Why Do Children Get Many More Ear Infections Than Adults Will My Child Always Get Ear Infections
Children are more likely than adults to get ear infections for these reasons:
- The eustachian tubes in young children are shorter and more horizontal. This shape encourages fluid to gather behind the eardrum.
- The immune system of children, which in the bodys infection-fighting system, is still developing.
- The adenoids in children are relatively larger than they are in adults. The adenoids are the small pads of tissue above the throat and behind the nose and near the eustachian tubes. As they swell to fight infection, they may block the normal ear drainage from the eustachian tube into the throat. This blockage of fluid can lead to a middle ear infection.
Most children stop getting ear infections by age 8.
What Are The Symptoms Of A Middle
Common symptoms of a middle-ear infection in adults are:
-
Pain in 1 or both ears
-
Drainage from the ear
-
Sore throat
You may also have a fever. Rarely, your balance can be affected.
These symptoms may be the same as for other conditions. Its important totalk with your health care provider if you think you have a middle-earinfection. If you have a high fever, severe pain behind your ear, orparalysis in your face, see your provider as soon as you can.
What Should I Expect If I Or My Child Has An Ear Infection
Ear infections are common in children. Adults can get them too. Most ear infections are not serious. Your healthcare provider will recommend over-the-counter medications to relieve pain and fever. Pain relief may begin as soon as a few hours after taking the drug.
Your healthcare provider may wait a few days before prescribing an antibiotic. Many infections go away on their own without the need for antibiotics. If you or your child receives an antibiotic, you should start to see improvement within two to three days.
If you or your child has ongoing or frequent infections, or if fluid remains in the middle ear and puts hearing at risk, ear tubes may be surgically implanted in the eardrum to keep fluid draining from the eustachian tube as it normally should.
Never hesitate to contact your healthcare provider if you have any concerns or questions.
Recommended Reading: Oil Of Oregano Pills For Yeast Infection
How Is An Ear Infection Diagnosed
Once youre at the doctors office, a medical professional will look inside your ear with an otoscope to determine whether you have an infection.
Typical signs include fluid buildup in the ear canal and middle ear, along with a red and inflamed eardrum.
Depending on the severity of your symptoms, your doctor may recommend waiting a few days to see if your ear infection improves.
Some infections resolve on their own. But if the infection is severe, or if symptoms dont improve after this time, then antibiotics may be warranted.
Chronic fluid buildup without an infection warrants additional testing from an ear, nose, and throat specialist.
Its especially important to diagnose young children so that they dont encounter speech and language delays from loss of hearing.
If your doctor recommends antibiotics to treat a severe ear infection, they will likely recommend an oral treatment, such as amoxicillin .
Which Antibiotic Is Best For An Ear Infection
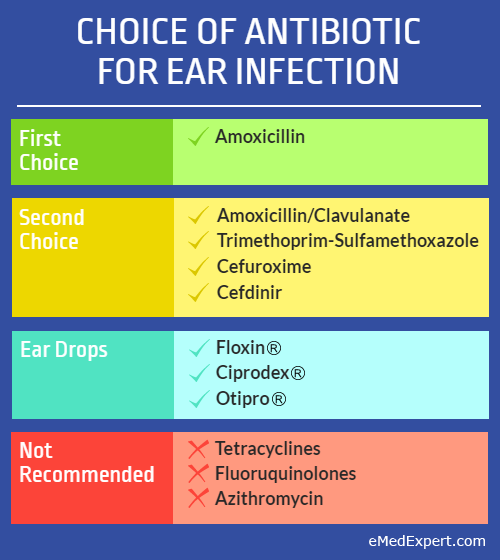
Two classes of antibiotics are commonly used to treat an infection.
Aminoglycosides
Aminoglycosides have been the main treatment for bacterial ear infections for decades. Two aminoglycosides used in ototopical preparations are:
- Neomycin
- Tobramycin
Though both of the above are commonly used in the United States, only neomycin has FDA approval. Neomycin is effective for gram-positive bacteria but its effectiveness against gram-negative bacteria has declined over years, especially against Pseudomonas, the most common bacteria in ear infections.
Tobramycin is effective for Pseudomonas and other gram-negative bacteria.
Quinolones
Quinolones are the most recently introduced ototopical antibiotics. Most quinolone antibiotics in use are fluoroquinolones, which also contain an atom of fluorine. Fluoroquinolones are considered the best available treatment now for ear infections for two reasons:
- Broad spectrum of activity against both gram-positive and gram-negative bacteria
- Lack of ototoxicity
Following are some of the FDA-approved fluoroquinolone solutions for external ear infection from Staphylococcus aureus and Pseudomonas aeruginosa:
Ciprofloxacin
Read Also: Antibiotics For Uti Bladder Infection
Who Cannot Take Antibiotics
It is very rare for anyone not to be able to take some type of antibiotic. The main reason why you may not be able to take an antibiotic is if you have had an allergic reaction to an antibiotic in the past. Even if you have had an allergic reaction to one antibiotic, your doctor or health professional will be able to choose a different type of antibiotic, which you will be able to take. If you are pregnant, there are certain antibiotics you should not take, but your health professional will be able to advise on which one is suitable if an antibiotic is needed. If you are on some medication, certain antibiotics may need to be avoided, or your regular medication stopped whilst you take the antibiotic. As above, when prescribed an antibiotic, make sure the prescriber knows about any other medication you take.
How to use the Yellow Card Scheme
If you think you have had a side-effect to one of your medicines you can report this on the Yellow Card Scheme. You can do this online at www.mhra.gov.uk/yellowcard.
The Yellow Card Scheme is used to make pharmacists, doctors and nurses aware of any new side-effects that medicines or any other healthcare products may have caused. If you wish to report a side-effect, you will need to provide basic information about:
- The side-effect.
- The name of the medicine which you think caused it.
- The person who had the side-effect.
- Your contact details as the reporter of the side-effect.
What Types Of Antibiotics Are Used
Swimmers ear is often treated with an antibiotic ear drop rather than an oral antibiotic.
For AOM, oral treatments such as amoxicillin are common. Oral antibiotics are usually prescribed to be taken for seven to 10 days. Make sure to always finish your antibiotics, even if you feel better before you run out.
Your doctor may not prescribe antibiotics at all, but rather opt to take a wait-and-see approach if your infection is mild. Recurring ear infections are sometimes treated surgically with ear tubes.
For more information or to schedule an appointment with experts, call Pinnacle ENT Associates today.
Don’t Miss: How To Deal With Tooth Infection Pain
What Are The Advantages Of Ototopical Antibiotics
Administration of antibiotics directly in the ear has several advantages over systemic delivery including the following:
Antibiotic concentration
Topical antibiotic solutions contain vastly greater concentration of antibiotic than the medications administered orally, or even intravenously. The high antibiotic concentration, delivered directly at the site of the infection, is much more effective in killing the bacteria. It also reduces the possibility for development of antibiotic-resistant bacterial strains.
The lowest level of drug concentration that can prevent bacterial growth is known as minimum inhibitory concentration . Some drug-resistant bacteria have a high MIC, but ototopical antibiotics far exceed the MIC required for destroying even highly resistant bacteria.
Absence of systemic effects
The absence of systemic effects with topical administration eliminates the risk of systemic antibiotic side effects. The normal beneficial bacteria that live in the respiratory and gastrointestinal tracts are unaffected. Absence of systemic antibiotics also prevents the natural selection and proliferation of drug-resistant bacteria.
Alteration of microenvironment
Donât Miss: Ears Ringing Alcohol
Dosage Intervals Of Amoxicillin For The Treatment Of Acute Middle Ear Infection
Acute middle ear infection is a very common disease in children and may cause pain and hearing loss. Delayed or ineffective treatment may lead to serious complications such as ear drum perforation, sensorineural hearing loss or the disease becoming chronic. Amoxicillin, with or without clavulanate, is the most commonly used antibiotic for treating acute otitis media. Currently, a reduction in the dosing interval to one or two daily doses is being used, in preference to the conventional three or four daily doses, to aid compliance.
We identified five randomised clinical studies with 1601 children comparing two dosing schedules. Participants were aged 12 years or younger with AOM. The primary outcome was clinical cure rate in terms of resolution of otalgia and fever at the end of antibiotic therapy . The secondary outcomes were clinical cure rate in terms of middle ear effusion during therapy, clinical cure rate post-treatment in terms of resolution of middle ear infection, AOM complications and adverse events to medication. The results showed that treating acute middle ear infection with either once/twice daily or three times daily amoxicillin, with or without clavulanate, has the same results using our outcome measures, including adverse events such as diarrhoea and skin reactions.
The evidence is current to March 2013.
We searched CENTRAL 2013, Issue 2, MEDLINE , EMBASE and the Science Citation Index .
Read Also: Medication For Middle Ear Infection
Why Are Children More Likely Than Adults To Get Ear Infections
There are several reasons why children are more likely than adults to get ear infections.
Eustachian tubes are smaller and more level in children than they are in adults. This makes it difficult for fluid to drain out of the ear, even under normal conditions. If the eustachian tubes are swollen or blocked with mucus due to a cold or other respiratory illness, fluid may not be able to drain.
A childs immune system isnt as effective as an adults because its still developing. This makes it harder for children to fight infections.
As part of the immune system, the adenoids respond to bacteria passing through the nose and mouth. Sometimes bacteria get trapped in the adenoids, causing a chronic infection that can then pass on to the eustachian tubes and the middle ear.
What Are The Treatments For Ear Infections
If your pediatrician recommends antibiotics, shell usually start with amoxicillin, an effective and safe antibiotic for bacterial infections that is one of the most commonly prescribed for young children. Whether or not your doctor opts for antibiotics or a watch-and-wait approach, rest and fluids are key as with any childhood respiratory infection or virus.
For pain relief at home, your pediatrician will usually recommend Acetaminophen for babies under 6 months and Acetaminophen or Ibuprofen for children 6 months and older. Remember that according to the CDC, over-the-counter cough medicines should not be given to children under 4 and should only be given to older children with your doctors approval. Recent research has shown that the negatives of these OTC medicines often outweigh any benefits.
Recommended Reading: Can Tooth Infection Cause Stomach Problems
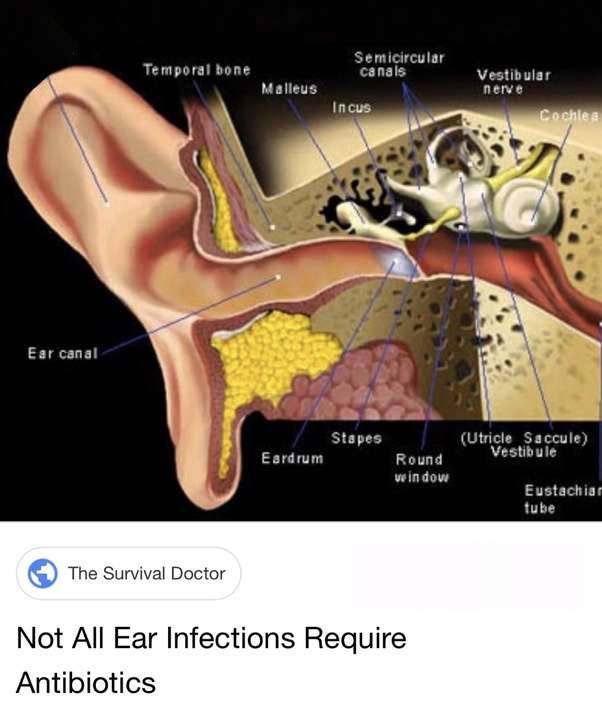
Where Is The Middle Ear
The middle ear is behind the eardrum and is also home to the delicate bones that aid in hearing. These bones are the hammer , anvil and stirrup . To provide the bigger picture, lets look at the whole structure and function of the ear:
The ear structure and function
There are three main parts of the ear: outer, middle and inner.
- The outer ear is the outside external ear flap and the ear canal .
- The middle ear is the air-filled space between the eardrum and the inner ear. The middle ear houses the delicate bones that transmit sound vibrations from the eardrum to the inner ear. This is where ear infections occur.
- The inner ear contains the snail-shaped labyrinth that converts sound vibrations received from the middle ear to electrical signals. The auditory nerve carries these signals to the brain.
Other nearby parts
- The eustachian tube regulates air pressure within the middle ear, connecting it to the upper part of the throat.
- Adenoids are small pads of tissue above the throat and behind the nose and near the eustachian tubes. Adenoids help fight infection caused by bacteria that enters through the mouth.
Antibiotic Treatment For Ear Infection
Antibiotic treatment for ear infections is an issue heavily debated by doctors. That debate is rooted in two arguments:
Ear infections are the most common type of childhood infections, affecting three out of four kids under the age of three.
Because so many children experience ear infections and because antibiotics are so often prescribed for treatment, many doctors worry that the bacteria is becoming resistant to the antibiotics. Some ear infections are caused by bacteria, in which case antibiotics can be effective. But others are viral, in which case antibiotics provide no defense. In addition, it is believed that four out of five ear infections will clear up on their own within a couple of days without antibiotic treatment.
As a result, the American Academy of Pediatrics released a new set of guidelines in 2013 for the antibiotic treatment of ear infections. Under the new guidelines:
-
Pediatricians are urged to only prescribe antibiotics if the patient displays severe pain and swelling for at least 48 hours, experiences an eardrum rupture, or has a fever higher than 102.2 Fahrenheit.
-
For all other patients, an alternative diagnosis and treatment mechanism is recommended. Sometimes pain relievers are prescribed to treat the symptoms of the ear infection without attacking the infection itself.
Don’t Miss: Sinus Infection Lower Tooth Pain
When Taking An Antibiotic
It is important to take antibiotics in the correct way. If you do not, this may reduce how well they work. For example, some antibiotics need to be taken with food and others should be taken on an empty stomach. If you do not take your antibiotics in the right way it will affect how much of them get into your body and therefore they may not work as well. So, follow the instructions as given by your doctor and on the leaflet that comes with the antibiotic you are prescribed.
Always take the entire course of antibiotics as directed by your doctor. Even though you may feel better before your medicine is entirely gone, follow through and take the entire course. This is important for your healing. If an antibiotic is stopped in mid-course, germs may be partially treated and not completely killed. Bacteria may then become resistant to that antibiotic.
Overuse of antibiotics has led to some bacteria changing their form or structure and becoming resistant to some antibiotics, which may then not work when really needed. For example, meticillin-resistant Staphylococcus aureus is a bacterium that has become resistant to many different antibiotics and is difficult to treat. Other bacteria produce chemicals called enzymes such as extended-spectrum beta-lactamases which allow them to be resistant to certain antibiotics.
Join The Drugscom Otitis Media Support Group
While you should only follow the medical advice of your doctor, you might consider joining the Drugs.com Otitis Media Support group to ask questions and share experiences with those who have similar questions and concerns about ear infections. You can also keep up with the latest ear infection news and approvals in the Drugs.com Otitis Media Support Group.
Related Topics
Read Also: Different Antibiotics For Tooth Infection
When To Talk To A Doctor
If you notice persistent ear infection symptoms that dont resolve on their own, call a healthcare professional.
This is particularly important for adults, as a middle ear infection can be a sign of a more serious problem in this age group compared to children.
And if you experience chronic ear infections, talk to your primary care provider, an otolaryngologist , or an otologist to discuss treatment options.
K Health articles are all written and reviewed by MDs, PhDs, NPs, or PharmDs and are for informational purposes only. This information does not constitute and should not be relied on for professional medical advice. Always talk to your doctor about the risks and benefits of any treatment.
K Health has strict sourcing guidelines and relies on peer-reviewed studies, academic research institutions, and medical associations. We avoid using tertiary references.
Hearing Loss And Speech Or Developmental Delay
Severe cases of recurrent acute otitis media or persistent otitis media with effusion may impair hearing for a period of time. But the hearing loss is not substantial or permanent for most children.
Hearing loss in children may temporarily slow down language development and reading skills. However, uncomplicated chronic middle ear effusion generally poses no danger for developmental delays in otherwise healthy children.
Rarely, patients with chronic otitis media develop involvement of the inner ear. In these situations, hearing loss can potentially be permanent. Most of these patients will also have problems with vertigo .
Also Check: Get Rid Of Chronic Yeast Infection
Who Should Take Oral Antibiotics For Ear Infections
- Children without ear tubes should take oral antibiotics for middle-ear infections, especially when they have severe ear pain or high fever.
- Children with ear tubes should take oral antibiotics if:
- They are very ill.
- They have another reason to be on an antibiotic.
- The infection doesnt go away with eardrops.
Treatment For Otitis Media With Effusion
Otitis media with effusion is fluid behind the middle ear . It usually resolves on its own without treatment, especially when it follows an acute ear infection. Antibiotics are not helpful for most cases of OME.
Clinical practice guidelines for OME recommend the following treatments:
- Watchful Waiting for OME. The child is typically monitored for the first 3 months. If OME lasts longer than 3 months, a hearing test should be conducted. Even if OME lasts for longer than 3 months, the condition generally resolves on its own without any long-term effects on language or development. The doctor will re-evaluate the child at periodic intervals to determine if there is risk for hearing loss.
- Drug Treatment. Antibiotics, decongestants, antihistamines, and corticosteroids do not help and are not recommended for routine management of OME. Antibiotic ear drops are helpful for treating ear infections that may occur in children with tympanostomy tubes. Topical antibiotics work better than oral antibiotics for treating the discharge that can occur with this type of infection.
- Surgery. Ear tube insertion may be recommended when fluid builds up behind your child’s eardrum and does not go away after 3 months or longer. Fluid buildup may cause some hearing loss while it is present. However, most children do not have long-term damage to their hearing or their ability to speak even when the fluid remains for many months.
Tonsillectomy is not recommended for OME treatment.
Read Also: Can You Get Over A Yeast Infection Without Treatment