesthesia. While there may be some discomfort during the procedure, it is not painful.
Recovery can take one to three days, depending on the number of warts removed or the size of the area treated for abnormal cells. Sexual activity should be avoided for one to three weeks after the procedure.
Leeps Impact On The Cervical Microbiome
In total 1,914,331 reads were obtained from 52 samples with an average number of reads per sample of 36,814 and the mean and medium read lengths of 445 and 453bp respectively. Using bacterial genera sequence data, samples were classified according to their bacterial communities consistent with previously described cervical microbiome as cervicotypes CT1: primarily composed of non-iners Lactobacillus , CT2: Lactobacillus iners dominated, CT3: Gardnerella dominated, CT4: lack of a consistent dominant species but communities all included Prevotella . To further explore the relationship between 4 distinct CTs, a PCA analysis was performed using the species-level taxonomic profiles. As shown in Fig. and Supplementary Fig. , the first two principal components, representing 71.08% of the variance, classified the 52 samples into three groups, though CT3 and CT4 are a continuum. The analysis of similarity test using Bray-Curtis dissimilarity showed that the observed cluster patterns were significant . Although the clusters were not clearly separated by LEEP surgery, most women with LEEP surgery carried L. iners as the dominant members.
Figure 1
Also Check: What Do Doctors Prescribe For Yeast Infections
Also Check: Can Ear Infections Go Away