Why Pips Is Important When Doing Root Canals
So how do we get the bugs out of the tooth and tubules? you might ask. In his pilot study Efficacy of PIPS on root canals infected with Enterococcus Faecalis , Dr. David Jaramillio explores whether the Er :Yag laser in PIPS mode is effective in the elimination of bacteria from infected root canals. This research study shows how efficient and effective PIPS is in removing bacteria from the tooth during root canal therapy.
Here is an image from the study showing the tubules devoid of bacteria after treating the tooth with PIPS technology with the Fotona laser. To me as a dentist, this result is nothing short of amazing.
Here is another quote from a different research study. All instrumentation techniques left 35% of the walls untouched. O. Peters, IEJ 2001. In other words, when you are just using files to do root canals 35% of the tooth surface does not get cleaned because the files are not an efficient way of cleaning the canals out. In my opinion, there are bacteria left behind when using hand files and traditional root canal treatment.
In a recent advancement, Fotona has added the SWEEPS mode to do the same thing as PIPS, but do it even better. Please see the video above once again and you will see the action of PIPS and SWEEPS side by side. SWEEPS is like PIPS on steroids. Its like a tsunami of activity, an endodontist commented when its used in conjunction with root canal therapy.
Avoiding A Missed Root During A Root Canal
by soniachopra | Jun 24, 2022 | Endodontics |
Whats the best way to give root canals a bad reputation? A missed root during root canal.
As an endodontist and educator, one of my primary responsibilities is to continue to dispel the harmful myths that have emerged and persisted around root canals. For decades, the dental community has had to contend with literature and even full-length documentaries that drive fear around root canals and what they do to our bodies. Most of these false claims are grounded in the idea that root canals never truly healthey will always be home to harmful bacteria that will only cause further pain and infection.
If that were true, I would understand why so many patients assume theyll need to have their teeth extracted! Fortunately, though, all those fears about root canals are totally unfounded. As every trained endodontist knows, a properly performed root canal is perfectly safe, and has the added benefit of balancing out a patients microbiome whilesaving their natural teeth.
However, as with any medical procedure, it is true that a failed root canal can cause complications later on. Thats why its imperative for any dentist to stick to the two cardinal rules of root canals:
- Find every single canal
- Get to the end of every single canal
What Causes Root Canal Infections
There are many reasons why a tooth can have an infection after a root canal. These include:
- The shape of your root canals can be very complicated and areas of infection may go undetected in the first procedure.
- Your tooth could have narrow or curved canals that werent fully cleaned and disinfected during the root canal.
- Your tooth may also have extra, accessory canals that could be housing bacteria which may reinfect a tooth.
- If the placement of the crown or permanent restoration is delayed following treatment, it could allow harmful bacteria back into your tooth.
- Your tooth may get a new cavity after treatment, or become cracked or damaged, leading to a new root canal infection.
To treat a root canal infection, a root canal retreatment may be recommended to give your tooth a second chance. This retreatment is similar to the first root canal procedure.
In retreatment, your dentist or root canal specialist will typically do the following:
Read Also: Do Antibiotics Kill Tooth Infection
One Size Does Not Fit All
After reading the above, Im sure you can see that with root canals, one approach does not fit every situation or patient. its impossible to generalize about whats best for each individual. Every situation is different, including patients overall oral health, wants, needs, history, symptoms and the condition of the tooth itself. Many alternative doctors in the holistic and integrative health field believe that every root canal should be extracted no matter what. This, in my experience, is not accurate or realistic, as it takes a very complex issue like health and generalizes one approach for every patient and situation. Conversely, most dentists and root canal specialists recommend that the tooth try to be saved at all costs. This is also not practical or realistic in some cases, as the tooth is clearly not a good prospect for additional treatment.
What Is The Success Rate Of Root Canal Retreatment
Success rates for root canal retreatments are high generally ranging from 80% to 88%. Your prognosis, however, can be affected by the type of treatment your tooth received previously. Its also essential to find an endodontic practice with a high level of experience performing retreat root canals, such as Midtown Endodontist NYC.
Read Also: Is Yellow Snot A Sinus Infection
After The Retreat Is Complete What Will I Need To Do To Keep My Tooth Strong
Youll need a final restoration in the tooth, whether thats a filling or a crown. Usually, this is a crown but in some cases it can be a filling. If the retreat is performed on a tooth that already has a crown and that crown hasnt broken during the retreat, we can seal the crown with a filling as your final restoration.
In some cases, the original crown will break during your procedure, but this is not the most common outcome. If that happens, you will need a new crown to protect your tooth.
Boil Or Pimple On The Jaw
Active abscesses create cysts inside of the bone and gum tissues, creating a fistula or fluid-filled pimple on your gums. These fistulas can range from small, tiny sores to large boils. On your X-ray, there may even be a hollow-looking cyst inside of the bone next to your tooth root. A fistula can come and go, depending on whether the pus drains out of it or the infection goes down. But the source of the swelling wont heal itself, so dont make the mistake of thinking that the problem has resolved itself.
Also Check: Is Bactrim Good For Tooth Infection
To Retreat Or Not: A Decision Matrix
Endodontic therapy enjoys a high survival rate of 97% when properly performed. In fact, the survival rates of endodontic treatment and implant placement are the same. However, as in any medical procedure, a certain percentage of treated cases will fail. Deciding on whether to pursue retreatment or not depends on a variety of factors. The patient’s needs, age, and clinical expectations are all important considerations. Tooth retention is the best possible treatment when possible, and retreatment can ultimately be the most time- and cost-effective option. Time, cost, and more flexible clinical management indicate that endodontic retreatment procedures should always be performed first unless the tooth is judged to be untreatable. However, it is important to keep in mind the concept that not all retreatments are created equal. The advent of single-tooth implants has given a viable alternative to hero-dontics, allowing treating specialists to focus on more successful retreatment cases and decide against treatment on cases that may not have a favorable prognosis.
Assess the reasons for initial treatment failure
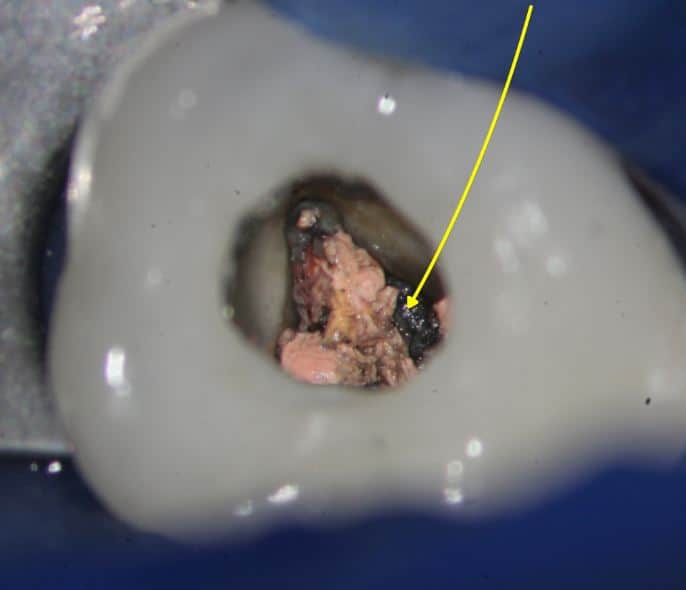
Missed canal anatomy cases …
Missed third canal in upper first premolar
Strategic tooth assessment
Tooth that is a terminal abutment
Periodontal assessment
Iatrogenic error
The delicacy of root canals make iatrogenic events an unfortunate occurrence. The question the clinician must ask when presented with a failing case due to iatrogenic error is: Is it repairable?
What To Do About A Failed Root Canal
There are only two options if you have a failed root canal: re-treat the tooth or have it extracted.
Root canal retreatment is almost always performed by an endodontist. Even more experienced general dentists typically refer their patients to an endodontic office because of the resources they have on hand. Retreatment can help you avoid an extraction, manage pain, and preserve as much tooth structure as possible.
Ideally, your dentist and endodontist will want to try to maintain your natural tooth. But sometimes a dental extraction cant be avoided. Such as severe fractures extending through the root tips or aggressive decay that has worked its way well into the majority of the tooth. In some instances, the inside of the tooth will begin to resorb leaving little to nothing left to repair. An extraction is usually recommended in any of these scenarios. But at that point, youll also need to plan for replacing your tooth with something like a bridge or dental implant.
Read Also: How Long Does Take To Get Rid Of Yeast Infection
Description Of The Condition
Root canal treatment for the infected pulp of a tooth aims to eradicate pathological microbiota and prevent future infection within the root canals. Root canal treatment should obtain proper root canal shape, so an efficient cleaning can be performed before threedimensional filling . In recent years, the number of people seeking root canal treatment has dramatically increased because a conservative approach is preferred over tooth extraction .
Even when an adequate standard of treatment is performed, failures may occur, owing to the anatomical characteristics of the root canal system and to the presence of peculiar noxious factors within the inflamed tissue . The persistence of microorganisms in the root canal system may induce an inflammatory and immune response in the periradicular tissues, resulting in local bone destruction. Furthermore, contamination of the periradicular tissues and of the filling material by microorganisms may initiate a foreign body reaction, thereby impairing tissue healing.
Large crosssectional studies from different countries have reported that the prevalence of apical periodontitis and other posttreatment periradicular disease can exceed 30% of all rootfilled teeth , suggesting a considerable need for treatment of this condition.
Furthermore, the presence of cysts, extraradicular infections or other conditions not properly related to a dental pathosis, such as foreign body reactions, could be an indication for rootend resection.
Description Of The Intervention
Although success rates up to 97% have been reported for the initial root canal treatment , failure may occur after treatment, mainly owing to incomplete removal of the pathogenic microbiota. In cases of persistent apical periodontitis or another posttreatment periapical disease in a previously treated tooth, as a consequence of the failure of primary root canal treatment to permanently eradicate the infection, two possible treatment alternatives exist to preserve the tooth: root canal retreatment and rootend resection.
Root canal retreatment has the same aim as primary treatment of infected root canals: complete elimination of microorganisms and hermetic sealing with biocompatible materials. This is accomplished by removal of root canal filling material, disinfection of the root canal system and sealing of root canals .
However, when root canal retreatment is not feasible, when it fails, when it is unlikely that it can improve on the previous result or when biopsy of the periapical lesion is necessary, a surgical intervention consisting of rootend resection with or without rootend filling might be indicated and represents the last chance for avoiding tooth extraction.
Rootend resection consists of surgical removal of a periapical lesion, resection of the apical portion of the root, disinfection and sealing of the apical portion of the remaining root canal .
Recommended Reading: Is Zpack Good For Tooth Infection
What Are Root Canal Infections
Teeth arent solid all the way through theyre made up of layers. The hard, outer surface of a tooth is called enamel. The inner layer is called dentin and is a porous, almost sponge-like tissue. At the center of each tooth is a collection of soft tissue called pulp.
The pulp contains the nerves and blood vessels that allow the tooth to grow. Its full of cells called odontoblasts that keep the tooth healthy.
A root canal removes the pulp of a tooth thats been infected or damaged by tooth decay or other injuries. Root canals can save teeth and are considered very safe.
Root canal infections arent common, but theres a small chance of a tooth becoming infected even after a root canal is performed.
What Are My Treatment Options
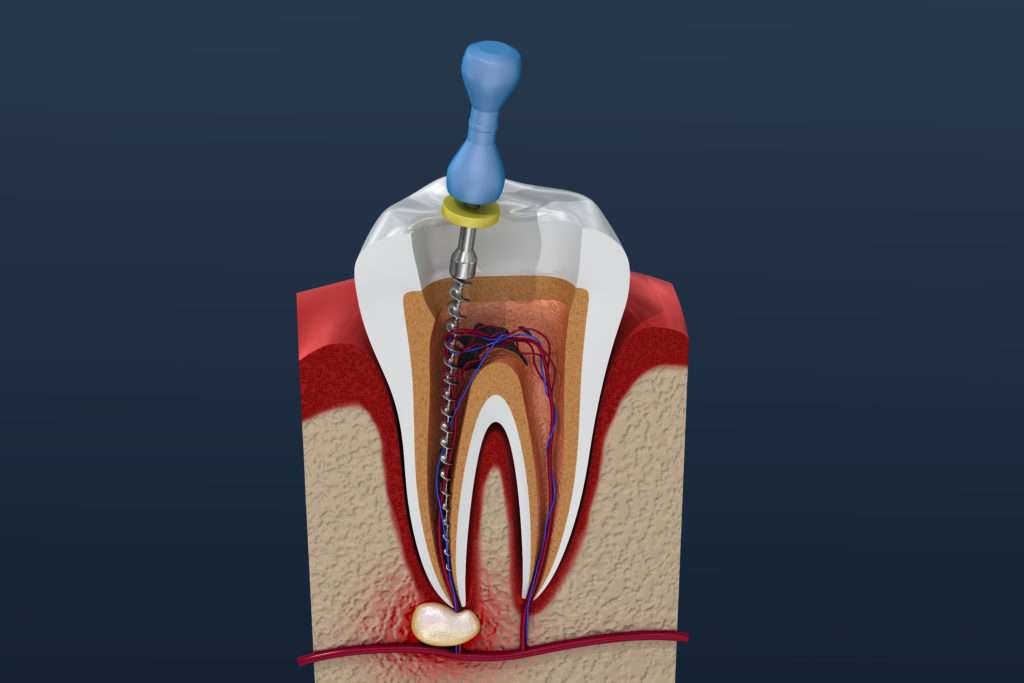
When you opted for your initial root canal treatment, your dentist probably explained that the only other treatment option was to remove the tooth. Now that you are experiencing pain in that tooth, your endodontist might suggest retreatment or endodontic surgery. In endodontic surgery, an incision is made at the tip of the tooth’s root to remove the infected portion surgically. This procedure is called an apicoectomy. Besides endodontic retreatment or surgery, the only other alternative is to have the tooth extracted.
Also Check: Mac Os Is Infected With Spyware
Infected Root Canal Symptoms
A root canal infection may occur not just from a damaged tooth, but after receiving root canal treatments. Early warning signs of a tooth infection after root canal treatment include:
- Pain when eating hot or cold food
- Pain when chewing or biting
- A loose tooth
Over time, these old root canal infection symptoms may disappear as the pulp dies. However, this does not mean the problem goes away. Eventually, the infection after root canal treatment will begin exhibiting new symptoms, which might include:
- Darkening of the tooths color
- Swelling in the face
How Can A Root Canal Treated Tooth Get Reinfected
Technically, a pulp-less root canal cannot be infected anymore because the infection can only happen on living tissue.
Having said that, a root canal treated tooth is still supported by surrounding living tissue, eg. gum and jawbone. An infection can still happen in two scenarios:
To suggest an analogy, a decorative plant will not be damaged by bugs. However, the bugs could still invade the soil supporting the plant, giving trouble to you.
Read Also: How To Treat Male Yeast Infection Over The Counter
Next Steps: Find A Qualified Endodontist
We hope this article answered some of your questions regarding what happens if a root canal fails? If you or a loved one are suffering from a failed root canal, ask your dentist to refer you to a skilled endodontist.
If you live in the Charlotte, NC area, we urge you to consider Ballantyne Endodontics. We have had the privilege of treating Charlotte residents since 2008. Our founder, Endodontist Sonia Chopra, D.D.S., knows first-hand what it is like to need retreatment for a root canal, and she has devoted her professional life to restoring health and balance for her patients.
Why Do I Need Another Endodontic Procedure
As occasionally happens with any dental or medical procedure, a tooth may not heal as expected after initial treatment for a variety of reasons:
- Narrow or curved canals were not treated during the initial procedure.
- Complicated canal anatomy went undetected in the first procedure.
- The placement of the crown or other restoration was delayed following the endodontic treatment.
- The restoration did not prevent salivary contamination to the inside of the tooth.
In other cases, a new problem can jeopardize a tooth that was successfully treated. For example:
- New decay can expose the root canal filling material to bacteria, causing a new infection in the tooth.
- A loose, cracked or broken crown or filling can expose the tooth to new infection.
- A tooth sustains a fracture.
Also Check: Can Yeast Infection Cause Painful Urination
What Is A Root Canal
The term root canal is a common shortening of root canal treatment or root canal infection but it actually also refers to the pulp inside the teeth.
An infected root canal is when the center of a tooth becomes exposed and bacteria move in. In this instance, it may need the pulp removed or the tooth may need to be extracted. Its important to act fast on infected tooth root canal treatment because once bacteria get inside the root canal of a tooth , it is extremely hard to stop it from continuing to grow. Over time, the tooth begins to decay and may not be able to be saved.
Can a root canal get infected? is a question often asked by those who have already had treatment, and it could mean one of two things. In terms of the root canal itself or the center of the tooth, then yes. A root canal can get infected if there is a cavity or decay that has reached the center of the tooth, or if there has been trauma or damage to a tooth. It may also happen when a filling fails. Once bacteria find a way in, it can begin to infect the center of the tooth.
The question might also refer to a root canal treatment, which is a procedure that removes bacteria from the root canal system of a tooth. A root canal treatment can get re-infected but thankfully, Living Well Dental has the best dentists, years of experience, and the expertise required to ensure the chances of that happening are very low.