Hiv Diagnoses Declining Among African American Women
From 2011 to 2015, the number of HIV diagnoses among Black/African American women fell 20%, which is indeed encouraging and movement in the right direction that we want to sustain. That data signal that we are on track to meet our National HIV/AIDS Strategy target for reducing the disparity in the rate of new HIV diagnoses among Black women by at least 15% by 2020. However, Black women continue to be diagnosed with HIV at disproportionately high rates relative to White and Hispanic/Latina women. In 2016, 4,560 Black women were diagnosed with HIV, representing 61% of HIV diagnoses among all women in the United States that year.
Resources With More Information
A number of organizations on the local, state, and federal levels are addressing HIV in Black communities. Many more privately owned grassroots organizations are addressing concerns every day.
Black AIDS Institute , for example, is a Los Angeles-based nonprofit dedicated to ending the HIV/AIDS epidemic in the Black community. BAI was founded by three Black gay doctors, including one who is living with HIV. It is the only Black HIV organization working to improve the health of Black people in America through research, advocacy, and policy work.
On the federal level, hundreds of millions of dollars have been committed to bolstering HIV data collection and prevention efforts, and strengthening the capacity and improving the performance of the nations HIV prevention workforce.
The U.S. government has shared its desire to end HIV in the nation by 2030. Through its Lets Stop HIV Together campaign, the CDC offers resources about HIV stigma, testing, prevention, and treatment and care. This campaign is part of the Ending the HIV Epidemic in the U.S. initiative.
How Common Is Hiv In The Us 2020
Over one billion are believed to exist today.U.S. doctors care for more than 2 million people who live with HIV.Each year, more than 35,000 people are infected with HIV.Since the beginning of the AIDS epidemic, more than 6,000 people have died.U.S. citizens live in more than 700,000 households.Those who have died with HIV and AIDS are mostly children.
Also Check: Eye Infection Not Pink Eye
Key Points: Hiv Incidence
HIV incidence declined 8% from 2015 to 2019. In 2019, the estimated number of HIV infections in the U.S. was 34,800 and the rate was 12.6 .
, the annual number of HIV infections in 2019, compared with 2015, decreased among persons aged 1324 and persons aged 45-54, but remained stable among all other age groups. In 2019, the rate was highest for persons aged 25-34 , followed by the rate for persons aged 35-44 .
, the annual number of HIV infections in 2019, compared with 2015, decreased among persons of multiple races, but remained stable for persons of all other races/ethnicities. In 2019, the highest rate was for Blacks/African American persons , followed by Hispanic/Latino persons and persons of multiple races .
, the annual number of new HIV infections in 2019, as compared to 2015, decreased among males, but remained stable among females. In 2019, the rate for males was 5 times the rate for females .
, the annual number of HIV infections in 2019, compared with 2015, decreased among males with transmission attributed to male-to-male sexual contact, but remained stable among all other transmission categories. In 2019, the largest percentages of HIV infections were attributed to male-to-male sexual contact
For more details on recent HIV incidence statistics, see Estimated HIV Incidence and Prevalence in the United States, 2015-2019.
Hiv Symptoms In Black Males
While some people living with HIV may detect symptoms of their infection early on, many are unaware of their status for many months. In the first few weeks after initial infection you may experience no symptoms or mistake your symptoms for another illness, like the flu or the common cold.
Symptoms of acute HIV infection are often flu-like and include:
- Fever
- Sore throat
Read Also: Planned Parenthood Treat Yeast Infections
Community And Government Outreach Programs
In 2018, the federal government announced an ambitious plan to eliminate HIV by 2030. The proposal includes the following initiatives:
- Funding existing prevention programs
- Providing HIV prevention medication to those at highest risk in hot spots across the U.S. and Puerto Rico
- Identifying where the virus is spreading in real time and deploying resources to those areas
- Creating an HIV HealthForce to support these efforts nationwide
While feasible, these efforts have failed to address the systemic issues that have allowed the virus to persist in Black communities.
On the plus side, various groups, including federal, state, and local organizations, have launched vigorous outreach programs in Black communities to inform and treat hard-to-reach people at risk of contracting the virus. This has resulted in consistent declines in the number of deaths and rates of death among Black Americans infected with HIV.
What Cdc Is Doing
CDC is pursuing a high-impact HIV prevention approach to maximize the effectiveness of HIV prevention interventions and strategies. Funding state, territorial, and local health departments and community-based organizations to develop and implement tailored programs is CDCs largest investment in HIV prevention. This includes longstanding successful programs and new efforts funded through the Ending the HIV Epidemic in the U.S. initiative. In addition to funding health departments and CBOs, CDC is also strengthening the HIV prevention workforce and developing HIV communication resources for consumers and health care providers.
- Under the integrated HIV surveillance and prevention cooperative agreement, CDC awards around $400 million per year to health departments for HIV data collection and prevention efforts. This award directs resources to the populations and geographic areas of greatest need, while supporting core HIV surveillance and prevention efforts across the US.
Also Check: Will Tooth Infection Go Away On Its Own
The Miseducation Of The Young Black Gay Man
With National Black HIV/AIDS Awareness Day on February 7, we take a look at how the epidemic continues to devestate the African American community.
When I was a young baby gay on the come up, AIDS was everywhere. Figuratively. There were posters in my school, there were special episodes on TV, there were ribbons on every Gucci lapel of every red carpet. The threat of AIDS was in movies and in music, in the very air, a cautinoary pall hanging over my youth. I still feel a tinge of sadness whenever I watch TLC’s “Waterfalls” and the shirtless dude just disappearsthose three letters having taken him to his final resting place. Never understood why it wasn’t four letters, but I digress.
There was an active anti-AIDS propoganda campaign in full motion during my adolesence and it worked. The ’90s and ’00s saw a sharp decline in HIV infections and coupled with advances in treating people with AIDS, by the time PrEP rolled around the threat of AIDS didn’t seem so, well, threatening.
But no tea, no shade, HIV/AIDS is still very much a threat. Which is why Feburary 7 is National Black HIV/AIDS Awareness Day.
According to the CDC, African Americans are the racial/ethnic group most affected by HIV in the US, with gay and bisexual men accounting for more than half of estimated new HIV diagnoses.
Related | HIV/AIDS in the Black Gay Male Community is at an Exceptional High
Below, some sobering facts from the CDC on the impact of HIV/AIDS on the black community:
Prevention Benefits Of Hiv Treatment Not Fully Realized
People living with HIV who know their status, are in care and on antiretroviral therapy that results in a suppressed or undetectable viral load are living longer, healthier lives. They are also preventing sexual transmission of HIV to their partners. Thats because we now know that people living with HIV who take HIV medications daily as prescribed and achieve and maintain an undetectable viral load have effectively no risk of sexually transmitting the virus to an HIV-negative partner. We also know that if someone who has achieved and maintained an undetectable viral load stops taking HIV medications the viral load will rebound quickly . When this occurs, someone who had effectively no risk of transmission can have a high or very high virologic potential for transmitting HIV.
But all who are living with HIV in the United States are not sharing these dual benefits of HIV treatment equally. We know that too few African Americans living with HIV are receiving HIV care and achieving and maintaining a suppressed viral load. The latest CDC data indicate that only 59% of African Americans living with HIV received HIV medical care in 2014 with fewer retained in care, and even fewer still achieving a suppressed viral load.
You May Like: What Antibiotic For Ear Infection In Adults
Hiv Among African Americans
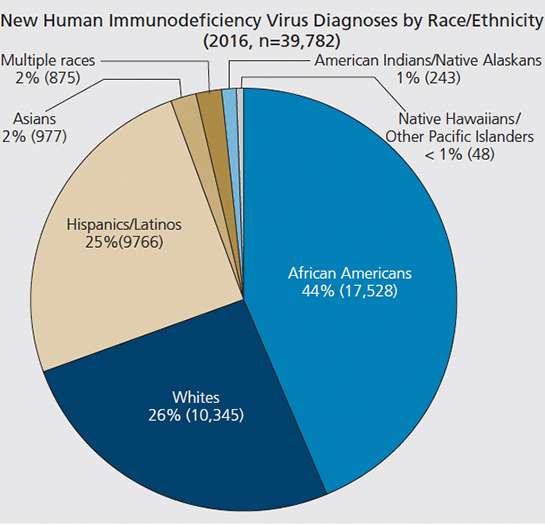
Blacks/African Americans1 account for a higher proportion of new HIV diagnoses, those living with HIV, and those who have ever received an AIDS diagnosis, compared to other races/ethnicities. In 2016, African Americans accounted for 44% of HIV diagnoses, though they comprise 12% of the U.S. population.2
How Hiv Became Treatable
This article is published in collaboration with The Conversation.
It has been almost 35 years since the world was introduced to the term AIDS. In the 1980s, researchers and physicians were trying to understand what was causing waves of strange infections and discovered it was a new virus called the human immunodeficiency virus, or HIV. Since that time, HIV has gone from a death sentence to a manageable chronic disease. Today, it is estimated that 1.2 million people living with HIV in the United States and 50,000 Americans are infected with HIV every year.
Thanks to treatment advances, people with HIV can and do live long and full lives. And that has led to a challenge that doctors and patients in the 1980s and early 1990s may not have imagined: the aging HIV patient.
And yet, while we have a treatment regimen that can keep people living with HIV well, and even prevent transmission of the virus, many people, both in the US and overseas, cant access it.
How did HIV become manageable?
But these drugs still had the same problems that made pre-1996 treatment so tough: a lot of pills, taken all day long. And it was expensive. Initially this kind of treatment was accessible only to people living in developed countries who could afford to pay the high cost of these medicines.
Better treatment and longer lives
A lifetime of treatment
Excellent treatment is available, but not everyone gets it
Read Also: Can Amoxicillin Be Used For Tooth Infection
Roles For All Of Us To Address These Disparities
Our fight against HIV is not over. Our continued efforts must include a focus on reducing the HIV-related disparities experienced by Blacks/African Americans. Working together to make the most effective and efficient use of the tools we now have to fight it, we can accelerate on our course to ending HIV in the United States.
Topics
I found this page helpful because the content on the page:
I did not find this page helpful because the content on the page:
What can we do to improve this page?
Key Points: Hiv Diagnoses
Gay, bisexual and other men who have sex with men b are the population most affected by HIV in the U.S.:
- MSM accounted for 69% of new HIV diagnoses in the United States.c
- From 2015 through 2019 in the United States and 6 dependent areas, Black/African American MSM accounted for more than 36% and White MSM accounted for more than 30% of HIV diagnoses among MSM annually.
- In 2019, Black/African American MSM accounted for 26% of new HIV diagnoses and 37.9% of diagnoses among all MSM.
- In 2019, Hispanic/Latinod MSM made up 22% of new HIV diagnoses and 32.5% of diagnosis among all MSM.
The number of HIV diagnoses decreased among MSM overall, but trends varied by race/ethnicity. From 2015 through 2019:
- Among MSM aged 1324 years, HIV diagnoses decreased or were stable among all racial/ethnic groups.
- HIV diagnoses increased among American Indian/Alaska Native and Native Hawaiian/other Pacific Islander MSM, ages 24 and older.
Transgender people accounted for approximately 2% of new HIV diagnoses in 2019.
- From 2015 through 2019 in the United States and 6 dependent areas, the number of diagnoses of HIV infection for transgender adults and adolescents increased.
- In 2019, among transgender adults and adolescents, the largest percentage of diagnoses of HIV infections was for transgender male-to-female people.
Blacks/African Americans and Hispanics/Latinx continue to be severely and disproportionately affected by HIV:
Read Also: Will Minocycline Treat Sinus Infection
Hiv Statistics By Race
Black or African American and Hispanic or Latino communities continue to be disproportionately affected by HIV compared to other racial/ethnic groups.
| Disparity in HIV by Race/Ethnicity | |
|---|---|
| Race | |
| 1.3% | 0.3% |
Of note, some subpopulations within racial and ethnic minority groups are more affected by HIV than others. For example, gay, bisexual, and other Black men who have sex with other men, accounted for 26% of new HIV infections and Latinos who identify similarly accounted for 22% of new HIV infections, despite making up 2% of the U.S. population.
Better Deploying Highly Effective Biomedical Interventions Is Key To Addressing Disparities
The science is clear. The key to lowering new HIV infections among all people, including African Americans, will require taking full advantage of the advances that research has provided and making the most efficient and effective use of the tools now available. Treatment as prevention and pre-exposure prophylaxis are the most powerful tools in our HIV toolkit. Yet, too many people are not aware of these new tools and the latest data on their effectiveness, so work needs to be done to educate many more people about the latest science.
Read Also: Otc Oral Yeast Infection Treatment Cvs
Women And Young People
- Among all women, Black women account for the largest share of new HIV diagnoses , and the rate of new diagnoses among Black women is 14 times the rate among white women and almost 5 times the rate among Latinas.24 Black women also accounted for the largest share of women living with an HIV diagnosis at the end of 2017.25
- Although new HIV diagnoses continue to occur disproportionately among Black women, data show a 43% decrease in new diagnoses for Black women between 2008 and 2018.26
- In 2018, Black women represented about one quarter of new HIV diagnoses among all Blacks a higher share than Latinas and white women .27
- In 2016, more than half of gay and bisexual teens and young adults with HIV were black.28
- According to a national survey of young adults ages 18-30, about three times as many Blacks as whites say HIV today is a very serious concern for people they know. Almost twice as many Black young adults say they know someone who is living with, or has died of, HIV/AIDS, compared to whites .29
Reasons That Explain Hiv Rates In Black Men
A number of challenges contribute to this observed disparity, including poverty, lack of access to healthcare, higher rates of some sexually transmitted infections , smaller sexual networks, lack of awareness of HIV status, and stigma.
Despite the public health communitys best efforts to counter the notion that HIV infection is the result of personal irresponsibility or being immoral, these beliefs are pervasive in some communities, causing shame and a reluctance to access healthcare services.
The medical community is not left without blame, as the focus of outreach has long been centered around mitigating high-risk sexual practices, and not the many social determinants of health that contribute to the transmission of this deadly disease.
Due to these factors, myths and misinformation have increased the stigma and discrimination surrounding HIV and AIDS. Therefore, increasing access to care while removing the stigma of HIV may be the best way to connect Black men to the care they need.
Don’t Miss: Uti Bladder Or Kidney Infection
The Hiv Epidemic In The United States Cont
The CDC tracks diagnoses of HIV infection information for 7 racial and ethnic groups: American Indian/Alaska Native, Asian, Black/African American, Hispanic/Latino, Native Hawaiian/Other Pacific Islander, White, and Multiple Races. Among these groups, the African American and Latino populations are disproportionately affected by HIV disease, with African Americans experiencing the greatest per-capita burden of the epidemic.
- Although African Americans comprise approximately 14% of the US population, 44% of new HIV infections reported in 2009 were among African Americans:
- Approximately 1 in 16 African American men and 1 in 32 African American women will be diagnosed with HIV infection at some point in their lives.
- In 2009, the estimated rate of new HIV infections among African American men was 6.5 times as high as that of white men and more than 2.5 times as high as those of Latino men and black women. Moreover, the estimated rate of new HIV infections among African American women was 15 times that of white women and > 3 times that of Latina women.
- Although Latinos comprised 16% of the US population, they accounted for 20% of new HIV infections in 2009.
- In 2009, the estimated rate of new HIV infections among Latino men was 2.5 times that of white men, with the rate among Latina women at 4.5 times that of white women.
Data include persons with a diagnosis of HIV infection regardless of stage of disease at diagnosis.
A Hispanic/Latino person can be of any race/ethnicity.
Ethnicity And Health In America Series: Hiv Among African
HIV among African-Americans.
In honor of Black History Month, the Ethnicity and Health in America Series is highlighting HIV in the African-American community. Our focus on HIV among African-Americans this month coincides with a national focus on HIV among Black Americans. February 7, is National Black HIV/AIDS Awareness Day, designed to get the African American community to understand the extent to which it is infected and affected by HIV. Prevalence rates for HIV infection among African Americans have now reached epidemic proportions:
-
African-Americans make up approximately 14 percent of the population of the United States. Yet in 2009, African Americans accounted for 44 percent of the new HIV/AIDS diagnoses.1
-
African American men account for 70 percent of the new infections, so that 1 in 16 black men and 1 in 32 black women will be diagnosed at some point in their lifetime.
-
Thus, the number of African Americans living with HIV infection was found to be almost eight times higher than the rate for their Caucasian counterparts.
-
African Americans with HIV/AIDS are dying at a disproportionately high rate nearly 10 times the rate of Whites.1
1CDC, 2011
Washington PostAIDS: DCs Silent Stalker of Women
Examining the social determinants of health such as poverty, education, poor access to health care, social justice and unemployment are essential in understanding this disparity . For instance, discrimination and stigmatization are influential from diagnosis to treatment:
Recommended Reading: Lemon Water Good For Bladder Infection