How K Health Can Help
Did you know you can get affordable primary care with the K Health app?
to check your symptoms, explore conditions and treatments, and if needed text with a doctor in minutes. K Healths AI-powered app is HIPAA compliant and based on 20 years of clinical data.
K Health articles are all written and reviewed by MDs, PhDs, NPs, or PharmDs and are for informational purposes only. This information does not constitute and should not be relied on for professional medical advice. Always talk to your doctor about the risks and benefits of any treatment.
K Health has strict sourcing guidelines and relies on peer-reviewed studies, academic research institutions, and medical associations. We avoid using tertiary references.
Ways To Tell If You Are Living With An Infected Tooth
Are you suffering from a debilitating toothache? Perhaps youve noticed a little gum or jaw swelling, or your tooth seems to be a different color? It could be a serious tooth infection.
Your teeth are packed with nerves. Thats why a toothache, though it may only affect one part of your mouth, is excruciating. Whats more, the pain may sometimes be related to a deeper oral health issue.
If your tooth feels sore, sensitive, or youre experiencing sharp pains in your mouth, you may have a tooth infection or a tooth abscess.
Why a tooth becomes infected
There are a number of causes of tooth infections. One of the most common causes is older root canals. When you have a root canal, your dental professional removes a nerve from the affected tooth. Unfortunately, bacteria can grow in that area, leading to an infection that your body struggles to fight off.
Its important to recognize the signs of an infection, so you can seek immediate treatment.
How to tell if your tooth is infected
How to cure a tooth infection
Common Antibiotics Used For A Tooth Infection
Penicillin-type drugs, such as amoxicillin and penicillin V potassium, are typically the first-line antibiotics that dentists prescribe to treat a tooth infection.
However, allergic reactions to penicillins are common. If you have a history of allergy symptoms after taking penicillin-type drugs, let your dentist know. They may prescribe a macrolide antibiotic, such as clindamycin, to clear up your infection.
In some cases, your dentist may prescribe another type of antibiotic, such as:
These drugs are typically prescribed if other antibiotics dont work to treat your symptoms or if your tooth infection begins to spread.
Read Also: Can Augmentin Be Used For Tooth Infection
What Are The Symptoms Of An Abscessed Tooth
In some cases, the area around the tooth hurts, but not always. If it does, itâs usually a sharp, throbbing pain, especially when you put pressure on your tooth. It might also spread to your jaw or other parts of your face on the side thatâs affected.
You might also notice:
- Sensitivity to hot or cold temperatures
- Puffy gums
- A bad odor when you chew with that tooth
Sometimes an abscess causes a pimple-like bump on your gum. If you press it and liquid oozes out, itâs a sure bet you have an abscessed tooth. That liquid is pus.
If you have swelling in your face and a fever, or you have trouble breathing or swallowing, go to the emergency room. The infection may have spread to other parts of your body.
Prevention Of Pulp Disease
When the pulp of the tooth gets sick and you have a toothache, you need a dental specialist who is experienced and trained to perform root canal therapy at the highest level. Dr. Steven Lipner the founder of Midtown Endodontist NYC is a brilliant caring doctor who uses a cutting-edge microscope to ensure wonderful outcomes for his patients. In his gifted hands, you will experience a treatment that is precise, pleasant, and perfect. Midtown Endodontist NYC is here when you need us.
About Dr. Steven Lipner
You May Like: Boric Acid For Urinary Tract Infection
What Is The Pulp
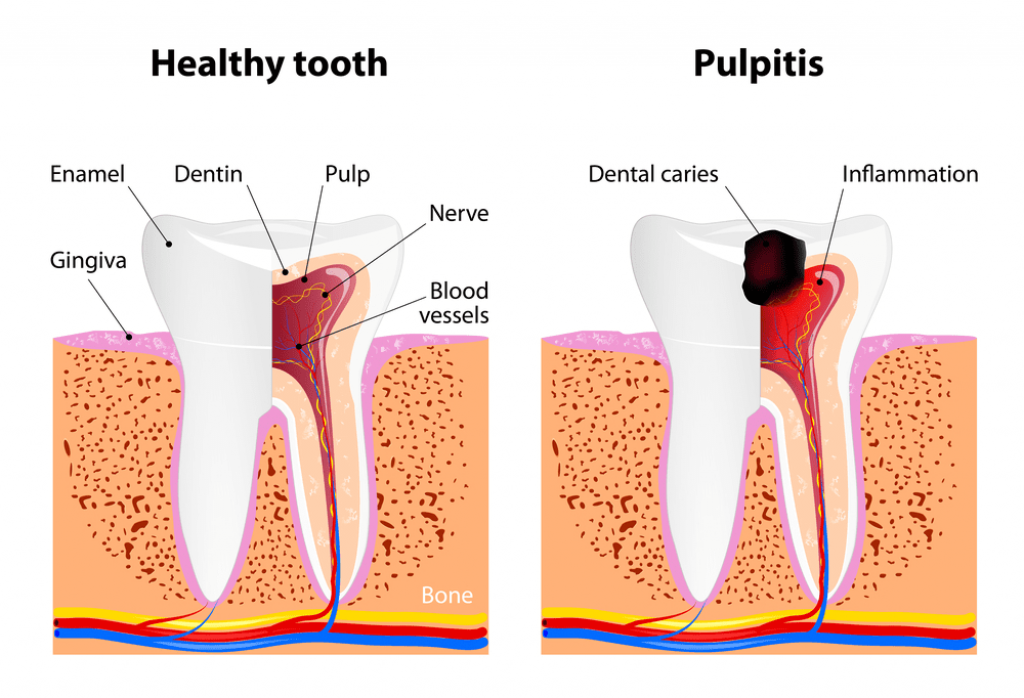
Pulp is a gelatinous organic material composed of connective tissue, nerves, artery and vein that occupies the tooths center in a hollow cavity called the pulp chamber. The pulp is the heart of the tooth, providing blood to the tooths root.
The tooths pulp is surrounded immediately by dentin, which comprises the largest part of the tooth. Enamel, the hardest substance in the body, is the thin outer covering of the tooth that protects the dentin and the pulp. The pulp produces new dentin and gives the tooth sensation from heat, cold, sweetness and pressure. The protection of this part of our tooth is crucial.
However, several things can broach the pulp chamber and damage the pulp:
- Caries, or deep cavities
- Bruxism, or grinding ones teeth
How Do You Treat Pulp Stones
4.3/5pulp stonestreatmentanswered comprehensively
Pulp stones generally do not have significant clinical implications as they are usually not a source of pain, discomfort or any form of pulpitis. However, when the tooth concerned will undergo endodontic treatment such as root canal treatment, presence of large pulp stones will be clinically significant.
Similarly, what causes pulp calcification? The dental pulp calcification presents as masses of calcified tissue present on the level of the pulp chamber and roots of the teeth. The formation of pulp stones has also been associated with long-standing irritants such as caries, deep fillings, and chronic inflammation.
Hereof, how common are pulp stones?
However, a recent retrospective study of adult patients examined by cone-beam computed tomography found pulp stones in approximately 32% of individuals and 10% of teeth, with the maxillary and mandibular molars most frequently affected.
How do you remove pulp from teeth?
A partial pulpectomy is when the dentist removes only the damaged portion of the pulp or all the pulp in the upper chamber of the tooth without touching the roots. Once the damaged pulp is removed, the tooth is cleaned, disinfected, and filled. A partial pulpectomy is also called pulpotomy, or pulp therapy.
You May Like: At Home Ear Infection Care
What Are The Risk Factors
Anything that increases the risk of tooth decay, such as living in an area without fluoridated water or having certain medical conditions, such as diabetes, may increase the risk of pulpitis.
Children and older adults may also be at increased risk, but this is largely determined by quality of dental care and oral hygiene habits.
Lifestyle habits may also increase the risk for pulpitis, including:
- poor oral hygiene habits, such as not brushing teeth after meals and not seeing a dentist for regular checkups
- eating a diet high in sugar, or consuming foods and drinks which promote tooth decay, such as refined carbohydrates
- having a profession or hobby that increases your risk of impact to the mouth, such as boxing or hockey
- chronic bruxism
What Causes A Dead Tooth
A dead tooth is caused by pulp necrosis or tooth necrosis. Pulp necrosis results from a chronic or acute infection that can be caused either by severe decay that gets close to the dental pulp, pulpitis that reaches the root of the tooth or physical trauma to the pulp. The pulp is the nerve inside the tooth that ensures the nourishment of the tooth.
If these problems are not treated quickly and effectively, the pain they cause will not be felt in the long term. This can give the illusion of being healed, when in fact no healing is taking place at all.
You May Like: Online Prescription For Sinus Infection
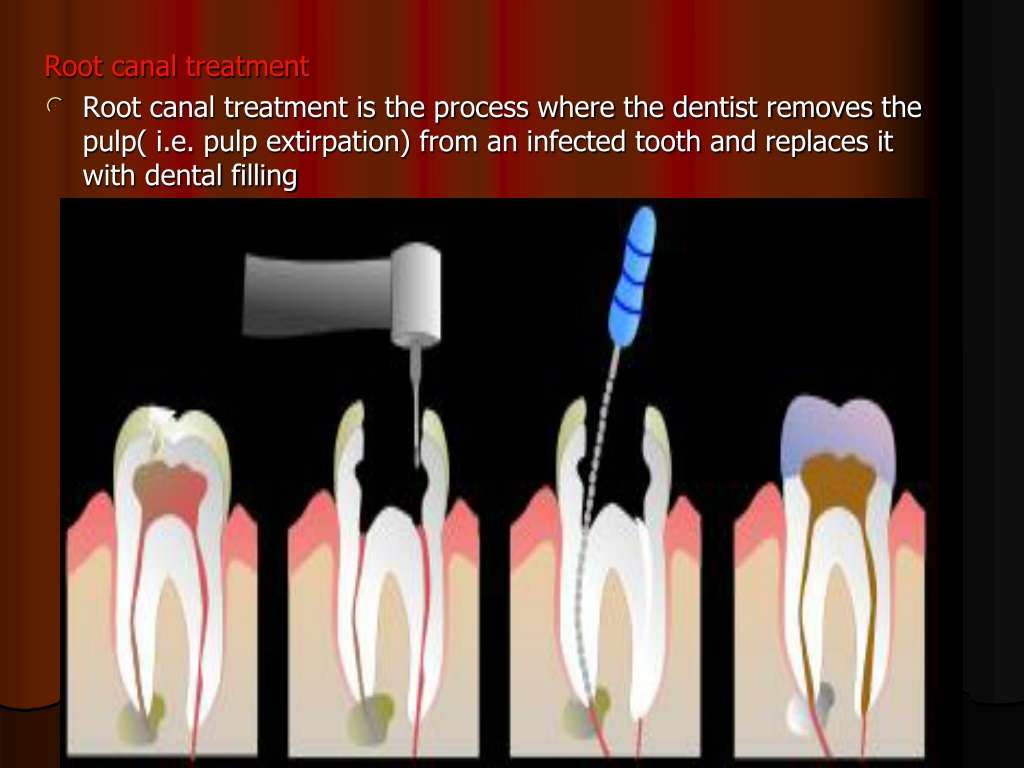
What To Expect From A Root Canal
If you have been to the dentist and it has been determined that you need a root canal, there are situations where your dentist can prescribe an antibiotic to buy you some time. Even with this antibiotic, the issue will not go away, and you will still need the procedure within a few weeks to fully eliminate the infection of your tooth.
When you have decided to undergo a root canal, you can expect the procedure to take a couple of hours to complete. In some severe cases, it can take longer. First, a local anesthetic will be applied to numb the area around the infected tooth, after which a hole will be drilled so that the center of the tooth can be accessed. Once the infected pulpal tissue has been removed, the tooth will be sealed. Your tooth will be severely weakened from this process, resulting in the need for a crown to be put over the tooth. A crown will protect the tooth so that it can be saved from extraction.
Despite what you may have heard, this entire process is not something to be feared. Local anesthetic ensures that the experience is comfortable to you and not much different than getting a filling.
Symptoms Of Tooth Infection Spreading To The Brain
A dental abscess can also travel to the brain, leading to the development of another abscess. If the infection reaches your brain, it can be life-threatening.
Since a brain abscess is so dangerous, the condition requires a visit to the hospital or emergency room for urgent treatment. A brain abscess is relatively rare but can occur if the dental infection is left untreated.
Symptoms of a brain abscess :
- Fever
- Going in and out of consciousness
Summary
Dental abscesses can lead to brain abscesses . This is why you should never leave them untreated. Vision changes and body weakness on one side are common with brain abscesses.
Can an Infected Tooth Make You Sick?
Poor oral hygiene and neglected dental care allow the harmful bacteria in your mouth to cause infections. Eventually, an untreated tooth infection can make you sick.
If left untreated, a dental abscess can have serious consequences on your oral health and entire body.
Don’t Miss: Can Clarithromycin Be Used To Treat A Urinary Tract Infection
Swollen Or Tender Lymph Nodes
The lymphatic system runs throughout the body and acts as a waste removal system, getting rid of cellular waste. When there is infection or inflammation in the body the lymph nodes can swell or become hard. If you suddenly have lumps under your jaw or in your neck that are hard to the touch, you may have inflamed lymph nodes, which could mean you have an infection.
You May Like: Can Ketoconazole Treat Yeast Infection
How A Dentist Will Treat A Tooth Infection
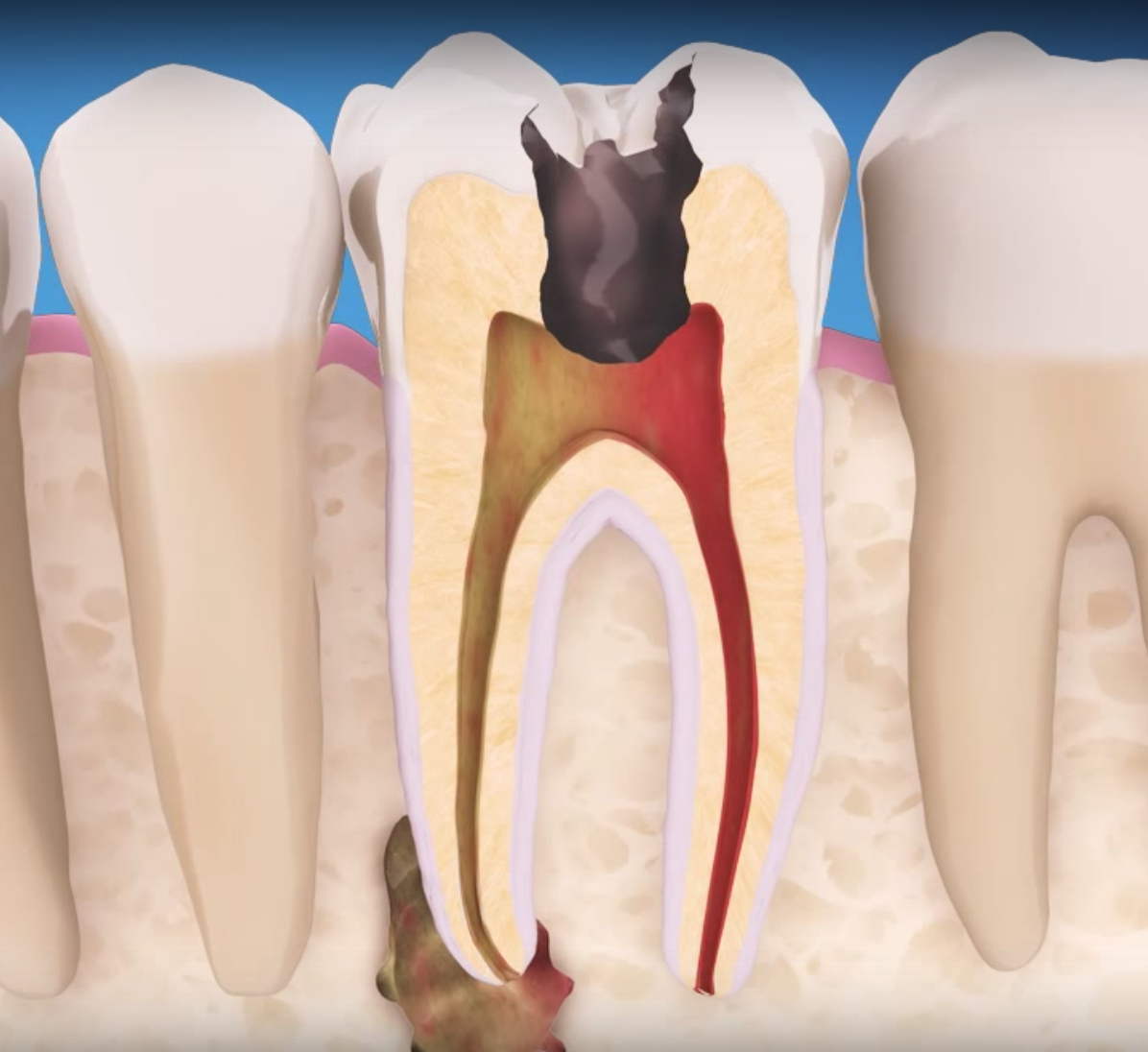
Once a dentist has determined that you have an infection, the dentist can work to treat the infection, clear out any abscesses that have formed, and assess the damage. You will usually be given a prescription for antibiotics too. If there are abscesses in the tooth or in the gums near the tooth the dentist will go in and clean those pockets out to get rid of the bacteria. Often that can provide immediate relief from the pain of an infected tooth. The dentist will also check your teeth to see if you will need a root canal in order to save the tooth.
Read Also: How Many Doses Of Fluconazole For Yeast Infection
What Are The Causes
In a healthy tooth, the enamel and dentin layers protect the pulp from infection. Pulpitis occurs when these protective layers are compromised, allowing bacteria to get into the pulp, causing swelling. The pulp remains trapped inside the tooths walls, so the swelling causes pressure and pain, as well as infection.
The enamel and dentin layers can become damaged by several conditions, including:
- cavities or tooth decay, which causes erosion to the tooth
- injury, such as an impact to the tooth
- having a fractured tooth, which exposes the pulp
- repetitive trauma caused by dental issues, such as jaw misalignment or bruxism
Devitalization Of The Infected Tooth By Root Canal Treatment
The first treatment option is a root canal. This procedure consists of devitalizing the tooth, i.e. removing the infected dental pulp from the tooth. This prevents the infection from penetrating deeper into the tooth or infecting other nearby tissues.
However, a devitalized tooth becomes more fragile. Your dentist will probably recommend covering it with a crown to protect it from any potential damage.
Recommended Reading: Amox Clav For Ear Infection
How Does A Root Canal Get Infected
The most common way a root canal becomes infected is due to a deep cavity. If this cavity is not treated promptly, it can spread and infect other parts of the mouth.
The infection usually starts in the pulp tissue. This soft layer in the tooths center contains nerves and blood vessels. If the infection spreads beyond the root, it may lead to other infections in other parts of the mouth.
Here are some swelling symptoms that may point to root canal infections:
- Swelling that lasts for a long period of time
- A gum pimple-like boil situated in front of or on the root tip
- The tooth that feels a bit taller than adjacent teeth
- A recurring pimple that forms on the gums
- Pronounced swelling.
You May Like: How To Tell If Tooth Infection Is Spreading
More Severe Cases Require Tooth Extraction
If pulp necrosis is not promptly treated, the infection can spread to the jawbone area. In addition, the structure of the tooth may be severely weakened, preventing it from being reconstructed. These are examples of situations where tooth extraction will be appropriate. Afterwards, a dental implant will be required to restore the appearance, comfort and functionality of the tooth.
Don’t Miss: How Did I Get An Ear Infection
Get Root Canal Therapy From Midtown Endodontist Nyc
After reading this post, you may be able to figure out if you need a root canal. If you are unsure, talking to a professional is always the most effective solution. Midtown Endodontist NYC has highly trained doctors who are specialists in this area of dentistry and friendly staff who love to help patients with all their root canal-related questions. Call us today at or book an appointment online to get your teeth treated!
About Dr. Steven Lipner
Removing An Infected Tooth
If infected pulp goes untreated, an abscess can form. This happens when the infection grows and the bacteria leaks out of the pulp chamber into the space between the tooth and jaw bone. A swollen and painful lump will form on the gum above the infected tooth. In very serious cases, the infection can spread to the jaw bone, ear, sinuses, or neck. In rare, serious cases, patients can even develop sepsis.
When pulp infection is extensive, or if an abscess has formed, its sometimes an indication that the tooth and its roots are dead. Extracting the tooth is often the only option. The lump that results from an abscess is filled with infected fluid. The dentist or endodontist first step will be to drain it. Antibiotics may be prescribed to stop the infection from spreading any further.
Don’t Miss: Urinary Tract Infection Detection Kit
How Is An Infected Dental Pulp Treated
Do you find yourself too tired to brush your teeth? Maybe, youre always canceling dental appointments. This combination can lead you to miss the early signs of tooth decay or other issues that may require a root canal in Charleston SC. When tooth decay isnt treated right away, it can lead to infection. Furthermore, it doesnt just affect the outer layer of your tooth. The bacteria in your decayed tooth can penetrate the pulp chamber, which is the area found in the center of your tooth that houses connective tissues, blood vessels, and nerves.
Your dentist may recommend a root canal treatment if your dental pulp is infected. Often times, you may be asymptomatic. Regardless if you show symptoms or not, you should trust your dentists recommendation to stop the infection from spreading.
Infected Root Canal Warning Signs
When you are concerned that you may have an infection after having a root canal performed, then knowing the warning signs is essential to your good overall health. Root canals are often a necessary procedure in order to save a tooth at risk of being lost. Even though root canal complications tend to be few and far between, they do exist. This makes it essential for you to pay close attention to any warning signs that may be present.
Recommended Reading: Ways To Cure Bladder Infection
Dont Panic Get It Taken Care Of Today
If you suspect that you have a dental issue that can only be resolved with a root canal, dont worry. Root canals, though not at the top of anyones list of a great time, are common and dont have to be painful. With the right dentist, the experience doesnt have to be a scary one.
The truth is, it hurts a lot more to continue on with a damaged tooth or teeth than to undergo a root canal procedure. In fact, most patients say the procedure was painless. Though you can expect to feel some minor aches and sensitivity once the anesthetic wears off, these small discomforts will subside within a couple of weeks.
The best thing to do is call your dentist and schedule an appointment today to get your teeth healthy again.
How To Diagnose A Gum Abscess
If you experience gum pain, tenderness, or tastes pus in your mouth, dont ignore these signs. Make an appointment with your dentist as soon as possible. Your dentist may be able to identify a gum abscess based on your symptoms.
During this appointment, your dentist may examine your gums and look for signs of an infection. These include pain, swelling, and redness. Along with visual observation of your gums, your doctor may order a dental X-ray to check for periodontal disease or an infected tooth . An X-ray can also help your doctor assess whether you have bone loss from the infection.
Symptoms of a gum abscess may improve slightly in time. But even if an abscess ruptures and drains, you should still see a dentist to treat the infection.
Donât Miss: Ear Infection Clear Up On Its Own
Also Check: Dr On Demand Tooth Infection