What Is The Impact Of Hiv On Racial And Ethnic Minorities In The Us
HIV can affect anyone regardless of sexual orientation, race, ethnicity, gender, age, or where they live. However, in the United States, some racial/ethnic groups are more affected than others, given their percentage of the population. This is because some population groups have higher rates of HIV in their communities, thus raising the risk of new infections with each sexual or injection drug use encounter. Additionally, a range of social, economic, and demographic factors such as stigma, discrimination, income, education, and geographic region can affect peoples risk for HIV.
Black/African American and Hispanic/Latino communities are disproportionately affected by HIV compared to other racial/ethnic groups. For example, in 2018 Blacks/African Americans represented 13% of the US population, but 41% of people with HIV. Hispanics/Latinos represented 18% of the population, but 23% of people with HIV.
Source: CDC, Estimated HIV incidence and prevalence in the United States, 20142018.
Certain subpopulations within racial and ethnic minority groups are affected as well. For example, gay, bisexual and other men who have sex with men are by far the most affected group in the US. They account for about 70% of new infections each year, even though they make up only 2% of the population.
According to CDC, in 2018:
For in-depth information about the impact of HIV on different racial and ethnic populations, see these CDC fact sheets:
Read Also: Is Hiv Curable Or Treatable
Hiv Life Expectancy: How Long Can You Live With Hiv Or Aids
The most frequently asked question for HIV-positive patients is how long can you live with HIV? Fortunately, the answer is far more promising than it was 20 years ago. Join Flo as we discuss how advancements in medical technology have altered the prognosis for those living with HIV or AIDS.
A national database containing statistics from 25 states shows that the average HIV life expectancy has more than doubled between 1996 and 2005. The bump from 10.5 to 22.5 years after diagnosis can be attributed to vast improvements in drug therapy and related approaches. However, experts still say this is only an average, and plenty of other circumstances must be taken into account regarding HIV life expectancy.
Dont Miss: Blood Test For H Pylori Infection
Since 2017 Public Health England Has Published Data On Trans People Accessing Hiv Care And Those Newly Diagnosed With Hiv
Headlines
- The majority of trans people accessing HIV care are trans women. In 2019, 111 trans women, 31 trans men and 7 gender diverse people were accessing HIV care in England.
- Trans people aged 35-49 are the largest group in terms of age.
- The majority of trans people accessing HIV care are white , with 47 trans people of other or mixed ethnicity making up the second largest group.
- Nearly all of the trans people accessing HIV care in 2019 acquired HIV through sex between men.
Also Check: How Soon Can You Transmit Hiv After Being Infected
The Importance Of Support Services
Living with HIV presents certain challenges, no matter what your age. But older people with HIV may face different issues than their younger counterparts, including greater social isolation and loneliness. Stigma is also a particular concern among older people with HIV. Stigma negatively affects peopleâs quality of life, self-image, and behaviors, and may prevent them disclosing their HIV status or seeking the health care or social services that many aging adults my require. HIV care.
Therefore, it is important for older people with HIV to get linked to HIV care and have access to mental health and other support services to help them stay healthy and remain engaged in HIV care. You can find support services through your health care provider, your local community center, or an HIV service organization. Or use the HIV Services Locator to find services near you.
Key Messages About Covid
Widespread vaccination is a critical tool to help stop the pandemic. Here are three key messages we need to share:
- Everyone over 12 years of age, regardless of HIV status, get vaccinated.
- Those with advanced HIV disease and/or not on medications, get a third dose of the vaccine.
- Those in HIV care and treatment who are virally suppressed, talk with your health care provider about the need for an additional dose.
Harold J. Phillips, Director, White House Office of National AIDS Policy
Read Also: How Long Can Hiv Live Outside The Body
Also Check: Cvs Minute Clinic Kidney Infection
Estimates Number Of New Hiv Infections
The Agency estimates that 2,242 new infections occurred in Canada in 2018. This estimate is a slight increase from the estimate for 2016 .
The resulting estimated incidence rate in Canada for 2018 was 6.0 per 100,000 population which is a slight increase from the estimate for 2016 .
Figure 8. HIV incidence: Estimated annual number of new HIV infections in Canada
This graph shows the point estimates of new HIV infections by year with each associated plausible ranges for point estimates. The vertical axis shows the estimated number of new HIV infections per year, with the low and high ranges. The horizontal axis shows the calendar years.
| Year |
|---|
| gbMSM-PWID | 2.7% |
Among the estimated new infections in 2018, an estimated 1,109 were among gay, bisexual and other men who have sex with men , representing just under half of all new HIV infections in 2018, despite representing approximately 3-4% of the Canadian adult male population. Although the gbMSM population continues to be over-represented in new HIV infections in Canada, the proportion of new infections among this population has decreased compared to 2016. .
Three hundred and twelve of the estimated new infections in 2018 were among people who inject drugs , accounting for 13.9% of new infections. The proportion of new infections attributed to heterosexuals increased slightly to 34.0% from 31.7% in 2016.
Facts About Hiv: Life Expectancy And Long
Overview
The outlook for people living with HIV has significantly improved over the past two decades. Many people who are HIV-positive can now live much longer, healthier lives when regularly taking antiretroviral treatment.
Kaiser Permanente researchers found that the life expectancy for people living with HIV and receiving treatment increased significantly from 1996 on. Since that year, new antiretroviral drugs have been developed and added to the existing antiretroviral therapy. This has resulted in a highly effective HIV treatment regimen.
In 1996, the total life expectancy for a 20-year-old person with HIV was 39 years. In 2011, the total life expectancy bumped up to about 70 years.
The survival rate for HIV-positive people has also dramatically improved since the first days of the HIV epidemic. For example,
, a person with undetectable levels of HIV in their blood isnt able to transmit the virus to a partner during sex.
Between 2010 and 2014, the annual number of new HIV infections in the United States fell by
Read Also: 7 Day Yeast Infection Treatment
Functional Limitations And Frailty
In the geriatrics literature, the well-described frailty phenotype is regarded as a loss of functional homeostasis that leaves a person unable to effectively recover from various stressors and is associated with poor health outcomes, including excess mortality . Ultimately, the cumulative burden of comorbidities and their respective therapies, as described above, may lead to frailty in HIV-infected persons. Indeed, based on a variety of definitions, the prevalence of frailty or a frailty-like syndrome has been reported in 519% of HIV-infected cohorts . Initial studies among HIV-infected populations describe the higher prevalence of frailty in persons with the deepest immune compromise, and subsequent studies have continued to demonstrate an association between HIV serostatus and frailty, regardless of effective antiretroviral therapy . In addition to the syndrome of frailty, impairment in objective measures of physical function is also apparent. Compared with demographically similar non-HIV-infected adults, HIV-infected persons appear to experience early impaired physical function that ranges from more subtle impairments at a high level of functioning, such as lower peak exercise capacity , to more severe impairments such as difficulty completing a quarter-mile walk or a short physical performance battery .
Is It Safe For Children With Hiv To Receive Routine Immunizations
-
MMR, or measles, mumps, and rubella vaccine, is safe to give to children with HIV, unless they have a severely weakened immune system.
-
DTaP/Td vaccine is safe to give to infants and children with HIV.
-
Hib and Hep B vaccines are safe to give to children with HIV.
-
Hepatitis A and B vaccines are safe to give to HIV-positive children.
-
VZIG should be considered for known HIV-positive children, depending on their immune status.
-
A yearly influenza vaccine is recommended for children with HIV, as well as any individual living in the same household as a child with HIV. There are two types of influenza vaccine children and adults with HIV should receive the “shot” form of the vaccine–not the nasal spray form, as it contains a live virus. Pneumococcal vaccine can be safely administered to age-appropriate HIV-infected children.
Always consult with your child’s doctor regarding immunizations for an HIV-infected child.
Also Check: Ear Infection Hurts So Bad
How Have Deaths From Hiv/aids Changed Over Time
Global deaths from HIV/AIDS halved within a decade
The world has made significant progress against HIV/AIDS. Global deaths from AIDS have halved over the past decade.
In the visualization we see the global number of deaths from HIV/AIDS in recent decades this is shown by age group. In the early 2000s 2004 to 2005 global deaths reached their peak at almost 2 million per year.
Driven mostly by the development and availability of antiretroviral therapy , global deaths have halved since then. In 2017, just under one million died from the disease.
You can explore this change for any country or region using the change country toggle on the interactive chart.
HIV/AIDS once accounted for more than 1-in-3 deaths in some countries, but rates are now falling
Global progress on HIV/AIDS has been driven by large improvements in countries which were most affected by the HIV epidemic.
Today the share of deaths remains high: more than 1-in-4 deaths in some countries are caused by HIV/AIDS. But in the past this share was even higher.In the visualization we see the change in the share of deaths from HIV/AIDS over time. From the 1990s through to the early 2000s, it was the cause of greater than 1-in-3 deaths in several countries. In Zimbabwe, it accounted for more than half of annual deaths in the late 1990s.
We see that over the past decade this share has fallen as antiretoviral treatment has become more widely available.
Children living with HIV
New HIV infections of children
Hiv/aids Is One Of The Worlds Most Fatal Infectious Disease
Almost 1 million people die from HIV/AIDS each year in some countries its the leading cause of death
HIV/AIDS is one of the worlds most fatal infectious diseases particularly across Sub-Saharan Africa, where the disease has had a massive impact on health outcomes and life expectancy in recent decades.
The Global Burden of Disease is a major global study on the causes of death and disease published in the medical journal The Lancet.1 These estimates of the annual number of deaths by cause are shown here. This chart is shown for the global total, but can be explored for any country or region using the change country toggle.
In the chart we see that, globally, it is the second most fatal infectious disease.
According to the Global Burden of Disease study, almost one million people died from HIV/AIDS in 2017. To put this into context: this was just over 50% higher than the number of deaths from malaria in 2017.
Its one of the largest killers globally but for some countries particularly across Sub-Saharan Africa, its the leading cause of death. If we look at the breakdown for South Africa, Botswana or Mozambique which you can do on the interactive chart we see that HIV/AIDS tops the list. For countries in Southern Sub-Saharan Africa, deaths from HIV/AIDS are more than 50% higher than deaths from heart disease, and more than twice that of cancer deaths.
Read Also: Saline Solution For Eye Infection
What The Current Research Says
At the time of the introduction of highly active antiretroviral therapy in 1996, the average life expectancy of a 20-year-old newly infected with HIV was 10 years. With a new generation of drugs that are not only safer but more effective, those numbers have leaped significantly.
According to research from the longstanding North American AIDS Cohort Collaboration on Research and Design , a 20-year-old started on HIV therapy today can expect to live into their early 70s.
With the life expectancy of the general U.S. population hovering around 77 years, this means that people treated early for HIV can enjoy near-normal life expectancies. Some can expect to do much better.
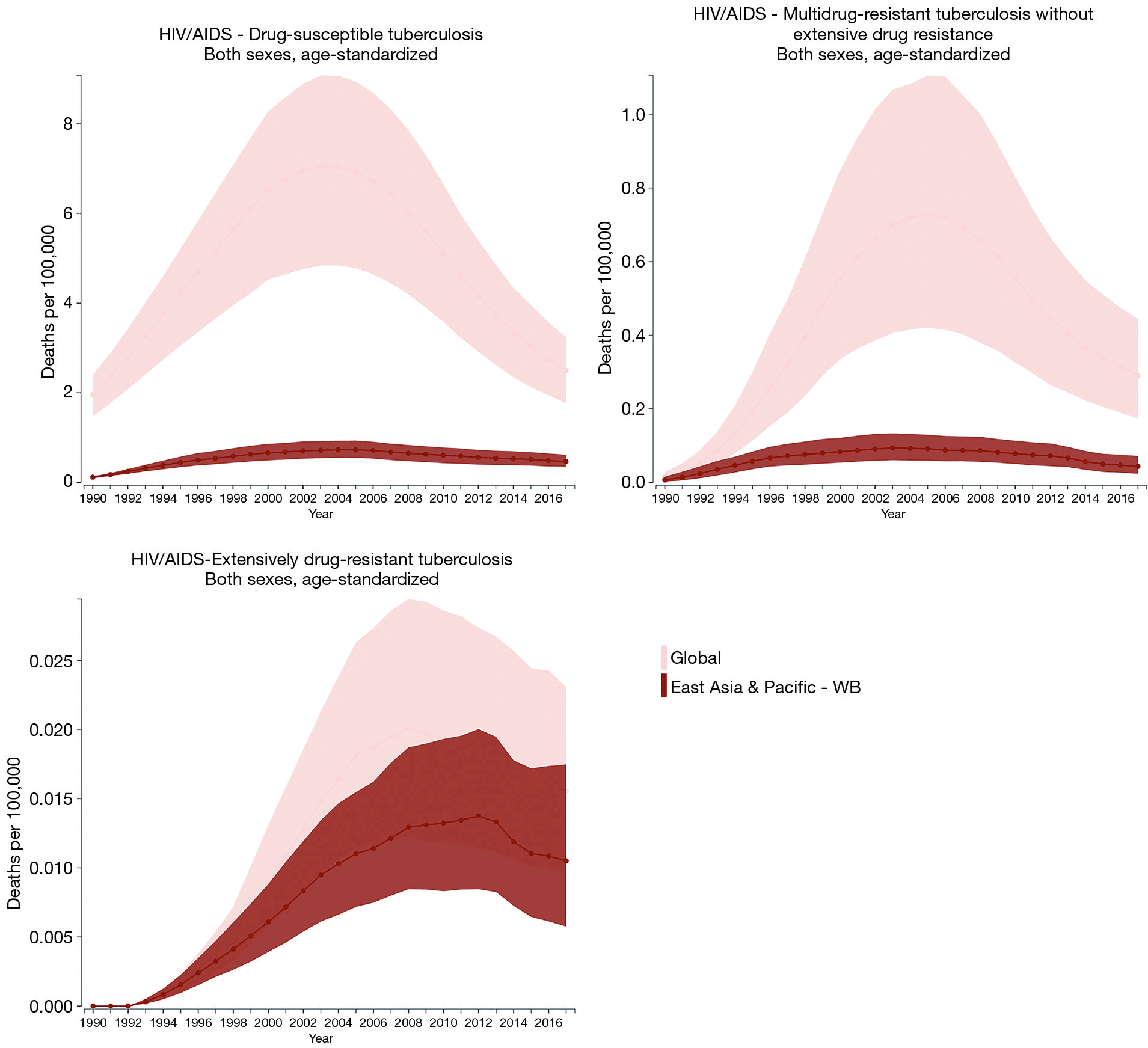
Hiv And Tuberculosis In South Africa
South Africa has the worlds sixth largest tuberculosis epidemic, and the disease is the leading cause of death in the country.120 South Africas HIV epidemic fuels the TB epidemic because people living with HIV are at a far higher risk of developing TB due to weakened immune systems. It is estimated that 60% of people living with HIV in South Africa are also co-infected with TB. In 2017 there were 193,000 new cases of TB among people living with HIV and 56,000 people living with HIV died due to a TB-related illness.121
In light of this, the South African National AIDS council combined the HIV and STI strategy with the national TB strategy to improve the integration of these two services. One of the aims of this strategy is to get more people living with HIV on isoniazid preventative therapy , a preventative medicine for TB.122 But as of 2017, only around half of people living with HIV in the country had access to IPT.123
The TB treatment success rate has improved in recent years, and stood at 83% in 2016.124
We cannot fight AIDS unless we do much more to fight TB.
Dont Miss: Where Did Hiv Aids Begin
Recommended Reading: Swollen Mouth From Tooth Infection
Life Expectancy With Hiv: How Long Can Someone Live With Hiv
The research on HIV, its symptoms and causes has been done since years, and the same is in continuation. As of now there is no cure for HIV or AIDS, but there are medications and treatment which can make the remaining life of the patient easier, and extend the duration of the patients life. As, HIV can be distinguished or categorized in three different stages, the life expectancy for different stage is different and also depends upon the infected percentage of your immune system.
As per the statistics reported from 1996-1997, an HIV positive person has a life expectancy of almost 19 years, say if the person has been found infected at the age of 20, he shall live further till he is 39-40 years old. However, there has been an immense inclination found in life expectancy since then, and as reported in the year 2011, the increased life span of 19 years was found to extend up to 53 years, where supposedly if a person is found HIV positive at the age of 20, he can live as long as 73-74 years old.
A HIV positive woman has lesser life expectancy than men, but with the advanced treatment methods, the life expectancy in the current scenario has been increased, where initially it was reported to be around 38 years old and now has been found to extend up to 49 years old. The increase in the life expectancy of a person with HIV has increased thanks to the advanced medicines and treating methods.
You May Like: How To Get Rid Of Tooth Infection Naturally
The Global Distribution Of Deaths From Hiv/aids
In some countries HIV/AIDS is the cause of more than a quarter of all deaths
Globally, 1.5% of deaths were caused by HIV/AIDS in 2019.
This share is high, but masks the wide variations in the toll of HIV/AIDS across the world. In some countries, this share was much higher.In the interactive map we see the share of deaths which resulted from HIV/AIDS across the world. Across most regions the share was low: across Europe, for example, it accounted for less than 0.1% of deaths.
But across some countries focused primarily in Southern Sub-Saharan Africa the share is very high. More than 1-in-4 of deaths in South Africa were caused by HIV/AIDS in 2019. The share was also very high across Botswana Mozambique Namibia Zambia Kenya and Congo .
Death rates are high across Sub-Saharan Africa
The large health burden of HIV/AIDS across Sub-Saharan Africa is also reflected in death rates. Death rates measure the number of deaths from HIV/AIDS per 100,000 individuals in a country or region.
In the interactive map we see the distribution of death rates across the world. Most countries have a rate of less than 10 deaths per 100,000 often much lower, below 5 per 100,000. Across Europe the death rate is less than one per 100,000.
Across Sub-Saharan Africa the rates are much higher. Most countries in the South of the region had rates greater than 100 per 100,000. In South Africa and Mozambique, it was over 200 per 100,000.
Don’t Miss: Urine Test For Yeast Infection
Age Differences In Hiv Transmission
The estimated mean age at infection was 35.6 among peopleclassed as definite sources and 36.9 among recipients already challengingthe assumption that recipients would probably be younger. In 57% of cases therecipient was older than the source, with an average age difference of 2.16years. However, this situation was reversed in men under 30, where on averagethe recipient was nearly nine years younger.
There was a clear and steady increase in the likelihood of thesource being the younger partner as both partners got older. It wascalculated that for every year older a recipient was, the average age of thesource of their infection only grew by 0.28 years .
When the recipient was under 25, their source partner was onaverage ten years older when 25-29, eight years older and when 30-34, fiveyears older. However, the average age difference between pairs aged 35-39 waszero, and after that source partners became younger than recipients two yearsin men aged 40-44, and 11 years among men over 45.
To put this another way: in recipients under 25, 92% of theirsource partners were older than them in 25-29 year olds, 51% in 30-34 yearolds, 47%. But in 35-39 year olds, 35% were younger in 40-44 year olds, 52% wereyounger and in men over 45, 71% were younger. The age at which the agedifference crossed was 38.4.