Heres What Has Worked For Me In Avoiding Pump Site Infections From Escalating:
1.Keep your site clean! I know this one sounds obvious, but I sware the longer you have diabetes, the lazier some of us get. The common thread between both pump site infections was from bacteria getting under the site. On the first infection, Im almost positive I did not use an alcohol swab before applying the site. On the second one, I had slightly ripped off the top half of the site while working out, and instead of changing it, I pressed it back down in hopes of getting a few more hours/day out of it. Moral of the story: think STERILE CLEAN.
2.Know the difference between site irritation + infection. In my experience, pump site irritations from the adhesives can be red but tend to lean on the itchier side. An infection forming, on the other hand, feels more tender for me to touch and will gradually feel hard under the skin close to the needle center if an abscess is forming. If you start to feel any tenderness while pushing down on the site, take it off immediatelydont wait!!!
3.Circle the site. If you take off the site and notice its slightly more red than usual and want to keep an eye on it, circle the area with the pen. If over the next 12 hours you realize the redness is spreading beyond the circle, thats when you might want to take some action.
Let me know in the comments below if you found this blog post helpful and go-ahead and share it with someone who you think might benefit from reading it!
Access To Insulin Pumps
In Australia, insulin pump therapy is limited to people with type 1 diabetes who have private health insurance. There are some government subsidy programs and charitable organisations, such as the Juvenile Diabetes Research Foundation , that may assist with the cost of an insulin pump in special circumstances. Patients without private health insurance have to purchase the insulin pump themselves. The current commercial price of an insulin pump is approximately $10 000.
In 2017 a government subsidy for continuous glucose monitors was implemented for people under the age of 21 years. However, patients over 21 years receive no subsidy and must purchase continuous glucose monitors at the full price of approximately $300400 per month. Additional costs with pump use include consumables such as infusion sets and reservoirs, costing $2530 per month.
Whats So Great About The Pump
The list is an important one, in large part because pumps provide more precise and tailored insulin delivery. As a result, they offer greater lifestyle flexibility. Tailored insulin delivery can help:
- The dawn phenomenon by matching your early-morning increase in insulin resistance, so you avoid high blood sugar.
- Post-meal glucose rise from slowly digested foods or gastroparesis .
- Shift workers by adjusting the basal rates to your varying work schedule
- Frequent travelers by adjusting the basal and bolus rate to your travel schedule and time zone changes
- Prevent low blood sugars during physical activity and exercise by use of temporary basal insulin rate settings
- Extremely insulin sensitive people by delivering small doses of insulin
Read Also: How To Prevent Yeast Infection From Antibiotics
Anatomy Of The Insulin Pump
Generally, insulin pumps consist of a reservoir, a microcontroller with battery, flexible catheter tubing, and a subcutaneous needle. When the first insulin pumps were created in the 1970-80s, they were quite bulky . In contrast, most pumps today are a little smaller than a pager. The controller and reservoir are usually housed together. Patients often will wear the pump on a belt clip or place it in a pocket. A basic interface lets the patient adjust the rate of insulin or select a pre-set. The insulins used are rapid acting, and the reservoir typically holds 200-300 units of insulin. The catheter is similar to most IV tubing , and connects directly to the needle. Patients insert the needle into their abdominal wall, although the upper arm or thigh can be used. The needle infusion set can be attached via any number of adhesives, but tape can do in a pinch. The needle needs to be re-sited every 2-3 days.
Continuous Subcutaneous Insulin Infusion
Continuous subcutaneous insulin infusion can give a better quality of life .
There has been a systematic review of 11 studies of at least 10 weeks duration, comparing soluble insulin with the analogues lispro and, in one case, aspart in pumps . The analogue produced a small, significant improvement in HbA1c. There were no differences in hypoglycemia. Ketosis, hyperglycemia, and clogging were not common.
In 132 patients with type 2 diabetes using insulin randomly assigned to continuous subcutaneous insulin infusion or multiple daily injections of insulin aspart and NPH insulin) for 16 weeks, after 8 weeks training to establish optimal dosages there were more episodes of hyperglycemia with multiple daily injections. HbA1c was identical. Most of the patients who expressed a view wanted to stay on the pump.
In 40 patients aged 425 years with type 1 diabetes who were given continuous subcutaneous insulin infusion for 6 months the number of episodes of hypoglycemia was reduced by a half . There were two episodes of diabetic ketoacidosis. In 10 patients lipohypertrophy developed at the insertion site and three patients had signs of skin redness, which improved with local antibiotic treatment.
Nancy A. Allen, Michelle L. Litchman, in, 2020
Read Also: Over The Counter Medicine For A Tooth Infection
Complications From Insulin Pump Use
The most common complications of insulin pump therapy involve the skin and soft tissue.
Travelling With An Insulin Pump
While travelling, an accompanying letter on practice letterhead should be provided stating the medical history of the patient, including the diagnosis of type 1 diabetes, and that management is via an insulin pump. A list of current drugs, with generic names and doses, should be included. The letter should stress that it is important that the patients drugs accompany them, and that the insulin pump should not be disconnected. In particular, the pump should not be put through airport X-ray machines.
Prescriptions should be obtained for insulin and other drugs before travel. In case of pump failure both rapid-acting and long-acting insulin should be obtained along with injecting devices and needles. Sufficient equipment for glucose testing should be packed in the hand luggage. In addition to drugs and glucose-testing equipment adequate quantities of consumables should be packed. As a rule, pack twice as many sets as potentially required for the planned period away from home. An adequate supply of consumables should be included in the hand luggage while flying.
You May Like: What Can Treat Urinary Tract Infection
Lumps And Bumps From Insulin Therapy
One of the most popular blogs of all time here at The LOOP is on lumps and bumps related to insulin infusion, so we wanted to bring it back to you along with some new tips.
Q. What are these lumps and bumps at my injection sites?
A. Lipohypertrophy is a medical word for a lump under the skin from a buildup of fat at the site of insulin injection or infusion. This comes in the form of lumps or bumps under the skin. Scar tissue, or hardened areas, may also develop at the sites.
This can happen to anyone who takes insulin, whether its delivered through a syringe or insulin pump. It happens due to the action of insulin on the fat cells because insulin can cause fat cells to increase in size. Its generally seen when someone uses the same favorite spots over and over again, and usually happens in areas easiest to reach
Q. What happens with these lumps and bumps?
A. Delivering insulin into affected areas can affect your glucose control. Since insulin is not always well-absorbed in these areas, you may find that your glucose control is not what you expect it to be. The more damaged the area is, the more likely it is that glucose control will be affected.1 Sometimes these areas have damaged nerve endings and you dont feel a needle going in at all. This is a sign that you should stay away from that spot.
Q. If I need to take insulin, how can this be prevented?
Heres a guide of some potential areas to give your insulin:
How Do You Manage Patients Using Subcutaneous Insulin Pumps
Insulin pumps are now commonly used and can ensure good glucose control. The pumps use one of the newer analog insulins and deliver both basal and bolus insulin doses. Since the basal rate is set to deliver necessary insulin for the fasting state, the pump can be used for insulin delivery during the perioperative and intraoperative periods, continuing the established basal rates. Check blood sugars at regular intervals, every 1 to 2 hours, to ensure that the patient’s blood sugar stays between 80 and 180 mg/dl. If the stress of a long surgery raises glucose levels, the basal infusion rate can be safely raised in increments of 0.1 unit per hour. If glucose levels fall, the rate can be safely reduced in increments of 0.1 unit per hour, or the pump can be suspended until glucose levels rise. When the patient is fully recovered, return to normal routines for pump use. The patients may consume a regular diet, as appropriate, when fully alert, awake, and with good bowel sounds.
Elizabeth A. Stephens, Terri Ryan, in, 2009
Don’t Miss: Can A Dentist Work On An Infected Tooth
Patients And Implantation Procedures
A total of 57 patients with T1DM were treated with CIPII. One patient with self-induced complications was excluded from analysis the remaining 56 patients are subject of this study. Patient characteristics are depicted in Table Table1.1. Two hundred eighty three patient years of follow up were observed, with a median duration of 4.7 years. In total, 80 pumps were implanted 20 patients had a second pump and 4 patients had a third pump implanted.
Infection From An Insulin Pump
Here is a blog from a Facebook friend involving an infection from an insulin pump. Most unusual, and a frightening experience for her. She has a blogsite called thediabeticjourney.com. Here is her blog:
The actual pump has not caused an infection the canula has though and thats down to basic hygiene surely?
Surely. That is why I try to schedule site changes to happen right after my shower. I never use arms because they are more exposed than the belly and the midriff. Butt would probably be good, too, if I could reach it. My understanding is that all insets are sealed into a sterile impervious environment. The only source for contamination would be the skin. Staph is commonly present on the skin and usually does not cause any problems unless it somehow sneaks into the body.
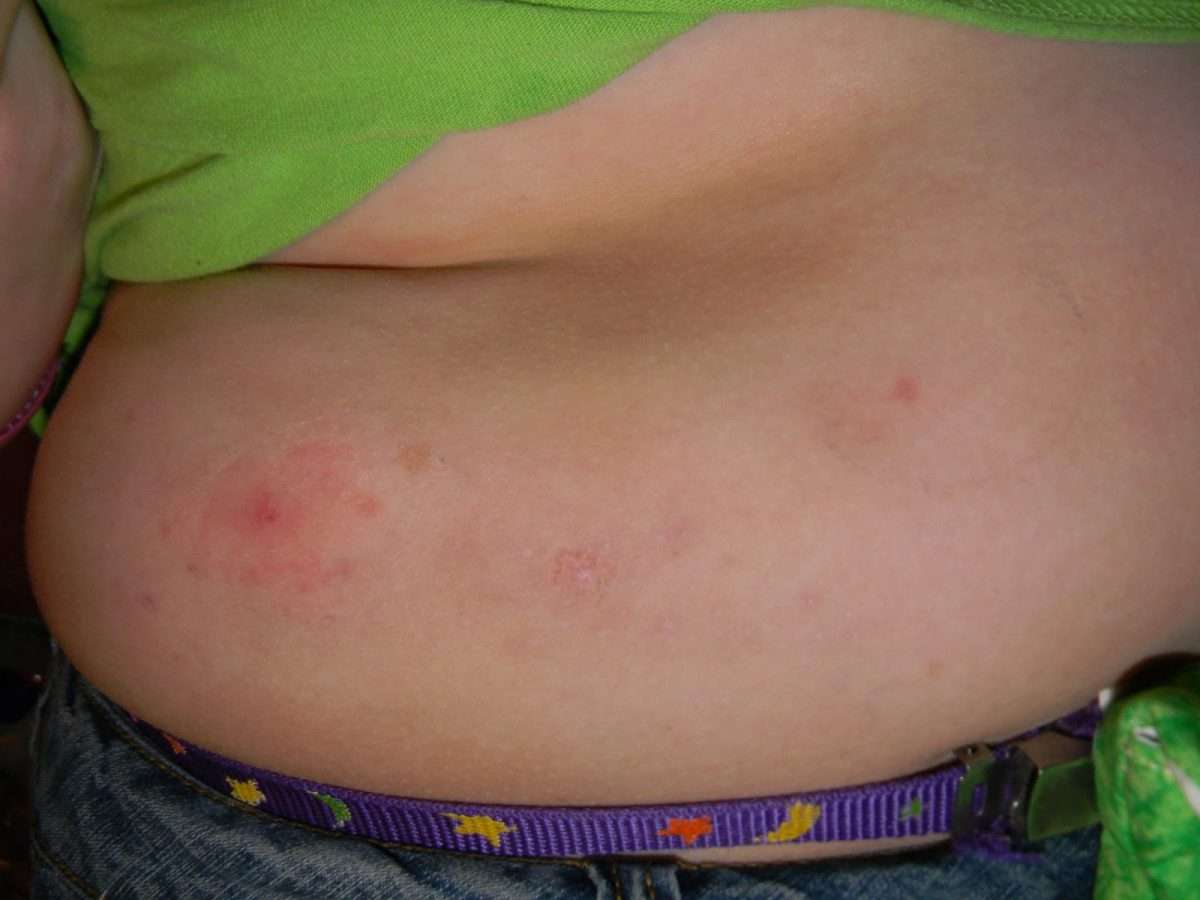
I once had an infection at an infusion site. I was vacationing in Costa Rica and it was the last infusion site I had inserted the day before I traveled home. The site was sore on my trip home but I let it ride and changed the site when I got home. A few days later it turned red and swollen. A large raised section of flesh formed the shape of an egg. My diabetes doctor referred me to a surgeon who lanced it and drained the puss. It took a week or more to heal. My blood glucose was elevated and resistant to correction.
Preventing and Treating Insulin Pump Site InfectionsBy Jacqueline Marshall, Nov 11, 2014
Recommended Reading: The Best Antibiotic For A Tooth Infection
Suitability For Pump Therapy
Careful consideration is essential to determine which patients are suitable for insulin pump therapy. Patients need to be willing and able to self-manage the technology which requires programming by the user. The patient also needs adequate carbohydrate counting skills, and to be competent at blood glucose self-monitoring. They must be motivated to accept responsibility for their own care.
Insulin pumps are typically recommended for patients with suboptimal glycaemic control despite multiple daily injections. In particular, those with frequent or unpredictable hypoglycaemia associated with hypoglycaemia unawareness may benefit. Women planning pregnancy often transition to pump therapy before conception to achieve tighter glycaemic targets pre-pregnancy and to maintain control during pregnancy. Insulin pumps may also provide greater flexibility for people who do shift work, frequent travel, intensive exercise and physical activity.
Complications Of Insulin Pump Therapy: The Effect Of Insulin Preparation
Diabetes Care
Robert S Mecklenburg, Terin S Guinn Complications of Insulin Pump Therapy: The Effect of Insulin Preparation. Diabetes Care 1 July 1985 8 : 367370.
Complications of insulin infusion pump therapy include ketoacidosis related to interruption of insulin delivery and infected infusion sites. To determine if the type of insulin used in insulin pumps is a factor influencing these complications, we compared the occurrence of inflammation and infection at infusion sites and obstruction of infusion tubing in a 6-mo crossover study of 28 patients using two different insulin preparations. The use of buffered purified pork insulin was associated with less infusion site inflammation and infusion set obstruction than use of unbuffered beef-pork insulin. Infected infusion sites occurred less often with buffered pure pork insulin than with unbuffered beef-pork insulin, but the difference was not statistically significant. We conclude that the type of insulin selected for use in insulin pumps influences the occurrence of adverse reactions to insulin pump therapy: buffered purified pork insulin is associated with less infusion site inflammation and infusion set obstruction than unbuffered beef-pork insulin.
Read Also: Will Nasacort Help Sinus Infection
Site Infection And Antibiotics
After 33 years doing MDI, I finally got a pump a few weeks ago. So far I love it, but I managed to get an infusion site infection on only my 5th pod or so It was quite red, raised and puffy and about 2 across so I went to the doctor who gave me a round of clindamycin. Anyone else been given oral antibiotics for a site infection and have it be effective? How long did it take to kick in? Ive been on them for a day and a half and not seeing any noticeable improvement yet, and the red area has continued to grow . Trying to get an idea of how long it might take to see it improving, and when I should go see my own doctor if Im not seeing it get better.
In over 30 years of pumping, Ive only had one infusion site infection. It was red and inflamed in an egg-shaped raised mound. My doctor referred me to a vascular surgeon. The surgeon lanced it and I did take some follow-up antibiotics. It resolved nicely.
On a side note, and this may not contain anything meaningful for you, I took clindamycin for a dental infection and was left with a difficult to shake c-dificile infection. I was told by a pharmacist at the time that clindamycin was notorious for this.
Thanks for the reply Terry!
Im on clindamycin since I have an allergy to most penicillins – I have taken it before without issue so hopefully this time will be ok too. Does not sound fun about the c dificile!
Managing Insulin Pumps In General Practice
The management of a patient on an insulin pump requires the involvement of a specialist diabetes team including an endocrinologist, diabetes nurse educator and dietitian. The GP is an essential member of this team and it is therefore important GPs understand the terminology related to insulin pump therapy .3
Read Also: How To Cure A Bacterial Sinus Infection
How Much Does An Insulin Pump Cost
If you pay for a pump yourself, they cost around £2000 to £3000 and should last between 4 to 8 years. This is a lot of money, and is a big commitment.
Extra costs
You’ll also have to buy other things that make the pump work, like your cannulas and tubing, batteries, dressings for the skin, adhesives and alcohol wipes for skin preparation if you prefer it to soap and water. This could cost around £1500 or more extra a year. You don’t have to pay for your prescription insulin which you get free.
Whats Not So Great About The Pump
There are downsides to any therapy, and the insulin pump is no exception.
- Wearing it can be unsettlingMost of the time, youll be wearing your pump on your body, clipped to your waistband or in your pocket. Fortunately, many accessories are available to make wearing the pump discreet and convenient.
- CostInsulin pumps cost thousands of dollars. Insurance coverage for insulin pumps varies. Some companies will cover all of the cost, while others may cover only half. Some might also pay for only certain brands. Dont forget to factor in the cost of disposable items, such as cartridge syringes, infusion sets and skin preparation items.
- Higher risk for ketoacidosisThere is a greater risk for ketoacidosis in pump therapy, because long-acting insulin is not used. Because of this, high levels of ketones may develop when there is not enough insulin in the bloodstream. This can happen if there is air in the tubing, a bad infusion set, insertion site infection, or if the insulin pump is disconnected for too long. See also Ketones and pump therapy. As a result, ketoacid levels rise, which can lead to diabetic coma.
- Risk of infusion site infectionInfections can occur if an infusion set is left in for too long. To lessen your chance of infection, change the set as directed by your doctor or pump educator. It is also crucial to wash your hands and the site properly in order to reduce chances of infection. See also Infusion set tips.
You May Like: Best Treatment For A Urinary Tract Infection