How Soon Will It Start Working
Once you start taking clindamycin, youll likely notice an improvement in your symptoms after a day or two. If your symptoms arent improving at all or seem to be getting worse after taking clindamycin for a few days, follow up with your healthcare provider.
important
Make sure you take the full course of antibiotics as prescribed by your doctor, even if you start to feel better before finishing them. Otherwise, you may not kill all of the bacteria, which can lead to recurring infections and antibiotic resistance.
Allergic reactions to clindamycin are rare. If you develop any kind of rash while taking clindamycin, contact your healthcare provider this may be a sign of a drug allergy.
In rare cases, its possible to have a potentially life-threatening reaction called anaphylaxis.
Symptoms typically appear within 30 minutes of taking a drug and can include:
- itchy hives and welts
- swollen throat, which can cause wheezing and trouble with breathing or swallowing
- chest tightness
- feelings of doom
While the risk of having an anaphylactic reaction to clindamycin is low, its important to know how to recognize the signs. Anaphylaxis is a medical emergency that requires immediate treatment.
Taking clindamycin can cause a range of side effects, including:
- nausea or vomiting
- loss of appetite
Symptoms of C. diff to watch for include:
- watery diarrhea up to 15 times per day that may contain blood or pus
- severe abdominal pain
How Long Does It Take For Antibiotics To Work
An antibiotic is a medication used to kill or decrease the growthof bacteria. The lifesaving medications come in various forms and can be used totreat infections caused by bacteria. Antibioticscan treat the infection by attacking the wall surrounding the bacteria, interferingwith its reproduction, or by blocking the protein production of it.
Although you might not notice it right away, antibiotics beginworking as soon as you start taking them. Usually, within 2-3 days, youllstart feeling better and see an improvement in the infection. On average, afull course of antibiotics takes 7 to 14 days to complete depending on the typeused.
Most often, infections are resolved when antibiotics are usedcorrectly, but there are some instances when they wont work, like whentreating an infected tooth. Instead, youll need a root canal to prevent yourtooth from needing to be extracted.
Herbal Tea Or Fenugreek
Herbal teas or medicinal grade teas contain high concentrations of these herbs and enhance their anti-inflammatory and healing properties. Additionally, there is the Fenugreek tea commonly known to alleviate symptoms of dental infection. Another tea is the so-called goldenseal associated with turmeric and has anti-inflammatory, antibacterial, and antibiotic properties that could be managed in a dental infection.
Also Check: Chicago Fire Infection Part 2
What To Do If Antibiotics Dont Fix Your Dental Abscess
If oral antibiotics do not fix your abscess, . In some cases, youll make an appointment to visit your dentist in the coming days.
For others, youll need to visit an emergency dentist for treatment of the infected tooth. This is when IV antibiotics or extraction are needed.
This is also the case when you first notice the abscess. An abscess might not seem severe, but it is a serious medical condition. You can ease the pain with over-the-counter pain relief, but you must see a dentist for immediate attention.
The infection causing the abscess can spread and is potentially fatal if not treated. This is true whether you are just experiencing the first symptoms of an abscess or if youve been taking antibiotics that have not worked.
In addition to seeking emergency dental treatment, youll want to:
- Avoid hot and cold beverages
- Avoid high-sugar and high acidity foods and beverages
- Take an over-the-counter pain reliever that is safe for you
- Floss between the affected teeth to prevent food particles from further aggravating the problem
- Sleep with your head elevated
- Rinse with warm salt water two to three times a day
A visit to an emergency dentist is necessary if you have an abscess and cannot see your regular dentist. An abscess can be fatal if left untreated. It is a dental emergency, even if you think you can deal with the pain.
Alternative Treatment Options
Alternative treatments and home remedies for abscesses include:
Take Over-The-Counter Pain Relievers
When To Seek Emergency Treatment For Dental Abscesses
Ideally, a person affected by a dental abscess, or who suspects that they may have a dental abscess, should visit the dentist as soon as possible. Because it is not always possible to see a dentist in time, some people may need to be treated for their abscesses in a hospital emergency department. Medical doctors are not specifically trained to handle dental issues, but will be able to stabilize the affected person, providing antibiotics and pain relief, until they can see the dentist.
Good to know: Dentists do not form part of the regular staff in most hospital emergency departments. Treatment by a doctor at a hospital will not replace seeing a dentist. Doctors are not trained to deal with dental problems but will be able to assist with managing infection and pain.
If a person with an abscess or a suspected abscess shows any of the signs listed below, they should seek urgent medical care as soon as possible. Danger signs for tooth abscesses include:
- An abscess of more than 1cm in diameter, or which feels large
- Severe swelling or hard lumps on the gums or the face
- Bleeding on the gums or in the mouth
- Fever or a body temperature of more than 38 C / 101.4 F
- Tender lymph nodes in the neck area
If a person shows the symptoms listed below, they should immediately be seen by a hospital emergency department:
Dont Miss: Can Hiv Cause Ear Infection
Don’t Miss: Antibiotic Shot For Ear Infection
Can You Treat A Tooth Infection Without Antibiotics
There are ways to relieve the pain and swelling associated with your infected tooth. Saltwater rinses with or without baking soda, hydrogen peroxide rinses, and cold compresses can all help with these symptoms. See a dentist right away if you have any symptoms, because an infection is unlikely to go away without treatment.
A cavity can be filled, and pulpitis can also be treated with a dental procedure. You may not need antibiotics. But depending on how bad the infection is, you might need a root canal or removal of the tooth.
If you have an abscess, it needs to be drained. Your dentist will probably also prescribe antibiotics to get rid of any bacteria that are still in the area.
How Long Do I Need To Take Antibiotics For
No matter which kind of antibiotic suits you and your tooth infection best, its crucial to complete the full round of treatment.Sometimes, your symptoms may improve after a day or two. However, if the dentist or pharmacist recommends that you take it for an entire week, dont stop.
Taking antibiotics even though your symptoms disappeared can help ensure that the infection is truly healed and wont return.
The only reason you should stop taking a form of prescribed antibiotics is if youre having an allergic reaction to them. Even then, you should consult your dentist before you make a switch.
Recommended Reading: Best Antibiotic For Sinus Infection Not Amoxicillin
How Are Most Utis Diagnosed
There are several ways that your physician can diagnose a UTI. To provide the best antibiotic treatment for UTI, he or she needs to determine the location of the infection and whether your UTI is complicated. He or she also needs to rule out other conditions that present similarly to UTI, such as vaginitis or certain sexually transmitted diseases.
Most UTIs are diagnosed via urine test. In some instances, your healthcare provider may also order blood cultures and a complete blood count. These test results will confirm the type of bacteria, virus or fungus thats causing the infection.
Bacteria is to blame for the vast majority of UTIs, and theyre treated using a wide range of antibiotics. In rarer cases, where a virus is behind the infection, antivirals such as cidofovir are prescribed. Fungal UTIs are treated with antifungals.
How To Get Antibiotics For A Tooth Infection
You can get antibiotics for a tooth infection from your dentist or doctor, although dentists are preferable due to their experience with tooth infections. Antibiotics are not available over the counter you must have a doctor’s prescription.
Depending on your condition, you may be able to get prescriptions through an online dental consultation.
If you have antibiotics leftover in your medicine cabinet from an old infection, you should not use them. To properly dispose of your antibiotics, take them to your nearest pharmacy.
Don’t Miss: Can Sinus Infection Heal On Its Own
When To Prescribe Antibiotics In Dentistry
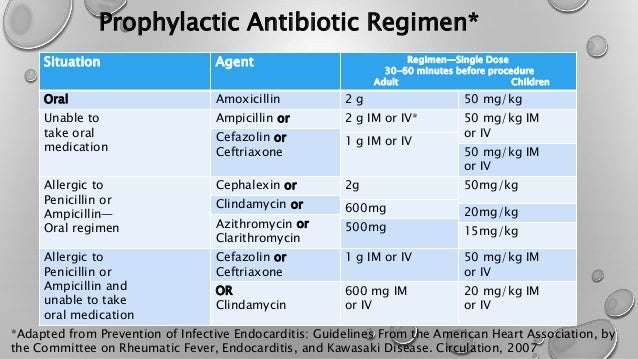
Dentists prescribe antibiotics also for precautionary purposes, as pre or post-operative prophylaxis. A particular case of antibiotic prophylaxis in dentistry concerns cardiac patients, those with congenital heart defects and those with an artificial valve. In these cases, the dentist prescribes antibiotic therapy to prevent bacterial endocarditis which can occur following a simple tartar ablation.
The selection of the antibiotic mainly depends on the type of bacterium that caused the infection. It also depends on infection severity, on the presence of pathologies or allergies and any pregnancy.
What Happens If A Tooth Infection Spreads To The Jaw
A tooth infection will not go away if it does not receive the right treatment.
You may feel less pain once the abscesses rupture, but dental treatment is still necessary.
If the abscess is not drained by a dentist, the infection can spread throughout the mouth and into your jaw. Infection that affects the jaw can harm the soft tissue surrounding this area.
The following are the potential health concerns that could happen when you leave a dental abscess unattended:
Also Check: Can A Tooth Be Pulled When Infected
Dental Abscess Treatment Options
Most dental abscesses will be treated immediately after diagnosis. An uncomplicated abscess will usually only require drainage to provide relief from the pain. Complicated abscesses may require more complex procedures and medications to control the underlying infection. If the infection spreads to the sinuses or neck, a surgeon may need to treat the condition.
The Global Antimicrobial Resistance And Use Surveillance System

WHO launched the Global Antimicrobial Resistance and Use Surveillance System in 2015 to continue filling knowledge gaps and to inform strategies at all levels. GLASS has been conceived to progressively incorporate data from surveillance of AMR in humans, surveillance of the use of antimicrobial medicines, AMR in the food chain and in the environment. GLASS provides a standardized approach to the collection, analysis, interpretation and sharing of data by countries, territories and areas, and monitors the status of existing and new national surveillance systems, with emphasis on representativeness and quality of data collection. Some WHO regions have established surveillance networks that provide technical support to countries and facilitate enrollment into GLASS.
Dont Miss: Should I Take An Antibiotic For Bronchitis
Also Check: Is Diflucan For Yeast Infection
How Dental Insurance Can Help
Dental emergencies happen. Even if you are practicing good dental hygiene and you take care of your teeth, you can still end up with an infected tooth that needs to be dealt with right away. Dental insurance can help cover the costs of things like X-rays, exams, and other treatments, as well as more expensive care like root canals.
This is not dental care advice and should not be substituted for regular consultation with your dentist. If you have any concerns about your dental health, please contact your dentists office.
You May Like: When To Get Meds For Sinus Infection
Surrounding Bone Gets Infected
The bones in our face are unable to tolerate the presence of an infection for a long time.
Leaving an infection to spread to your facial bones may eventually necessitate surgical removal to stop it.
Even in minor cases, a tooth infection can cause the bone structures of your jaw to weaken, making it hard to support your teeth.
Don’t Miss: Can A Bladder Infection Stop Your Period
Antibiotic Use In Pediatric Dentistry
Anatomical and physiological differences between children and adults such as the amount of their body water and fat, the maturation of the immune system, the volume of protein, and the level of liver enzymes should be considered while prescribing antibiotics for children . Dentists treat children with antibiotics to reduce the risk of bacteremia caused by dental infections however, antibiotic therapy should not be used as an alternative method for elimination of an infection source . Furthermore, antibiotic resistance owing to inappropriate use, prescribing antibiotics in the wrong situation and for a too long period in children is a global concern . Therefore, dental practitioners should be aware of proper antibiotic choices and indications of antibiotic therapy for children under 13 years . Common types and forms of antimicrobial agents used in pediatric dentistry are listed in Tables Tables22 and and33.
Can A Tooth Abscess Go Away On Its Own
A tooth abscess is a specific type of dental abscess called a periapical abscess. It starts as an infection inside the tooth and moves into the area below the tooth. It will not go away on its own. If the abscess ruptures, youll feel immediate pain relief, but you should still seek dental treatment for the underlying infection.
You May Like: How To Heal Infected Tooth Naturally
Selection Of Study Group
The study group comprised patients who, for behavioral reasons , underwent dental extractions under general anesthesia in the Santiago de Compostela University Hospital from January 2003 to December 2004. The following exclusion criteria were applied: age under 18 years receipt of antibiotics in the previous 3 months routine use of oral antiseptics a history of allergy or intolerance to AMX, CLI, or MXF any type of congenital or acquired immunodeficiency or any known risk factor for BE. By applying these criteria, 221 patients were selected and were randomly distributed into four study groups: the control group comprised 53 patients who did not receive any type of prophylaxis before the surgical procedure the AMX group comprised 56 patients who received a standard prophylactic regimen of 2 g of AMX orally 1 to 2 h before anesthesia induction the CLI group comprised 54 patients who received a standard prophylactic regimen of 600 mg of CLI orally 1 to 2 h before anesthesia induction and the MXF group comprised 58 patients who received a prophylactic regimen of 400 mg of MXF orally 1 to 2 h before anesthesia induction.
Randomization was based on a single sequence of random assignments by application of a computer-generated randomization list.
What Accelerates The Emergence And Spread Of Antimicrobial Resistance
AMR occurs naturally over time, usually through genetic changes. Antimicrobial resistant organisms are found in people, animals, food, plants and the environment . They can spread from person to person or between people and animals, including from food of animal origin. The main drivers of antimicrobial resistance include the misuse and overuse of antimicrobials lack of access to clean water, sanitation and hygiene for both humans and animals poor infection and disease prevention and control in health-care facilities and farms poor access to quality, affordable medicines, vaccines and diagnostics lack of awareness and knowledge and lack of enforcement of legislation.
Recommended Reading: Will Teladoc Treat Ear Infection
Bone And Joint Infections
The Oral versus Intravenous Antibiotics for Bone and Joint Infection trial was conducted at multiple centres across the UK.16 It compared early switching from intravenous to oral therapy to continuing intravenous antibiotics for at least six weeks. It included all adults with suspected bone and joint infections, irrespective of surgical intervention or antibiotic choice, who were planned to receive at least six weeks of antibiotic therapy. Comparing the outcomes at one year suggested that appropriately selected oral therapy is non-inferior to intravenous therapy. However, there are several important caveats:
- the trial was not powered to evaluate the outcome between different types of infection
- Gram-negative infections were under-represented
- most patients had surgical management of the infection
- rifampicin was used as a treatment option in approximately one-third of the cohort
- the clinicians managing the patients were specialist-led teams.
Although the events were not necessarily related to the antibiotics, one in four patients experienced a serious adverse event. This shows that ongoing monitoring is still required even with an oral antibiotic regimen.16,17 Further studies are required to look more closely at the different types of infection and the varying antibiotic regimens. Ideally these trials should be performed in the Australian healthcare system.
Dont Miss: Antibiotics To Treat Tooth Abscess
Endodontic Treatment Of Infection
The objectives for endodontic treatment are removal of the microbes, their byproducts, and pulpal debris from the infected root canal system. This allows a favorable condition for periradicular healing. When a patient has signs and symptoms associated with a severe infection, the canals should be disinfected and the access opening should be sealed to prevent coronal leakage.
In the rare case that there is continual drainage, the access may be left open until the next day to allow the accumulated irritants and inflammatory mediators to decrease to a level that allows the patient to initiate healing. Leaving a tooth open for an extended period of time allows for gross contamination with no further benefit to the patient. When there is localized swelling, increasing in size or associated with cellulitis, an incision for drainage should be considered. Incision for drainage is important to remove purulent materials and other inflammatory mediators. Drainage improves circulation to the infected tissues and increases delivery of the antibiotic to the area. Patients requiring extra oral drainage or hospitalization should be referred to an oral surgeon.
When a patient develops signs and symptoms of a severe endodontic infection, adjunctive antibiotics may be considered .
Antibiotics are not indicated in an otherwise healthy patient for a small localized swelling without systemic signs or symptoms of an infection .
| TABLE 1: Indications for Adjunctive Antibiotics |
|---|
|
Don’t Miss: Epstein Barr Virus Infection Symptoms