Why Does Birth Control Cause Yeast Infections
To prevent you from getting pregnant, hormonal contraceptives alter your naturally occurring hormones. This is a powerful disruption to your bodys chemistry and can cause several significant side effects, among them, an imbalance of bacteria and yeast, which causes infections.
If you take hormonal contraceptives high in estrogen and/or progesterone, you could be prone to experiencing vaginal yeast infections. Lower-dose hormonal contraceptives pose less risk for developing infections. If you suspect your birth control is the cause of your yeast infection, do not stop using it without consulting your healthcare provider first.
Fluconazole And Birth Control
Theres little evidence that Fluconazole, the generic form of Diflucan and a common medication used to treat yeast infections, will affect birth control. Its worth discussing any safety concerns or questions with your primary care provider before taking any new medication. Whenever starting a new medication, the more details about your medical history you provide, the better. Discuss topics including any allergies you have, possible interactions with any vitamins, supplements, or other medications you take, and if pre-existing conditions increase your risk of experiencing side effects. Some conditions are contraindicated when considering Diflucan are:
- Low amounts of either potassium or magnesium in the blood
- Torsades de pointes
You Have A Blood Sugar Imbalance
Insulin resistance caused by prediabetes, diabetes or polycystic ovary syndrome is another common trigger for recurring yeast infections, Dr. Gersh says. Blood sugar imbalances can cause excess sugar to accumulate in the urine, which can affect the vaginal environment and set the stage for yeast growth.
âFix it: âTalk with your primary care provider if your blood sugar isn’t well controlled. Together, you can determine whether lifestyle changes like diet and exercise can address the problem or whether you need to take medication to get your blood sugar back into balance, per the Centers for Disease Control and Prevention .
Don’t Miss: How To Fix A Tooth Infection At Home
Birth Control That Doesnt Cause Yeast Infection
Non-hormonal birth control options are less likely to increase your chances of experiencing a yeast infection. Barrier methods like diaphragms, cervical caps, condoms , and IUDs are all types of non-hormonal birth control.Options also include sterilization , pulling out, and menstrual cycle tracking. Each type of birth control has pros and cons. We suggest speaking with your primary care provider about which method are best in your situation. Although most birth control methods have a low risk of leading to a yeast infection, it might be worth discussing alternative birth control methods with your primary care provider if youre experiencing any problems or to specifically discuss changes of developing a yeast infection on birth control.
Can The Pill Make You Itchy

Evidence for higher rates of thrush in women taking the pill is contradictory. Some research suggests switching to the contraceptive injection such as Depo-Provera, which only contains the hormone progestogen and may help those with recurrent yeast infections and vulvar itching. However it is not yet clear whether other progestogen-only methods will offer the same benefits.
A quarter of The Lowdown reviewers for the combined contraceptive pill noted thrush and an itchy vag as a side effect. Similarly, 23% of those on the progestogen-only pill experienced thrush whilst using the contraceptive.
You May Like: Sphenoid Sinus Infection Neck Pain
You Have A Weakened Immune System
Medical conditions such as HIV or using certain medications can weaken the immune system, making it harder for the body to fight off infections, including yeast infections, per UpToDate.com.
âFix it: âTalk with your doctor if you’re experiencing recurrent yeast infections alongside a condition or medication that’s suppressing your immune system. Together you can decide on the best steps to reduce your infection risk and discuss whether it’s possible to change medications.
Your Birth Control Isn’t A Good Fit
Hormonal fluctuations caused by birth control options like the pill can create a vaginal environment that’s more prone to yeast infections, according to the Cleveland Clinic.
This isn’t always the case, as different studies have shown different results when it comes to hormonal birth control and the immune response, according to a February 2022 paper in âCancersâ. It seems to depend on the individual, the hormonal dose and the method of delivery , and how they all react together.
âFix it: âRecurring yeast infections may be a sign that your birth control isn’t a good fit.
Talk with your gynecologist about trying a contraceptive with a different hormonal dose or method of delivery. Research in the November 2012 issue of âContraception âsuggests that the vaginal ring may be a better fit.
Don’t Miss: How Soon After Hiv Infection Can You Infect Others
The Connection Between Yeast Infections And Birth Control Use
Perhaps the most significant risk factor for yeast infections, since it affects the largest category of women at any given time, is birth control use.
Birth control, including condoms, spermicidal jellies and creams, intrauterine devices , sponges and diaphragms, and oral contraceptives can increase vaginal yeast infection risk in several ways , .
Blood Clots: Uncommon But Serious
Blood clots are a rare but potentially serious side effect of oral contraceptives. Each year, a small number of women who take oral contraceptives develop blood clots, notes the American Congress of Obstetricians and Gynecologists . Women who smoke, are overweight, are over 35, or have recently given birth are considered at higher risk.
Blood clot signs to watch for:
- Breathing problems or chest pain could signal a clot in the heart or lungs.
- Pain, warmth, and swelling in the leg could indicate clotting in the lower leg, called deep vein thrombosis.
If you experience symptoms of a possible blood clot, seek immediate medical attention, says Kyoko Peña-Robles, MD, MPH, who specializes in obstetrics and gynecology with One Medical Group in San Francisco.
Also Check: Uti Symptoms Vs Kidney Infection
I Exercise A Lot Which Means Yeast Infections Can Be Part Of Life
Im super active, and while being active can lead to many positive results, it can sometimes lead to a few not-so-good results. Like vaginal yeast infections. Yeast thrives in warm, moist environments in the vaginal area. Sweat from physical activity, wet swimsuits after swimming laps, and tight spandex or nylon underwear can contribute to warm, moist environments that help yeast to thrive. If youre active like me, and you get yeast infections, the good news is, theres something you can do about it.
When To See A Healthcare Professional
If you have used the OTC medication and the infection has not cleared up within a week, you might need to contact a health provider to get a prescription for oral medication or a prescription-strength antifungal cream. Also contact your provider if you:
- Continue to have abdominal pain.
- Notice a strong and unpleasant odor with your vaginal discharge.
Read Also: Will Tooth Infection Go Away On Its Own
Implementation Of The Study
The study was conducted in the oral diagnosis department of the dental infirmary of Islamic Azad University in the city of Isfahan. Verbal consent was obtained from patients before taking samples. In order to assess the oral health status of patients, their plaque indexes were recorded. Patients with similar plaque indexes were selected by the clinician who conducted the examination in order to ensure greater consistency in the studys collected data. The questionnaire was completed to gather information such as age, type of OCP used, days of consumption and duration of therapy, previous history of fungal infection, systemic disease, smoking habits, and recent use of antibiotics or corticosteroid medication. Next, a thorough examination of the oral cavity for the presence of red and white candidiasis lesions was performed. The patient was questioned for symptoms such as a burning sensation or an unpleasant taste.
The survey results are based on the color of the microorganism colonies. C. albicans turns green, C. tropicalis turns metallic blue, C. krusei turns pink velvet, and other species are detected in white to purple colors. The colonies were counted and examined by microbiology specialist.
What About The Vaginal Ring
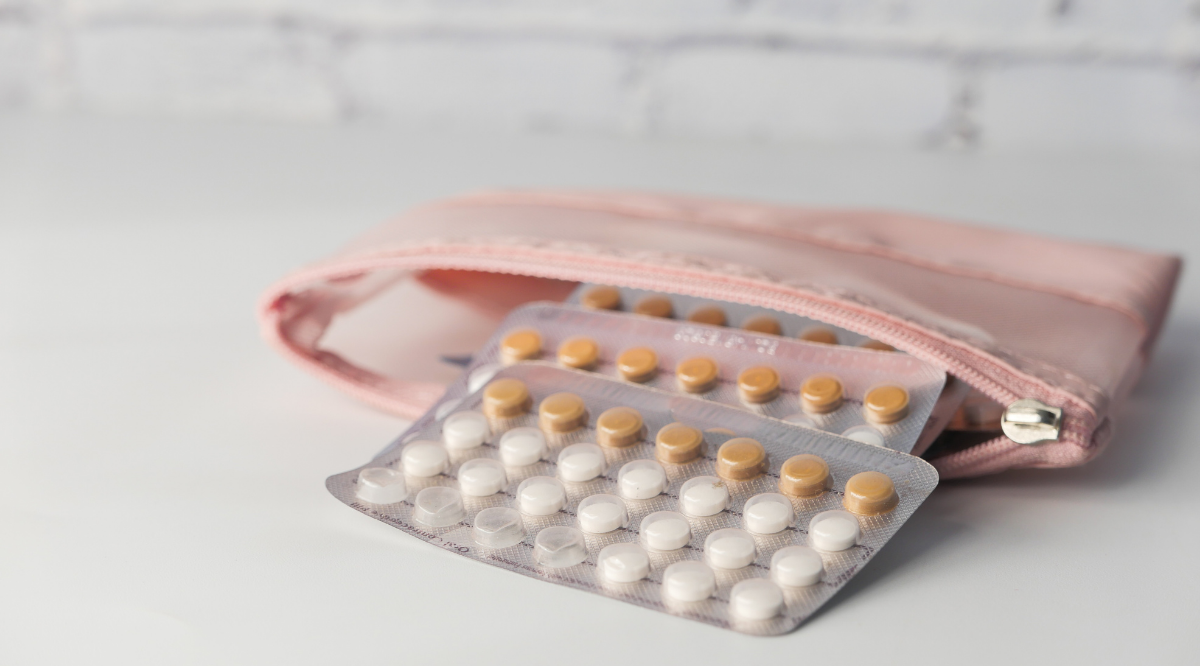
In a similar result to the study on coils, yeasts were found adhered to the surface of vaginal rings in a study on the vaginal health of users. However, cases of thrush were not found to be higher in those using the contraceptive vaginal ring when compared to those using equivalent oral contraceptives.
As for The Lowdown users, 26% experienced thrush whilst using the vaginal ring: the highest percentage for a method of contraception reviewed by our audience, but not by any great margin when compared to the mini pill , combined pill , or hormonal IUS .
Recommended Reading: What Do Doctors Prescribe For Yeast Infections
How Are Vaginal Yeast Infections Diagnosed
In most cases, you can treat this complaint in the privacy of your own home and will soon know if you are suffering from a yeast infection of not by the improvement, or lack of, you are likely to experience. To firmly establish the diagnosis and to rule out any other underlying causes of the symptoms, your doctor will take a specimen, a smear test, scraped from the affected area for microscopic analysis or for culture in a laboratory. Identification of yeast under a microscope, when possible, is the least expensive and most rapid and accurate way to establish the diagnosis and in chronic cases I always recommend identification.
Early detection is important because you may have another condition that may present just like a yeast infection for example such as gardnerella, which is a bacterial infection and not a yeast infection.
Birth Control Pills And Yeast Infections
Would you be surprised if I told you there is a direct connection between birth control pills and yeast infections?Unfortunately this is the truth. If youre a chronic yeast infection sufferer on the pill this article will more than likely shed a tremendous amount of light on the root cause of whats causing youre frequent yeast infections.
There are lots of amazing natural treatments you can use when you first experience a yeast infection, make sure to not limit yourself to drug based treatments such as Monistat as they have their own issues.
Click Here to Discover how I cured my Vaginal Yeast Infection in less than 12 hours without the use of harmful drugs , antibiotics or expensive supplements!
======================================================
Read Also: Natural Antibiotics For Dental Infection
How Does Hormonal Birth Control Increase Your Risk
Many birth control pills, the patch, and the vaginal ring all contain a combination of estrogen and progestin. Progestin is a synthetic version of progesterone.
These methods disrupt your bodys natural balance of estrogen and progesterone. This can lead to yeast overgrowth.
Overgrowth occurs when Candida, a common form of yeast, attaches itself to estrogen. This prevents your body from using the estrogen and eventually drives your estrogen levels down. During this time your progesterone levels may increase.
This is the perfect condition for Candida and bacteria to flourish, which can lead to a yeast infection.
The type of birth control you use typically isnt enough to prompt a yeast infection. Several other factors may be involved.
Certain habits may increase your risk:
- eating excessive amounts of sugar
- not changing tampons or pads often enough
- wearing tight, synthetic, or wet garments
- using irritating bath products, laundry detergent, lubes, or spermicides
- using a contraceptive sponge
Common Side Effects Of Nuvaring
Here are some common side effects reported from women who have used the birth control method NuvaRing:
- Nausea and vomiting
Less common side effects include:
- High blood sugar, especially in women who have diabetes
- High fat levels in blood
- Blotchy darkening of the skin
- Vaginal yeast infection
- Fluid retention
Recommended Reading: Medicine For Bacterial Sinus Infection
Yasmin And Yeast Infection
Birth control pills, like Yasmin, can increase your risk of yeast infection because they alter the hormones in your body. There are two main pill forms of birth control: combination pills and minipills. Combination pills have estrogen and progestin, whereas minipills only have progestin. Its considered relatively low risk to use a birth control pill unless you have preexisting conditions that increase your risk of yeast infection or other health problems. If you think your birth control is causing a problem, speak to your primary care provider about other birth control options.
Can Contraceptives Help With Vaginal Dryness
With the rise in popularity of fertility awareness methods , you may already know that changes exist in both consistency and volume of normal discharge throughout your menstrual cycle.
Due to variations in hormone levels, cervical mucus can take different forms depending on the day of your cycle. Oestrogen levels are particularly high around ovulation, and you may notice an increase in discharge at this time.
The combined contraceptive pill contains both progestogen and oestrogen, and this increased level of oestrogen in those taking the combined pill may translate to an increase in discharge. Although as we mentioned earlier users may also experience vaginal dryness!
The Lowdown users have reported discharge as a side effect of hormonal contraceptives, with a whopping 56% of those taking the combined pill experiencing this change.
Recommended Reading: Pentrexyl 500mg For Tooth Infection
What Increases My Risk Of Getting A Yeast Infection
Certain factors make you more likely to get a vaginal yeast infection.
Certain factors can increase your risk of getting a vaginal yeast infection. Some of those are:
Certain lifestyle risk factors also increase your risk of a vaginal yeast infection, such as:
- Sitting in a wet bathing suit.
- Not changing out of sweaty clothes.
- Wearing scented tampons or using a vaginal deodorant.
You’re Taking Antibiotics Too Often
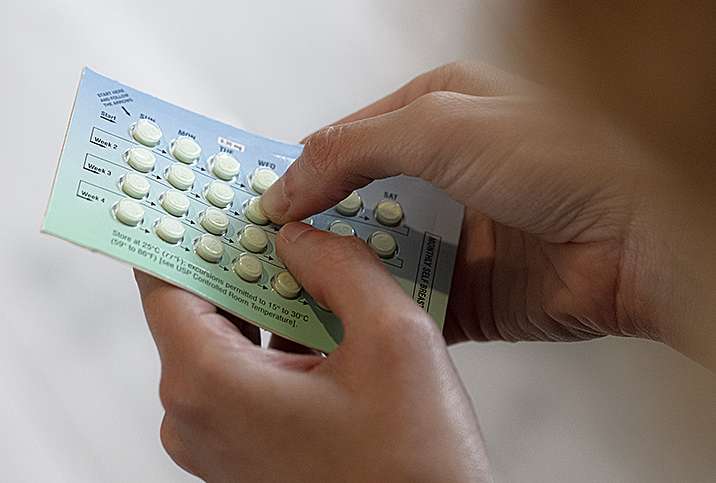
That can set the stage for yeast like candida to grow out of control and cause an infection, especially if someone is taking antibiotics frequently, says Felice Gersh, MD, ob-gyn and founder and director of the Integrative Medical Group of Irvine in Irvine, California.
âFix it: âIf you’re taking antibiotics regularly or often, reducing your use can help bring your vaginal bacteria back into balance, making it harder for yeast infections to develop.
Talk with your doctor before making any changes to your antibiotic regimen.
Don’t Miss: Fastest Way To Cure A Bladder Infection
Keep Getting Yeast Infections Here’s What Your Body’s Trying To Tell You
The majority of people with vaginas will get a yeast infection at least once, or maybe even twice, in their lifetime. But is it normal for them to practically be a regular thing?
Video of the Day
Vaginal yeast infections are caused by an overgrowth of the fungus candida albicans. They’re typically marked by intense vaginal itching or irritation, redness or swelling, burning while urinating and vaginal discharge that can be watery or white and cottage cheese-like, according to the Mayo Clinic.
Yeast infections are considered recurring if a person has four or more of them per year. When that happens, they’re typically triggered by an underlying cause that needs to be addressed.
Here are the most common culprits behind recurrent yeast infections and what you can do to find relief.
Treatment For Yeast Infections
Mild yeast infections often clear up on their own within a few days, and over-the-counter antifungal ointments, creams and suppositories can clear up lingering infections within a week or less. If symptoms do not clear with OTC treatment, then a doctor’s visit may be needed.
If you experience frequent yeast infections , then you are strongly encouraged to consult a medical professional. Chronic yeast infections can be a sign of a more serious condition or autoimmune diseases, such as diabetes or HIV/AIDS.
Recommended Reading: What Is A Natural Antibiotic For Sinus Infection
What Are The Symptoms Of A Vaginal Yeast Infection
There are several tell-tale signs of a vaginal yeast infection. These symptoms can include:
- A thick, white vaginal discharge with the consistency of cottage cheese.
- Small cuts or tiny cracks in the skin of your vulva because of fragile skin in the area.
- A burning feeling when you pee.
In some cases, another symptom of a vaginal yeast infection can be pain during sex.
Symptoms of a yeast infection are similar to the symptoms people feel when they have a sexually transmitted infection or other vaginal infection. Contact your healthcare provider if you have any of these symptoms so they can examine you.
Does My Sexual Partner Need To Be Treated If I Have A Vaginal Yeast Infection
A note from Cleveland Clinic
Yeast infections are a very common fungal infection that most women or people assigned female at birth will have in their lifetime. Its highly treatable with medication, some of which are available to purchase at your local drug store without a prescription. Even though you may know the signs of a vaginal yeast infection, its important to get examined by your healthcare provider. They can recommend the best treatment based on the type of yeast infection you have and its severity.
Last reviewed by a Cleveland Clinic medical professional on 09/02/2022.
References
Don’t Miss: What To Do If You Have A Bad Tooth Infection
Vaginal Yeast Infections More Common When Using Contraceptives Or Spermicides Or Participating In Receptive Oral Sex
- Share on:
ANN ARBORTwo out of three women experience the itching, burning, soreness and discharge of vulvo-vaginal Candidiasis, or vaginal yeast infection, at least once in their lives, but surprisingly little is known about what women can do to prevent themselves from getting this common condition.
A University of Michigan School of Public Health study of 691 women is the first population-based study specifically designed to identify risk factors for yeast infections. The researchers also tested whether commonly suspected factors increase the risk and found that some were not significant after all. The researchers gathered data through clinic records and a survey.
The researchersBetsy Foxman, associate professor of epidemiology at U-M, and Ann M. Geiger, now a researcher at Kaiser Permanente, Southern Californiapublished their study in the March issue of Epidemiology.
The risk factors included:
Receptive oral sex. Participation in oral sex tripled the risk, said Geiger. Oral sex may provide a route for transmission of yeast, as one-third to one-half of adults carry yeast in their oral cavity. Saliva could also cause irritation, facilitating Candida adherence and growth.
Oral contraceptive and spermicide use within the last two weeks. Risk for a yeast infection was doubled by use of oral contraceptives and tripled by spermicides, said Foxman.
412 Maynard St.