Tooth Infection Treatment: Are Antibiotics The Best Option
A tooth infection, sometimes called a dental infection or a dental abscess, is a condition that occurs when bacteria enter a damaged tooth or the gums around it. The bacterial infection triggers an immune system response, which leads to swelling, inflammation, or pus, a thick fluid of dead tissue, bacteria, and white blood cells. If the condition progresses, pus can accumulate within the infected area, forming an abscess or pocket of pus near the affected tooth or teeth.
Dental infection symptoms vary according to the severity of the infection and may include throbbing or persistent tooth pain, fever, sensitivity to hot or cold food, bad breath, a discolored tooth, difficulty swallowing, or swelling in your jaw, neck, cheeks, or gums. Although modern dentistry and oral health practices have made most dental infections less concerning than they once were, the condition can become serious and even life-threatening if left untreated.
If you believe you have a tooth abscess, seek treatment right away. Some infections may require a procedure to drain pus, fill a cavity, or remove an infected tooth, and some, but not all, infections may benefit from antibiotics. In rare cases, severe infections may require intravenous antibiotics or surgery. Your dentist or healthcare professional may also recommend over-the-counter medications to help manage any pain.
Tooth Infection Treatment: Whatre Your Options
To treat a tooth abscess, your dentist will perform an exam and often take an x-ray to locate your infection and determine its severity and whether it has spread. Based on these findings, treatment options may include:
- Draining the abscess:Your dentist or healthcare provider will administer a local anesthetic and then create an incision in the abscess to drain the pus.
- Performing a root canal treatment:Your dentist will administer an anesthetic and then drill into your infected tooth to remove the pus collected in its interior. After they clean the area, they will fill, seal, and cap the tooth to complete the root canal procedure and ensure that no more bacteria can enter.
- Extracting the tooth:Your dentist may recommend extracting a tooth if it is too damaged to save. Once they pull your tooth, they will drain the area of any remaining pus to treat the abscess and relieve your pain.
In most cases, the American Dental Association recommends that dentists treat abscesses and other causes of dental pain with appropriate dental procedures and pain relievers, not antibiotics.
To manage your pain, your dentist may suggest taking over-the-counter pain relievers like ibuprofen , acetaminophen , or naproxen before or after your dental procedure.
Relieving Pain From A Dental Abscess
While you’re waiting to see a dentist, painkillers can help control your pain.
Ibuprofen is the preferred painkiller for dental abscesses, but if you’re unable to take it for medical reasons, you can take paracetamol instead.
Aspirin should not be given to children under 16.
If 1 painkiller does not relieve the pain, taking both paracetamol and ibuprofen at the doses shown in the medicine leaflet may help.
This is safe for adults, but not for children under 16.
It may also help to:
- avoid hot or cold food and drink if it makes the pain worse
- try eating cool, soft foods if possible, using the opposite side of your mouth
- use a soft toothbrush and temporarily avoid flossing around the affected tooth
These measures can help relieve your symptoms temporarily, but you should not use them to delay getting help from a dentist.
Read Also: Can Urgent Care Test For Yeast Infection
Treating Gum Disease With Antibiotics
For those of our patients at Champlin Family Dental who suffer from periodontal disease, we proudly offer topical or oral antibiotics to help reduce or entirely eliminate disease-causing bacteria. It can also help fight the bacterial infection causing gingivitis, a mild form of periodontal disease that is characterized by reddening, swelling, and bleeding of the gums.
Doctors Bauer, Lawrenz, and Stark may recommend systemic or topical antibiotics in conjuncture with scaling and root planing, as well as other procedures. These antibiotics include:
Most forms of gum disease can be treated without antibiotics, but the biggest advantage of using topical antibiotics to help treat the disease is that they are directed to their specific target areas, thus the entire body is not affected. The other advantages of topical antibiotics include reduced dosage and reduced side effects. Doctors Bauer, Lawrenz, and Stark can discuss with you the advantages, as well as side effects, of each antibiotic during your visit.
To learn more, or to schedule your next visit at Champlin Family Dental, please give us a call today at our convenient Champlin, MN office!
Tags:
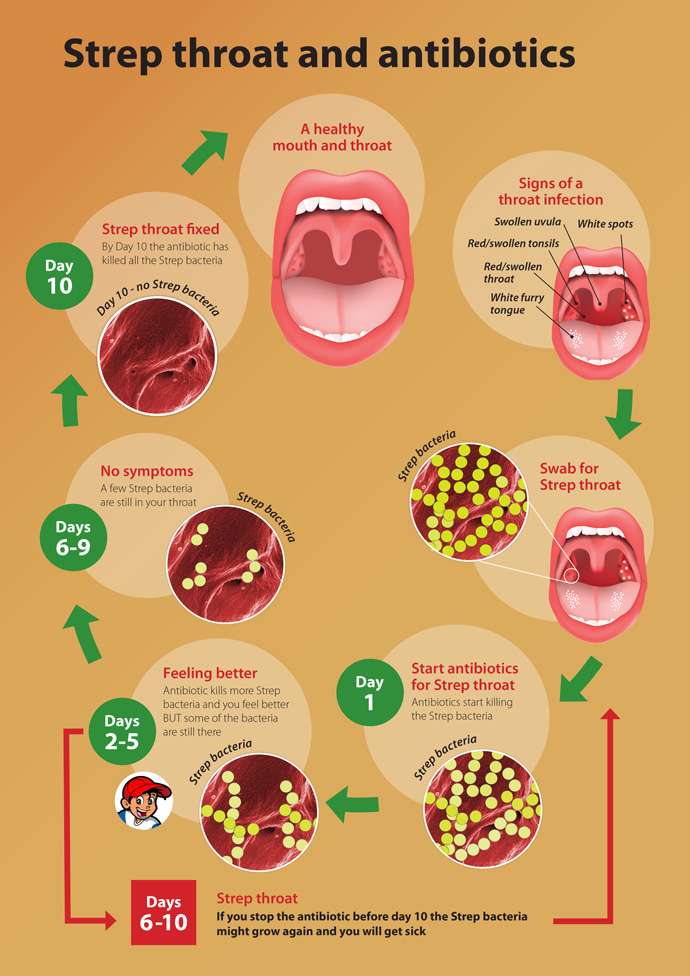
When To See A Doctor For A Throat Infection
Since many sore throats are just a symptom of a virus like a cold or the flu, which should clear up by itself, you dont need to run to the doctor as soon as your throat feels scratchy.
If you experience any of these symptoms, though, its time to contact a doctor:
- Severe sore throat
- It hurts to breathe or youre experiencing shortness of breath
- Difficulty opening your mouth
- A high fever
- Skin rash
- Blood in saliva or phlegm
- Sore throat lasts more than a week
- Dark urine, rash, or chest pain
Don’t Miss: Best Over The Counter Skin Yeast Infection Treatment
Are Antibiotics An Effective Way To Prevent Infection Following Tooth Removal
What is the problem?
Teeth that are affected by decay or gum disease or painful wisdom teeth are often removed by dentists. Tooth extraction is a surgical procedure that leaves a wound in the mouth that can become infected. Infection can lead to swelling, pain, development of pus, fever, as well as dry socket .
These complications are unpleasant for patients and may cause difficulty with chewing, speaking, and teeth cleaning, and may even result in days off work or study. Treatment of infection is generally simple and involves drainage of the infection from the wound and patients receiving antibiotics.
Why is this question important?
Antibiotics work by killing the bacteria that cause infections, or by slowing their growth. However, some infections clear up by themselves. Taking antibiotics unnecessarily may stop them working effectively in future. This antimicrobial resistance is a growing problem throughout the world.
Antibiotics may also cause unwanted effects such as diarrhoea and nausea. Some patients may be allergic to antibiotics, and antibiotics may not mix well with other medicines.
Dentists frequently give patients antibiotics at the time of the extraction as a precaution in order to prevent infection occurring in the first place. This may be unnecessary and may lead to unwanted effects.
What did we want to find out?
What did we do?
What we found
Main results
How reliable are the results?
What does this mean?
How up-to-date is this review?
Replenishing The Antibiotic Pipeline And Developing Other New Therapies
Because antibiotic-resistant bacterial strains continue to emerge and spread, there is a constant need to develop new antibacterial treatments. Current strategies include traditional chemistry-based approaches such as natural product-based drug discovery, newer chemistry-based approaches such as drug design, traditional biology-based approaches such as immunoglobulin therapy, and experimental biology-based approaches such as phage therapy,fecal microbiota transplants,antisense RNA-based treatments, and CRISPR-Cas9-based treatments.
Recommended Reading: Common Urinary Tract Infection Antibiotics
Antibiotic Coverage During The Endodontic Procedure
The most conventional therapy in case of dental abscess requires two different procedures. First the dentist has to drain the bump to allow the pus to come out. To do that, your doctor will puncture the boil containing the yellowish fluid and press it gently to get it all out. As soon as the pus starts to exit, you will feel immediately.
The second step has the scope to remove all the infected material from within the dental element. The clinician will use surgical instruments like files and reamers to clean and shape the root canal. At this point, antibiotics for abscess avoid that additional bacteria contaminate the surgical area.
What Are The Most Common Symptoms Of A Tooth Infection
If youve never had an infected tooth before, you might be wondering how youd know if your tooth was infected. Pain is often the most common sign of a tooth infection. Unfortunately, this pain isnt always confined to the tooth itself. Because our teeth are connected to so many nerves, pain from an infected tooth can extend into the jaw, face, and neck. Talk about discomfort!
Other signs to look for include:
-
Tooth sensitivity to heat, cold, and/or pressure
-
Tenderness around the tooth
-
Swelling of the mouth, jaw, or face
If you have a dental abscess that bursts open on its own, you might taste a strong, salty fluid that could also smell bad.
Read Also: Can I Infect Someone While On Prep
When Does A Toothache Require Antibiotics
When the dental infection is severe or impacts the gum around an erupting tooth, your dentist may recommend antibiotics. For instance, pericoronitis is an infection in the gum tissue that can develop around impacted wisdom teeth. Patients with this condition may be given antibiotics as part of their treatment.
Additionally, if your dentist notices signs of a dental abscess a tooth infection that can develop from an untreated cavity, they may recommend antibiotics.
Complications Of Dental Abscess
In rare cases, complications do arise. These can include:
- Cellulitis, an infection of the skin and subcutaneous tissues.
- Ludwigâs angina, which occurs when cellulitis spreads into the tissues under the tongue, in the lower jaw and under the chin. It is also known as submandibular cellulitis/submandibular space infection.
- Osteomyelitis, an infection of underlying bone.
- Parapharyngeal abscess, an abscess at the back of the mouth, near the throat. It is caused by staphylococcal and/or streptococcal bacteria. It is most common in children aged five years or younger.
- Cavernous sinus thrombosis, which can occur when the infection spreads into the blood vessels in the sinuses of the head.
These conditions require very urgent medical attention and are best evaluated via a hospital emergency department.
Also Check: How To Heal Tooth Infection Without Antibiotics
Antibiotic Prophylaxis For Dental Work
Your dentist may prescribe preventative antibiotics for certain dental services or before the treatment of your dental infection this is called antibiotic prophylaxis.
During certain dental treatments, the bacteria that reside in your mouth may enter the bloodstream, and prophylactic antibiotics can prevent infection.
Causes Of Dental Abscesses

Dental abscesses are the result of bacterial infection. When the gum tissue surrounding a tooth becomes damaged or the tooth itself is damaged, bacteria that are already in the mouth and, under usual circumstances not harmful, may enter the area and cause infection.
One of the most common causes of damage to the teeth and gums is poor dental hygiene, such as inadequate brushing and flossing, high sugar or carbohydrate consumption, and lack of regular checkups at the dentist. These factors may lead to dental caries or cavities, gingivitis and periodontitis, which can admit bacteria to the inside of the tooth or the gum. Maintaining healthy teeth and gums is therefore one of the best ways of reducing the risk of developing dental abscesses, as it removes one of the main causes of abscesses.
Recommended Reading: Natural Medicine For Kidney Infection
What Are The Symptoms Of A Dental Infection
Depending on the location and extent of the infection, dental infection symptoms can range from mild to severe. If you have a tooth infection, you may experience one or more of the following symptoms:
- A lump or bulge around the infected tooth
- Throbbing or persistent pain around the infected tooth
- Throbbing or constant pain that radiates to your jaw, neck, or ear
- Pain in your face
- Red, swollen, or bleeding gums
- A swollen mouth or face
- Sensitivity to hot or cold temperatures
- Tenderness or sensitivity to touch around the infected tooth
- A discolored or loose tooth
- Bad breath or a foul taste in your mouth
- Difficulty opening your mouth
If a tooth infection goes untreated, bacteria can spread and infect areas of your jaw, face, head, or neck. In rare instances, your infection can develop into a serious skin infection or blood infection . Symptoms of a tooth infection spreading to body parts outside the mouth include:
- Feeling generally ill or unwell
If you experience these symptoms, seek medical attention from a healthcare provider immediately.
Antibiotics For Tooth Abscess Complication
A deep neck infection is a dangerous complication of tooth infection when it spreads into the space between neck muscles. An abscess forms inside the neck. The abscess may swell and block breathing or swallowing.
Deep neck infections are treated in the hospital with an intravenous antibiotic along with opening the space in the neck to drain the abscess. For this type of infection, the best antibiotic may be amoxicillin with clavulanate through an IV.
The antibiotic for a deep neck infection may change if a lab culture shows that bacteria are more sensitive to another antibiotic .
Don’t Miss: Are There Different Types Of Uti Infections
The Difference Between An Abscess And An Infection
A tooth infection can take the form of a cavity, pulpitis, or an abscess. Yes, a dental cavity is an infection. It causes the enamel, or hard surface, of the tooth to begin to break down. This can be painful, if it happens quickly, but many cavities dont cause symptoms.
If the infection extends into the middle of the tooth the pulp it causes pulpitis. This usually causes a toothache, which can be aggravated by hot and cold foods and liquids.
Finally, if the infection is not treated and continues to spread, it can form an abscess. After the infection has spread through the middle of the tooth and has nowhere else to go, it forms a pocket of pus, which is an abscess.
Treatments For A Dental Abscess
Dental abscesses are treated by removing the source of the infection and draining away the pus.
Depending on the location of the abscess and how severe the infection is, possible treatments include:
- root canal treatment a procedure to remove the abscess from the root of an affected tooth before filling and sealing it
- removing the affected tooth this may be necessary if root canal treatment is not possible
- incision and drainage where a small cut is made in the gum to drain the abscess
Local anaesthetic will usually be used to numb your mouth for these procedures.
More extensive operations may be carried out under general anaesthetic, where you’re asleep.
Antibiotics are not routinely prescribed for dental abscesses, but may be used if the infection spreads or is particularly severe.
Also Check: What If A Yeast Infection Goes Untreated
Using Oral Antibiotics For Gum Infection
If you are provided antibiotics in oral type, you will take them for 7 to 10 days.
Your dental professional likewise can place an antibiotic straight into the affected parts of your mouth. This is called local therapy. It can take numerous kinds, including:.
- Gel: Your dental expert injects a gel including doxycycline under your gums. The area is sealed and covered with an unique plaster called a periodontal pack. After 7 to 10 days, your dentist removes the plaster and any staying gel.
- Powder: Your dental professional squirts a powder including minocycline under your gums. The powder liquifies over 3 weeks.
Periostat is another kind of pill that sometimes is used. It consists of doxcycline at extremely low levels. It does not eliminate bacteria. Rather, it reduces the bodys immune-system action to the bacteria. This response is what causes gums and bone to become swollen and damaged. Minimizing the immune action helps to stop bone from dissolving. Patients typically take Periostat for 6 months or more to manage bone loss.
If your dental practitioner owns a dental laser, it will be used after root planing and scaling. The dental practitioner places the laser tip in the space in between your tooth and gum, then moves it around the whole tooth. This process begins from the base of each pocket. The dental professional can treat your whole mouth at one time. This will remove the bacteria in the pockets throughout your mouth.
Parapharyngeal Abscesses And Ludwigs Angina
Parapharyngeal abscesses and Ludwigâs angina can both cause swelling severe enough to obstruct the airways and cause difficulty breathing. Parapharyngeal abscesses require a and needle aspiration to diagnose. Ludwigâs angina is diagnosed by, needle aspiration and X-rays.
Treatment for Ludwigâs angina, parapharyngeal abscess, osteomyelitis, cellulitis and cavernous sinus thrombosis involves drainage of any pus that is present, possibly via surgery and antibiotics and possibly intravenous antibiotics. People affected by Ludwigâs angina, if untreated, may require a tracheostomy to open their airways and thereby help them breathe if the swelling obstructs the windpipe.
Also Check: How To Tell Tooth Infection
Are There Effective Home Remedies That Treat Tooth Infections
While there are no home remedies for a tooth infection, your dentist or healthcare provider may suggest that you use home remedies such as the below in addition to their recommended treatment plan to ease your symptoms:
- Rinsing your mouth with saltwater, swishing with a baking soda solution, or using hydrogen peroxide as a mouthwash may help kill bacteria and promote healthy gums.
- Applying a cold compress to the infected part of your face may reduce pain and swelling.
- Over-the-counter tooth pain gels, clove oil, and pain medications such as ibuprofen and acetaminophen may help relieve pain.
How To Ward Off Any Dental Infection
- Brush your teeth every day at least twice. It is highly recommended to brush your teeth after every meal. Replace your toothbrush atlease every three months.
- Use dental floss to remove any food that stuck between the teeth
- Restraint eating food that contains too much sugar in the night before going to bed.
- Fluoridated drinking water helps. Fluoride strengthens your teeths enamel, making it more difficult for bacteria like plaque and tartar to enter. Most cities in the US have fluoride in their drinking water.
- Visit the dentist at least once in two months.
Your best way to get rid of tooth infection is without antibiotics. Help yourself to stop tooth pain fast.
Also Check: Lupin 500 For Tooth Infection