Is This Your Child’s Symptom
- Your child was diagnosed with a Strep throat infection
- A doctor has told you your child probably has Strep throat or
- Your child has a positive Strep test
- Your child is taking an antibiotic for Strep throat and you have questions
- You are worried that the fever or sore throat is not getting better fast enough
Symptoms Of Strep A Infections
Usually, strep A infections only cause minor symptoms. Only in rare cases can a more serious infection develop.
Throat infection
Symptoms and signs of a sore throat include:
- swollen tonsils
- a painful, tender feeling at the back of your throat
- discomfort when swallowing
- an unusually high or low temperature
- unusually fast or slow breathing
- an unusually fast or slow heart rate
While much rarer, strep B infections can occasionally develop in adults. These tend to take a similar form to invasive strep A infection, with symptoms depending on where in the body the infection takes place.
What Is Strep Infection
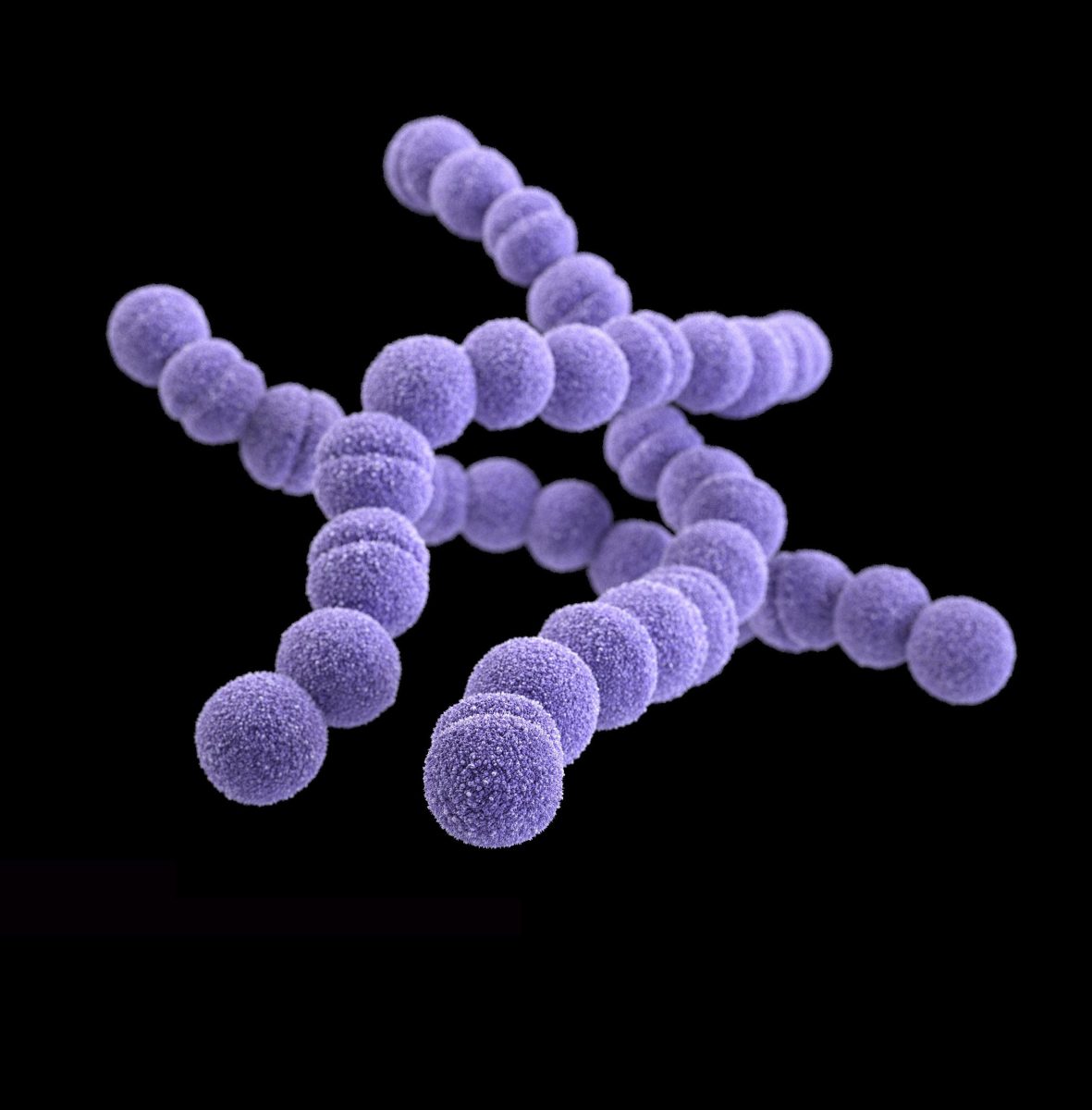
Strep infection is a bacterial infection caused due to Streptococcus bacteria. Streptococci are gram-positive aerobic organisms that cause many diseases. There are three different types of Streptococci as alpha haemolytic Streptococci, beta haemolytic Streptococci, and gamma haemolytic Streptococci. Many Streptococci have virulent factors, including streptolysin, DNAases, and hyaluronidase, which help tissue destruction and spread of disease. A few strains also make exotoxins trigger, releasing cytokines leading to shock, organs failure, and death. Alpha haemolytic Streptococci include Streptococcus pneumoniae and Viridians Streptococcci. Streptococcus pneumoniae can cause sinusitis, middle ear infection, pneumonia, meningitis, and bacteremia. Viridians Streptococcci can cause endocarditis. Beta haemolytic Streptococci include group A and group B Streptococcci. They can cause strep throat, scarlet fever, impetigo, and pneumomia. Gamma haemolytic Streptococci include group D Streptococci. They can cause endocarditis and urinary tract infections.
Figure 01: Strep Infection
The common symptoms of strep infections include tiredness, weakness, fever, weight loss, respiratory problems, problems with heart function, stiff neck, headache, confusion, etc. Diagnosis can be made through physical examination, tissue biopsy, culturing, rapid antigens test, and blood tests. The treatment is mainly done through the administration of antibiotics such as penicillin and amoxicillin.
Recommended Reading: Why Do I Get A Sinus Infection Every Year
About Group A Streptococcus: Commonly Asked Questions
Download a PDF version formatted for print:Group A Streptococcus: Commonly Asked Questions
What is Group A Streptococcus ? Group A streptococci are bacteria commonly found in the throat and on the skin. People may carry GAS in the throat or on the skin and not become ill.
How are Group A Streptococci Spread? These bacteria are spread by direct contact with discharges from the nose and throat of infected people or by contact with infected wounds or sores on the skin. The risk of spreading the infection is highest when a person is ill, such as when people have “strep throat” or an infected wound. People who carry the bacteria but have no symptoms are much less able to spread the bacteria. Treatment of an infected person with an appropriate antibiotic for 24 hours or longer removes their ability to spread the bacteria. However, it is important that a person take all of the antibiotic as prescribed. Household items like plates, cups, toys, etc., do not play a major role in disease spread.
How Common is Invasive Group A Streptococcal Disease? It is estimated that about 10,000-15,000 cases of invasive GAS disease occur in the U.S. each year resulting in over 2,000 deaths. CDC estimates there are 500-1,500 cases of necrotizing fasciitis and 2,000-3,000 cases of STSS each year in the United States. In contrast, there are several million cases of the milder GAS illnesses, strep throat, and impetigo, each year.
Why Does Invasive Group A Streptococcal Disease Occur
Invasive group A streptococcal infections occur when the bacteria gets past the defenses of the person who is infected. This may occur when a person has sores or other breaks in the skin that allow the bacteria to get into the tissue. Health conditions that decrease a person’s immunity to infection also make invasive disease more likely. In addition, there are certain strains of GAS that are more likely to cause severe disease than others. The reason why some strains will cause more severe illness is not totally clear but may involve the production of substances that cause shock and organ damage and of enzymes that cause tissue destruction.
You May Like: Can Yeast Infections Clear On Their Own
Treatment For Group A Streptococcal Infection
A course of antibiotics is the standard treatment for group A streptococcal infection the duration will depend on the site of infection. Antibiotics which may be prescribed include:
- penicillin
- a cephalosporin or macrolide antibiotic if you are allergic to penicillin
- antibiotic ointments for impetigo.
What Is Staph Infection
Staph infection is a bacterial infection caused due to Staphylococcus bacteria. They are commonly found in the human skin and nose. Normally, they cause minor skin infections. Staph infection can turn deadly if the bacteria invade deeper into the body and enter the bloodstream, joints, bones, and lungs. The symptoms vary from minor skin infections to lethal endocarditis. Skin infections cause boils, impetigo, cellulitis, and scalded skin syndrome. The symptoms of food poisoning include diarrhoea, nausea, vomiting, dehydration, and low blood pressure. Bacteremia causes infections in the lung, heart, and brain. Moreover, Staphylococcus causes toxic shock syndrome. The symptoms of toxic shock syndrome include high fever, rash, confusion, muscle ache, diarrhoea, and stomach pain.
Figure 02: Staph Infection
You May Like: Antibiotics Not Helping Ear Infection
Signs And Symptoms Of Sore Throat
The way youre most likely to tell the difference between a bacterial and a viral sore throat is by the symptoms. Below are three symptoms each of bacterial and viral sore throats that do not appear in the other type.
Bacterial
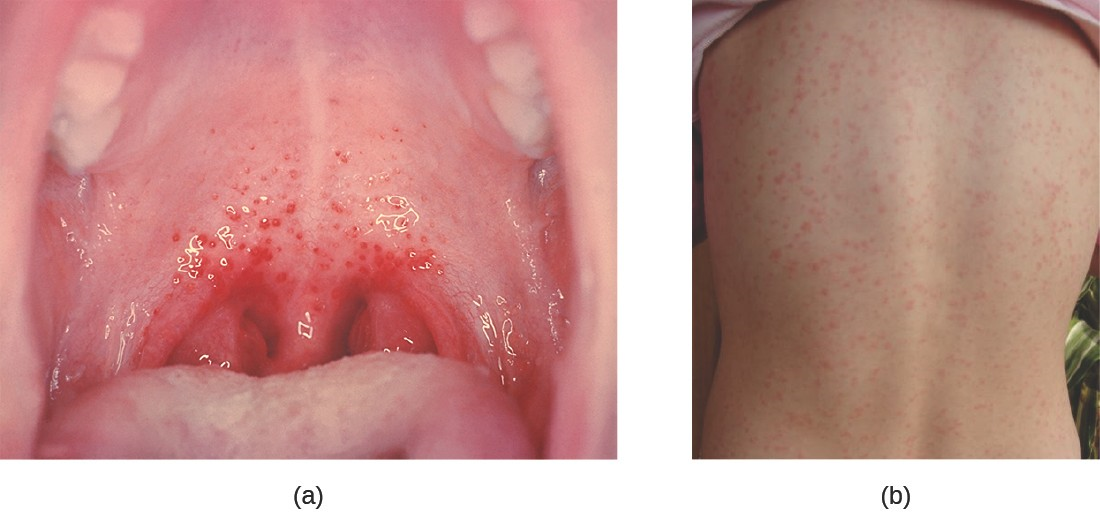
Painful swallowing is common to both bacterial and viral sore throats, but bacterial sore throats often come with red and swollen tonsils at the back of the throat. You may very well also see white patches or streaks of pus there. Fever is also common to both, but the fever associated with bacteria tends to be higher and more severe than with a viral infection.
Some people with a strep throat infection will also notice tiny red spots, called petechiae, on the roof of the mouth. These are actually tiny blood vessels, capillaries, that have broken as a result of the infection and are leaking little bits of blood.
Here are some more common symptoms that distinguish a bacterial sore throat from a viral one:
Viral
Here are some of the major signs to look for:
This is why an accurate medical diagnosis is necessary.
What Are Different Types Of Sore Throat
Sore throats may be divided into three types based on the part of the throat they affect
- Pharyngitis: It affects the area right behind the mouth.
- Tonsillitis: Swelling and redness of the tonsils, the soft tissue in the back of the mouth. Sometimes, white patches or areas of pus will form on the tonsils. These white patches are more common in strep throat than in a sore throat caused by a virus.
- Laryngitis: Swelling and redness of the voice box or larynx.
Recommended Reading: External Vulvar Cream For Yeast Infection
What Are The Symptoms Of Group A Streptococcal Infections
Symptoms range in severity and vary based on the illness that the group A streptococcus bacteria caused. Mild symptoms of group A streptococcal infection include:
- Difficulty swallowing or pain when swallowing.
- Severe pain that spreads beyond the wound.
- Skin changes color .
- Skin swells or is warm to the touch.
Who Do Group A Streptococcal Infections Affect
Group A streptococcal infections can affect anyone since the bacteria easily spreads from person to person. People who have a GAS infection are contagious while theyre ill. They can pass the bacteria to you by coughing or sneezing or you can get the bacteria if you come into contact with an infected part of their skin .
Read Also: Is A Uti And A Bladder Infection The Same
What Questions Should I Ask My Doctor
- How often should I take antibiotics?
- What type of infection do I have?
- What type of antibiotics can I take if I have a penicillin allergy?
- How should I take care of my wound until it heals?
A note from Cleveland Clinic
Group A streptococcal infections cause temporary illnesses that are easily treated with antibiotics. If you experience symptoms, visit your healthcare provider to receive treatment to minimize the amount of time youll feel under the weather. Infections can be serious and spread to other parts of your body, so dont delay getting treatment.
Treatment Of Streptococcal Skin Infection
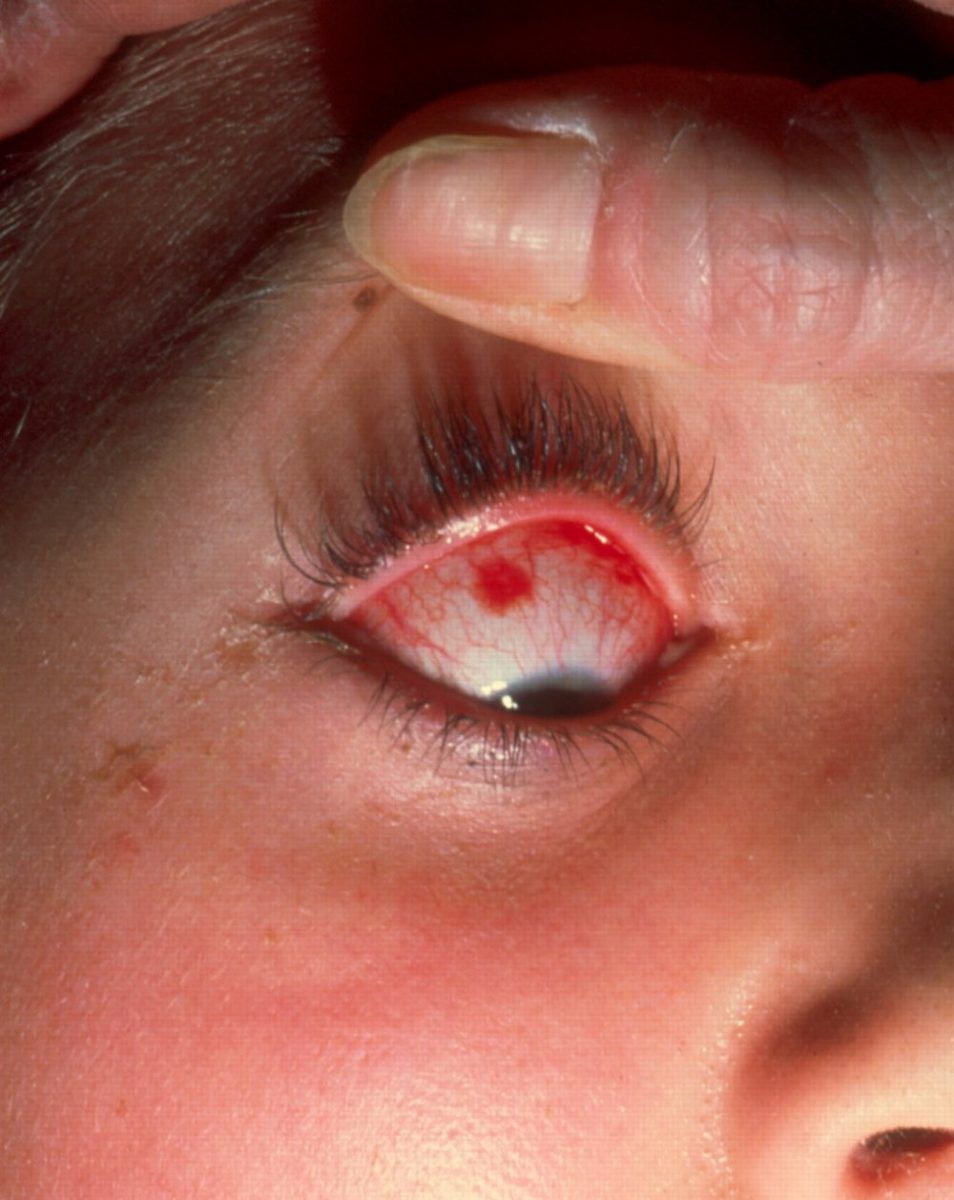
It can be difficult to distinguish clinically between skin infection caused by streptococci and other bacteria such as Staphylococcus aureus. Antibiotics should therefore be chosen to cover the most likely organisms. Flucloxacillin is more appropriate than simple penicillin as it treats both Staphylococcus and strep.
If the laboratory has confirmed streptococcal infection, then the most appropriate antibiotic is usually penicillin. All streptococci in the Lancefield group are very sensitive to penicillin. Those patients with penicillin allergy may be given erythromycin or a cephalosporin , which are effective against most streptococci although some erythromycin resistance is emerging. In very severe S. pyogenes infections, such as necrotising fasciitis, clindamycin may be added to penicillin as very large numbers of bacteria may overwhelm penicillin’s mechanism of action.
Pneumococcal skin infections are generally treated with penicillin but low levels of resistance have recently been reported. In more serious infections, ceftriaxone or vancomycin may be more appropriate.
Recommended Reading: Treat Bv And Yeast Infection At Same Time
Who Is Most At Risk Of Invasive Group A Streptococcal Disease
Few people who come in contact with a virulent strain of GAS will develop invasive GAS disease most will have a routine throat or skin infection and some may have no symptoms whatsoever. Although healthy people can get invasive GAS disease, people with chronic illnesses like cancer, diabetes and kidney dialysis, and those who use medications such as steroids, are at higher risk. In addition, breaks in the skin, like cuts, surgical wounds or chickenpox, may provide an opportunity for the bacteria to enter the body.
Should Close Contacts Of Individuals With Invasive Group A Streptococcal Disease Be Tested And Treated
There have been no reports of casual contacts, like co-workers or school classmates, developing invasive Group A Strep disease following contact with a person who developed invasive Group A Strep disease. Rarely, however, close contacts such as family members have developed invasive Group A Strep disease. Persons at highest risk include contacts with underlying diseases or contacts of patients with the most severe forms of invasive Group A Strep . Therefore, the decision regarding antibiotic prophylaxis should be made on an individual basis by the physicians involved.
Also Check: Can You Get Antibiotics For A Viral Infection
What Are Group A Streptococcal Infections
Group A streptococcal infections occur when a microorganism enters your body and causes an illness, most often in your skin and throat. There are more than 120 strains of group A Streptococcus bacteria, which is the bacteria that causes group A streptococcal infections.
The majority of illnesses caused by GAS bacteria are mild. Sometimes, GAS infections cause severe, life-threatening symptoms if you dont receive treatment.
How Can I Reduce My Risk Of Spreading Or Getting Group A Streptococcal Infections
Even though there is no vaccine to prevent group A streptococcal infections, you can reduce your risk of getting an infection or spreading infection by having good hygiene. Good hygiene includes:
- Washing your hands with soap and water often.
- Covering your mouth and nose when you cough or sneeze.
- Throwing away your tissues after using them.
- Washing utensils, plates and glasses after someone who is sick uses them.
- Staying home if you feel sick.
- Cleaning and covering wounds until they heal.
Don’t Miss: Strep Throat And Ear Infection
Can Group A Streptococcal Infection Be Prevented
The best way to prevent group A streptococcal infection is to maintain good hygiene. To decrease the spread of bacteria, wash your hands often, especially after sneezing or coughing and before preparing, serving or eating food.
Ensure surfaces such as bathroom sinks, taps and door handles, as well as clothes and bedlinen, are kept clean to protect all the members of your household.
If you or your child have strep throat or another form of type A streptococcal infection, the infected person should stay home from pre-school, school or work for at least 24 hours after starting antibiotic treatment.
What Should You Do If You Think You Have Symptoms
Symptoms of a strep A infection include sudden fever, headaches, a sore red throat and a loss of appetite
The infection can also cause swollen lymph nodes and difficulty swallowing.
If these symptoms are persistent or severe then you should visit your GP, who may recommend an antibiotic.
Rachel Hearn, director of nursing and quality at Mid Essex CCG, told BBC News: The risk of contracting iGAS is very low for the vast majority of people and treatment with antibiotics is very effective if started early.
Recommended Reading: Common Prescription For Sinus Infection
How Can I Help My Child Feel Better
Home care can help your child feel better while battling strep throat. Give plenty of liquids to prevent dehydration, such as water or ginger ale, especially if your child had a fever. Avoid orange juice, grapefruit juice, lemonade, or other acidic beverages, which can irritate a sore throat. Warm liquids like soups, sweetened tea, or hot chocolate can be soothing.
For fever and pain, your doctor may suggest an over-the-counter medicine, such as acetaminophen or ibuprofen. Follow the package directions on how much to give and when.
Talk to your doctor about when your child can return to normal activities. Most kids can go back to school when they’ve taken antibiotics for at least 24 hours and no longer have a fever.
When Should I See My Doctor
Visit your doctor if you have a sore throat or skin sores or a wound that seems to spread or is not getting better. If you think you or someone you care for has a group A streptococcal infection, it is important to see a doctor as soon as possible. The infection can spread through the body and can become serious if not promptly treated with antibiotics.
Read Also: Ear Infection Causing Hearing Loss
Deterrence And Patient Education
As with any infection, whether it be viral or bacterial, isolation and avoidance of exposure are important to avoid contracting the infection. This is especially true in cases of impetigo, and strep pharyngitis as these infections are much more common in children. As such, children have a higher propensity to spread this infection through close contact with other children. Therefore, it is important for isolating known infections from close contact with others by having them remain home from school, daycare, etc. However, due to the fact that GAS is ubiquitous in our environment and part of our normal skin flora, there is really very little that can be done to completely avoid infection with GAS.
How To Prevent Strep Throat
Theres no vaccine available to prevent strep throat. One of the most effective ways to help avoid infection is regularly washing your hands. If you cant access soap and water, you can use a hand sanitizer instead.
Dont share drinks or food with someone who has strep throat. If someone in your home has strep throat, dont share their towels, sheets, or pillowcases. Wash dishes and laundry in water thats hot and soapy.
Parents of children with strep throat can help stop the spread to other family members by:
- keeping the childs eating and drinking dishes separate
- not sharing food, drinks, napkins, cloths, or linens between the child and others
- having the child cover all coughs and sneezes
- enforcing regular hand washing among everyone in the household
- replacing the childs toothbrush after the course of antibiotics ends
If you have strep throat, sneeze or cough into the crook of your elbow or a tissue rather than into your hand. Be sure to wash your hands frequently. Explore more ways to prevent strep throat.
Read Also: Best Pain Medicine For Tooth Infection
Children And Certain Adults Are At Increased Risk
Anyone can get strep throat, but there are some factors that can increase the risk of getting this common infection.
Strep throat is more common in children than adults. It is most common in children 5 through 15 years old. It is very rare in children younger than 3 years old.
Adults who are at increased risk for strep throat include:
- Parents of school-aged children
- Adults who are often in contact with children
Close contact with another person with strep throat is the most common risk factor for illness. For example, if someone has strep throat, the bacteria often spread to other people in their household.
Infectious illnesses tend to spread wherever large groups of people gather. Crowded settings can increase the risk of getting a group A strep infection. These settings include:
- Up to 3 in 10 children with a sore throat have strep throat
- About 1 in 10 adults with a sore throat has strep throat