How Can Hiv Status Be Confirmed If A Prep Patient Has Ambiguous Hiv Test Results At A Follow
If a patient has unclear HIV test results at a follow-up visit, providers can follow these steps to confirm the patients true HIV status:
- Wait 5-7 days and then draw a new blood specimen for repeat laboratory HIV testing using both an HIV antigen/antibody test and an HIV-1 RNA assay.
- If the repeat testing results show the patient has HIV, link the patient to HIV care and treatment. If the repeat testing results confirm that the patient does not have HIV, PrEP can be continued.
- If the results are still ambiguous, contact the PrEPline to get further testing advice and for linkage to a laboratory that can do specialized testing to confirm their HIV status.
While HIV status is being confirmed, providers have the following antiretroviral management options:
For patients using oral PrEP:
For patients using CAB injections:
- Pause CAB injections until testing shows that the patient does not have HIV.
- During the 12 weeks needed for additional HIV testing to determine HIV status, CAB is likely to remain at protective levels.
- If the patient has HIV, start HIV treatment immediately.
- If the patient does not have HIV, resume CAB injections every 2 months.
Since Prep Medication Alone Is Not Effective At Treating Hiv Is It Possible That Taking Prep Could Lead To My Developing Drug Resistant Hiv If I Become Infected Could It Lead To Higher Levels Of Drug Resistant Virus In The Community
HIV testing is a critical component when using PrEP for HIV prevention. HIV testing is done before a person begins PrEP to ensure that only HIV negative people are prescribed PrEP. Periodic HIV testing for everyone taking PrEP ensures that anyone who gets HIV will be identified quickly so they can be put on an effective treatment regimen. If a person on PrEP gets HIV, drug resistance testing is done to determine an effective treatment regimen. There is no evidence that PrEP can lead to higher rates of drug resistant virus in the community.
Frequency Of Hiv Infection Among Persons Taking Prep
Acquiring HIV infection by persons taking PrEP is uncommon. In 32 international open-label demonstration projects, Mera et al. reported 67 infections during 7061 cumulative person-years of FTC/TDF exposure for a seroconversion rate of 0.95/100 person-years of use . Marcus et al. reported no seroconversions during 5104 person-years of PrEP in an observational cohort in northern California . Thus, the expected frequency of new infections when patients are taking PrEP as prescribed is expected to be low, but the absolute number of new infections may increase as PrEP is more widely used.
Don’t Miss: Antiseptic For Urinary Tract Infection
Who Prep Is For
Anyone can get HIV. Your sex, age, sexual orientation, race, and ethnicity do not independently factor into your risk.
PrEP is for those considered to be at a high risk of HIV.
Reasons that put you at high risk include:
- You have a sexual partner with HIV or whose status is unknown
- You do not consistently use condoms
- You have sex in a region or network in which HIV is common
- You have been diagnosed with a sexually transmitted infection in the past six months
- You have a drug-injecting partner with HIV
- You share needles, syringes, or other equipment, such as cookers, to inject drugs
PrEP can be used by women trying to get pregnant or who are pregnant or breastfeeding and have a partner with HIV.
What Drugs Are Approved For Prep

There are two oral medications approved for daily use as PrEP. They are combinations of two anti-HIV drugs in a single pill:
- Truvada® is for all people at risk for HIV through sex or injection drug use. Generic products are also available.
- Descovy®) is for sexually active men and transgender women at risk of getting HIV. Descovy® has not yet been studied for HIV prevention for receptive vaginal sex.
A long-acting injectable form of PrEP, , has also been approved by the FDA. It is administered by a health care provider every two months instead of daily oral pills.
Read Also: Bath To Help Yeast Infection
When To Use Prep
If you are at a higher risk of contracting HIV due to your sexual activity or lifestyle, PrEP may be a good option for you. You may be at a higher risk if you are a man who has sex with other men, you are in sexual relationships with HIV-positive partners, or you use intravenous drugs.
Nurx offers PrEP for HIV prevention for as little as $0 with insurance for medication.
What Are The Side Effects Of The Prep Medications
All three approved medications, Truvada, Descovy and Cabotegravir, are recognized as well-tolerated medications with few side effects. In clinical trials, only a small number of people found the side effects serious enough to stop taking the medication. People taking PrEP should discuss any side effects they experience with their healthcare provider. In many cases, side effects are only short term and can be managed. Two important health issues related to taking PrEP include kidney function and bone density. Your healthcare provider will ask if you have a history of kidney disease and will periodically order lab work to monitor your kidney function. Bone density will be monitored as needed. The NYSDOH is aware that there are lawsuits that claim harm to individuals taking Truvada. However, scientific evidence shows that when taken as directed, Truvada is safe and effective. Since there are risks to taking any medication, individuals should speak with their healthcare provider about the benefits, risks , and possible alternatives for every medication they choose to take in order to understand the best choices for their specific situation.
Also Check: What Antibiotic Is Used For Dental Infection
Is It Ok To Switch Between Daily Prep And On
On-demand PrEP is only for cis-gender MSM. Other individuals are not eligible for on-demand PrEP because studies have not demonstrated that it is effective for other populations. Before switching from daily PrEP to on-demand PrEP, or vice versa, a cis-gender MSM should consult with their healthcare provider.
What Should I Tell My Healthcare Provider Before Taking Descovy For Prep
- All your health problems. Be sure to tell your healthcare provider if you have or have had any kidney or liver problems, including hepatitis.
- All the medicines you take, including prescription and over-the-counter medicines, vitamins, and herbal supplements. DESCOVY may interact with other medicines. Keep a list of all your medicines and show it to your healthcare provider and pharmacist when you get a new medicine.
You are encouraged to report negative side effects of prescription drugs to the FDA. Visit www.fda.gov/medwatch, or call 1-800-FDA-1088.
Recommended Reading: Can You Buy Antibiotics Over The Counter For Tooth Infection
Whats Treatment As Prevention
Treatment as prevention is a term that describes the use of antiretroviral therapy to prevent transmission of HIV.
AIDSinfo, a service of the U.S. Department of Health and Human Services, recommends that all people with HIV receive antiretroviral therapy.
Its important to begin antiretroviral therapy as soon as possible after a diagnosis. Early treatment can lower a persons risk of transmitting HIV as well as reduce their chances of developing stage 3 HIV, commonly known as AIDS.
How Should A Patient Who Acquires Hiv Infection While Taking Prep Be Managed
Once additional laboratory tests have confirmed infection, the following steps should be taken:
- Initiate treatment or refer for comprehensive HIV care.
- Counsel the patient about how to prevent HIV transmission to others and to improve their own health.
- Report the new HIV infection to the local health department.
Don’t Miss: Will Minocycline Treat Sinus Infection
Can I Get Pregnant If I Have Hiv
Some people think that HIV hurts your chances of getting pregnant, but this isnt true. If you have HIV and want to become pregnant, talk to your healthcare provider. Together you can make a plan before you try to get pregnant to keep you, your partner and any future children healthy.
HIV can spread to your partner during unprotected sex and to your baby during pregnancy, childbirth and breastfeeding. Taking ART medications can greatly reduce your risk of transmitting HIV to your baby, especially if you have an undetectable viral load. Your provider may recommend that you dont breastfeed your baby and use formula instead.
Who Can Use Prep
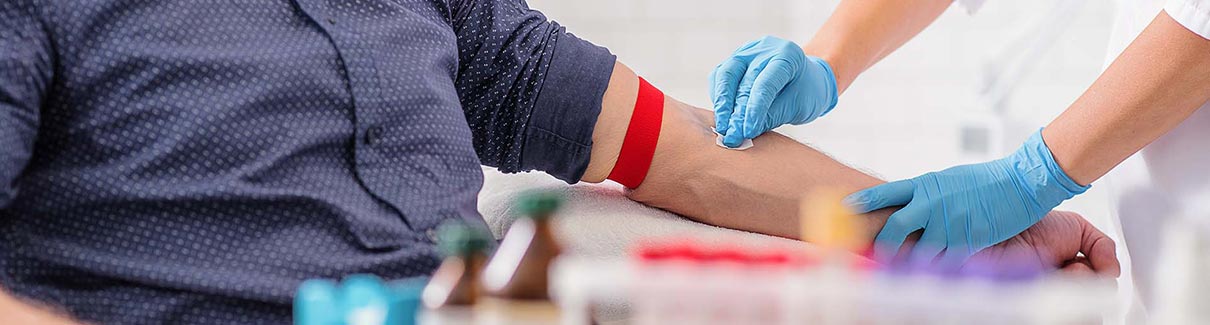
Anyone who is sexually active and doesn’t have HIV can use PrEP. To find out if PrEP is right for you, talk to your nurse or doctor. You may choose to use PrEP if you:
-
Have a sexual partner who has HIV
-
Dont regularly use condoms
-
Have been diagnosed with another STD within the last 6 months.
Have shared needles, syringes, or other equipment to inject drugs in the last 6 months.
Have used PEP multiple times.
If youre at high risk for HIV and youre pregnant, trying to get pregnant, or breastfeeding, PrEP may also help you and your baby avoid getting HIV.
PrEP isnt the same thing as PEP . PEP is a short-term treatment for people whove already been exposed to HIV within the past 72 hours. PrEP is generally an ongoing daily pill or bi-monthy shot for people who may be exposed to HIV in the future.
Don’t Miss: 8 Hour Infection Control Certificate
Can Adolescents Consent To Prep On Their Own Does A Healthcare Provider Need The Consent Of A Parent Or Guardian In Order To Prescribe Prep To An Adolescent
2017 amendments to NYSDOH regulations allow minors to consent to their own HIV treatment and HIV preventive services, such as PrEP and PEP, without parental/guardian involvement . The FDA has approved the use of Truvada for adolescents regardless of gender, and Descovy for adolescent cis-gender males. Injectable PrEP, CAB-LA, may be an option for adolescents who weigh at least 77 lbs. These developments, along with updated New York State Clinical Guidelines, mean that adolescents who are at risk for HIV may consent to PrEP without the involvement of the young persons parent or guardian.
Is Pep For Me
PEP will only be given if specialist doctors decide you are at a high risk for HIV infection if doctors decide you are not at high risk then you will not receive PEP. Caution: PEP is NOT a substitute for condoms.
If you are unsure of your level of risk you can get information on how HIV is transmitted here.
You May Like: How To Kill Mouth Infection
At What Stage Of The Infection Can Hiv Be Transmitted
If someone with HIV is taking HIV medication and has an undetectable viral load, they cannot pass on the virus. It can take up to six months on treatment to become undetectable.
Someone with HIV can pass on the virus if they have a detectable viral load.
This often happens during the first few months after infection when the levels of the virus in their body fluids are at their highest and they may not yet have been diagnosed.
This is why testing and early diagnosis are so important you can start treatment right away to protect your health and reduce your viral load to undetectable levels.
It can also happen when an object that has body fluids on it is put inside an HIV negative person during sex.
Getting The Conversation Started
If you think you may have higher chances of developing HIV, its important to discuss this and the steps you can take for protection from HIV with a trained healthcare professional.
Here are some things you can do to get a meaningful discussion started:
- Learn about the chances of contracting HIV from reputable sources like the CDC.
- Write down questions you want to ask a counselor or healthcare professional.
- Be open and share your concerns about HIV and your health experience.
- Ask where you can get tested regularly.
- Ask about where you can get PrEP medications in your area.
- If you dont have insurance, some state health departments offer free access to PrEP.
- Discuss how to share concerns with sexual partners about contracting HIV.
Also Check: Yeast Infection Clear On Its Own
What Should I Tell My Healthcare Provider Before Taking Truvada For Prep
- All your health problems. Be sure to tell your healthcare provider if you have or have had any kidney, bone, or liver problems, including hepatitis.
- If you are pregnant or plan to become pregnant. It is not known if TRUVADA can harm your unborn baby. If you become pregnant while taking TRUVADA for PrEP, tell your healthcare provider.
- If you are breastfeeding or plan to breastfeed. Do not breastfeed if you think you may have recently become infected with HIV. HIV can be passed to the baby in breast milk. Talk to your healthcare provider about the risks and benefits of breastfeeding while taking TRUVADA for PrEP.
- All the medicines you take, including prescription and over-the-counter medicines, vitamins, and herbal supplements. TRUVADA may interact with other medicines. Keep a list of all your medicines and show it to your healthcare provider and pharmacist when you get a new medicine.
- If you take certain other medicines with TRUVADA, your healthcare provider may need to check you more often or change your dose. These medicines include certain medicines to treat hepatitis B or C infection.
You are encouraged to report negative side effects of prescription drugs to the FDA. Visit www.FDA.gov/medwatch, or call .1-800-FDA-1088.
If I Drink Alcohol And/or Use Recreational Drugs Is It Safe To Take Prep
Alcohol and recreational drugs are not known to interact with PrEP medications. It is safe to take PrEP before, after and on days when you are âpartying.â In fact, it is important to take extra steps to make sure you take PrEP according to the healthcare providers directions when you are âpartying.â
Don’t Miss: How Effective Is Fluconazole For Yeast Infection
Prep Failure Or Test Failure
There is no reason to suspect PrEP failure in this case. The patient disclosed high-risk sex up to the time he started PrEP, including in the week between his first and second negative HIV tests. The most likely scenario is that he was infected a few days before starting PrEP or even the day or two afterwards, at the time PrEP drug levels were reaching maximum.
However, while this does not point to PrEP failure, it certainly points to test failure or at least a poor ability to detect HIV infection in a context where someone has just started PrEP. Our current tests may not be sufficiently sensitive or discriminating to detect HIV infection when the levels of HIV antigens and RNA may be suppressed by PrEP, and the resultant antibody response to them is very weak.
What Can I Expect If I Have Hiv
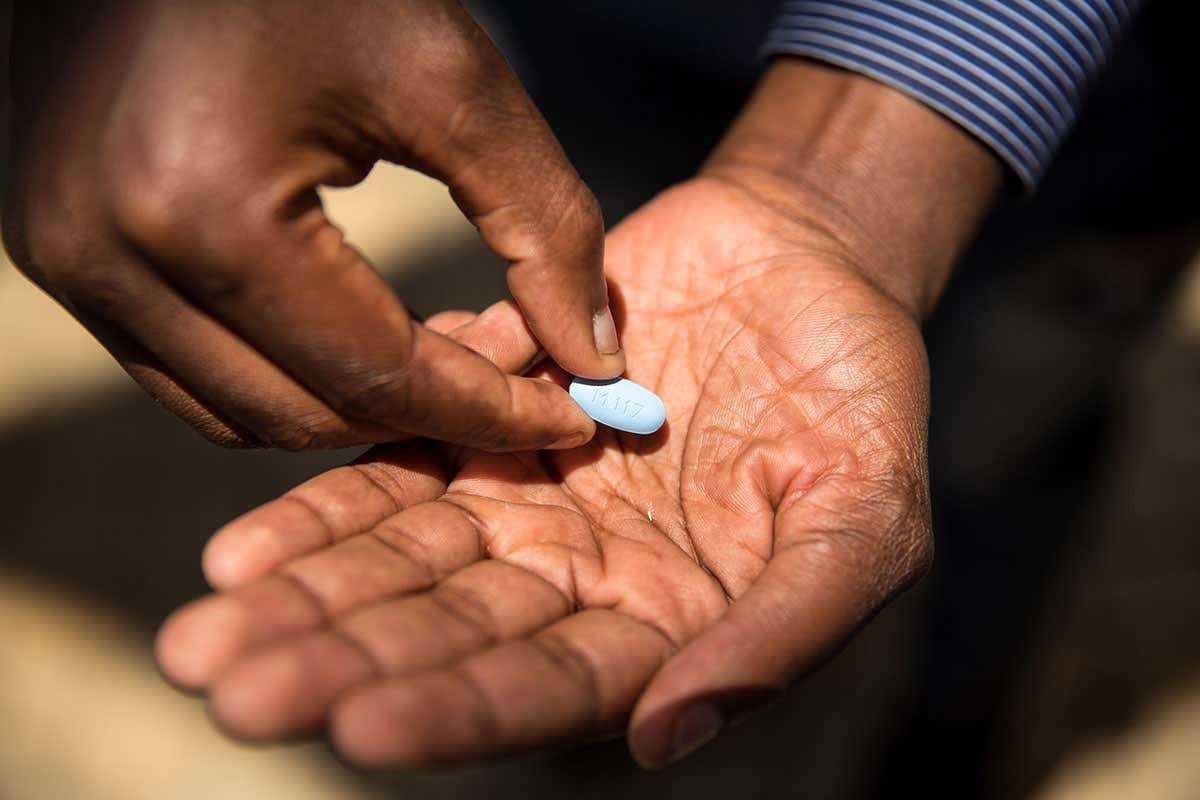
If youre diagnosed with HIV, its important to know that those living with HIV who follow treatment guidelines can live full lives for nearly as long as those without HIV.
If you have a high CD4 count and an undetectable viral load within a year of starting treatment, research suggests youll have the best outcomes, as long as you continue your treatment plan.
You can improve your outlook by:
- Getting tested as part of routine healthcare or if you think youve been exposed.
- Starting ART soon after being diagnosed.
- Taking your medicine every day.
- Keeping your appointments with your healthcare team.
ART can keep blood levels undetectable but cant entirely rid your body of the virus . If you dont take your medication every day, the virus can start multiplying again and mutate, which may cause your medications to stop working.
Left untreated, it can take about 10 years for HIV to advance to AIDS. If you progress to AIDS and it goes untreated, you can expect to live about three years more.
For those on treatment, if you have a high CD4 count and undetectable viral load within a year of starting treatment, you can expect to live about as long as someone without HIV. If you have a low CD4 count or a detectable viral load within a year of starting treatment, you may live 10 to 20 years less than someone without HIV.
You May Like: Strongest Antibiotic For Dental Infection
Who Is Prep For
PrEP is for HIV-negative people at risk of HIV infection. Such as:
- Men who have sex with men without using a condom.
- Having a sexual partner who is HIV-positive and not on treatment or they are at high risk of getting HIV.
- You are sexually active and inconsistently use condoms.
PrEP isnt necessarily for everyone and is a personal choice. Your circumstances and your risk of being exposed to HIV should all play a role in deciding whether PrEP is right for you.
Speak with your doctor to see if PrEP is your best option to prevent HIV.
A Note On Gonorrhoea Resistance
Gonorrhoea resistance causes significant concern and may be one of the most significant medical risks of increased STI prevalence. The Neisseria gonorrhoeae bacterium easily becomes resistant to antibiotics. Originally treated with sulphonamides and then penicillin in the 1940s, gonorrhoea became progressively resistant to those drugs and then to tetracycline and ciprofloxacin, which replaced them.
As the proportion of gonorrhoea resistant to ciprofloxacin in the UK climbed to 50% in gay men and 20% in heterosexuals, a switch was made to a whole new class of antibiotics the cephalosporins. A single drug from this class, cefixime, was used for first-line treatment of gonorrhoea starting in 2006.
However, the proportion of gonorrhoea with resistance to cefixime rapidly increased in gay men from about 5% in 2008 to 31% in 2010. As a result, in 2011 the recommended therapy changed, to dual combination therapy. This combined another cephalosporin, ceftriaxone, with the macrolide drug azithromycin.
Emphasising this as the only approved regimen for gonorrhoea, and guarding against over-treatment, appeared to have positive results both in the US, where rates of resistance to ceftriaxone fell tenfold between 2011 and 2014, and in Europe, where in the UK and Belgium resistance to both drugs halved between 2011 and 2014. No cases of ceftriaxone-resistant gonorrhoea were detected in Europe in 2016, compared with seven in 2013.
Recommended Reading: Urinary Tract Infection Water Retention